3-D Printing May Help TAVR Operators Avoid Paravalvular Leak
In a small, retrospective study, 3-D printing and computer modeling were able to accurately predict leaks confirmed after TAVR using echocardiography.
SAN DIEGO, CA—Despite rapid advances in TAVR technology, paravalvular leak (PVL) still remains a problem for many patients, with more serious leaks being linked to worse outcomes down the road. A new study supports a role for 3-D printing as a means of helping operators predict areas where an ill-fitting stent frame could lead to leaks.
“Although we’ve made huge improvements in reducing PVL . . . there are still significant barriers with some of the self-expandable valves,” said Sergey Gurevich, MD (University of Minnesota, Minneapolis, MN), in an interview with TCTMD.
Even with 3-D multislice CT, operators may have a difficult time predicting which patients will have PVL and whether it will be mild, moderate, or severe. “Right now, we rely on valve technology to assist us,” Gurevich added. “But it would be nice to know what to expect, before we go in, to help us with valve selection.”
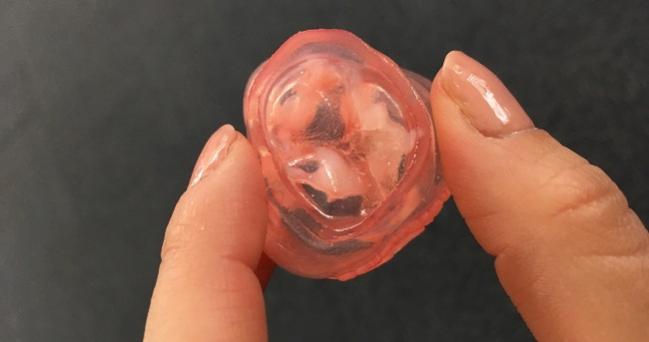
To that end, he and his colleagues conducted a small, retrospective study of six patients who developed PVL after TAVR for severe, calcific aortic stenosis. The researchers analyzed preprocedure CT images to create 3-D printed models of each patient’s aortic root. They then “implanted” each of those models with the device the patient received—all Sapien XT (Edwards Lifesciences). Five patients received the 26-mm valve, and one received a 23-mm valve.
The implanted 3-D models were then rescanned with CT, and these images were compared with echocardiograms from the patients taken after TAVR. In every case, the fit of the 3-D printed model predicted the leak seen on echo, suggesting that if the modeling had been done prior to the TAVR procedure, the PVL could potentially have been prevented. In most cases, significant calcifications identified on pre-TAVR CT were associated with areas of poor stent apposition. Two patients found to have central aortic insufficiency were suspected to have patient-prosthesis mismatch: one had received the 23-mm XT valve, while the other had a body surface area of approximately 3 m2—more than 50% higher than average.
‘Tip of the Iceberg’ for Personalized Valve Procedures
The research is being presented in a poster session today at the Society for Cardiovascular Angiography and Interventions (SCAI) 2018 Scientific Sessions.
Prior to his presentation, Gurevich told TCTMD that his group is working on building a library of aortic valve geometries that will be analyzed by computational flow dynamics, with the goal of quantifying the amount of leak anticipated. Once enough data have been compiled, he added, most pre-TAVR modeling scenarios can probably be done on a computer without the need of a 3-D printed model like the researchers used in this study. Ultimately, this type of research may even pave the way for custom aortic valves, once the technology has been refined, Gurevich said.
Describing this early work as “the tip of the iceberg,” he observed that it also may be possible to extend this type of personalized approach to other structural interventions, including left atrial appendage closure devices and mitral valves.
Photo Credit: Yael L. Maxwell, TCTMD
L.A. McKeown is a Senior Medical Journalist for TCTMD, the Section Editor of CV Team Forum, and Senior Medical…
Read Full BioSources
Gurevich S. 3D printing and computer modeling to predict paravalvular leak in transcatheter aortic valve replacement. Presented at: SCAI 2018. April 26, 2018. San Diego, CA.
Disclosures
- Gurevich reports no relevant conflicts of interest.


Comments