Belly Fat the Biggest Driver of Obesity-Related CVD, Says AHA
A scientific statement highlights the harmful effects of visceral adiposity even when BMI is normal.
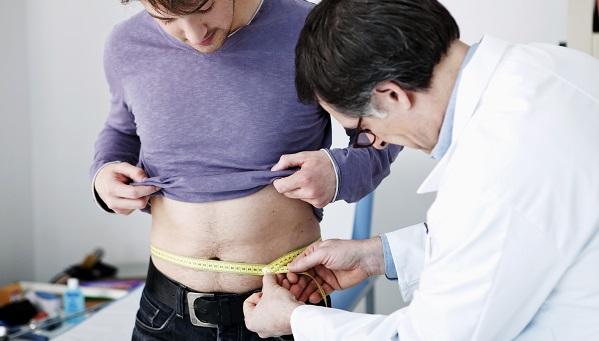
Published April 22, 2021, in Circulation, the statement warns that abdominal obesity and excess fat in the midsection and organs pose the biggest risk to long-term cardiovascular health.
“There has really been a shift in how obesity is viewed,” lead author Tiffany Powell-Wiley, MD, MPH (National Heart, Lung, and Blood Institute, Bethesda, MD), told TCTMD. “It’s being viewed more and more as a complex disease, so we wanted to make sure that we highlighted some of that complexity. One of the big takeaways is that waist circumference is distinct from body mass index [BMI]. Waist circumference is more of a measure of abdominal obesity, or visceral adiposity, and there have been a number of studies over the past 15 years that really highlight the relationship between elevated waist circumference, even in the setting of normal BMI, and cardiovascular risk.”
Several organizations and expert panels, including those from the AHA, the American College of Cardiology, the Obesity Society, and the Endocrine Society, now recommend that waist circumference be measured in addition to BMI. Overweight or obese individuals with low levels of visceral adiposity can have a more-favorable cardiovascular risk profile, which is sometimes referred to as metabolically healthy obesity, while obese patients with excess visceral adipose tissue represent a subgroup of patients at highest CVD risk, according to the experts. To TCTMD, Powell-Wiley said visceral adiposity promotes inflammation, which can lead to detrimental downstream effects, such as the development of atherosclerosis or type 2 diabetes. Physical activity, particularly aerobic physical activity, has been shown to decrease visceral adiposity.
“That can be even without weight loss,” stressed Powell-Wiley. “We really want people to try to follow the recommendations for physical activity, which is 150 minutes per week of moderate-intensity aerobic exercise. Making healthy changes with diet and exercise can have an impact on visceral fat even if you’re not seeing the scale change. Weight loss should not necessarily be the end-all goal.”
For example, one recent meta-analysis showed that both diet and exercise led to reductions in visceral adipose tissue, but exercise alone led to a 6.1% reduction in visceral adipose tissue in the absence of weight loss.
AF and Heart Failure
In addition to the focus on waist circumference, the scientific statement provides an update on the clinical management and treatment of coronary artery disease in obese patients, highlighting the benefits of weight loss as well as reviewing clinical outcomes of obese patients who undergo coronary revascularization with either PCI or surgery.
The experts also highlight the impact of obesity on heart function, including heart failure. Numerous studies have linked obesity to hypertension and left ventricular hypertrophy, which are both risk factors for the development of heart failure. Some of the new treatments that have emerged in recent years for diabetes might also play a role in treating obese patients with HF, according to the AHA. Glucagon-like peptide agonists, such as a liraglutide, and sodium-glucose cotransporter 2 inhibitors have both shown an ability to reduce body weight and to decrease the risk of hospitalizations for HF and cardiovascular death. These agents are currently being tested in number of clinical trials, including in patients who have HF with reduced ejection fraction and those who have HF with preserved ejection fraction (with and without diabetes).
Obesity is also associated with a higher risk of sudden cardiac death and may be responsible for as many as 20% of atrial fibrillation (AF) cases. “We really want to emphasize there is strong data to support weight management as part of the treatment options for atrial fibrillation,” said Powell-Wiley.
Right now, there are still many unknowns, she added, including the potential role of bariatric surgery for reducing the risk of major adverse cardiovascular events in obese patients. Observational studies, including data from the Swedish Obese Subjects study, suggested bariatric surgery can lower the risk of coronary artery disease and cardiovascular mortality, but there is no randomized trial evidence to date. Still, Powell-Wiley said that it’s important for cardiologists to be aware of the “treatment continuum” for obesity. If patients aren’t responding to lifestyle interventions, there are opportunities for pharmacological therapy and even bariatric surgery, she said.
Finally, Powell-Wiley stressed that more research is needed in younger populations to address the rising prevalence of obesity in adolescents. Upstream prevention strategies are needed, she said, as are treatments for younger people with severe obesity. More research is also needed to understand the most effective lifestyle interventions to decrease visceral adiposity and improve cardiovascular outcomes, she said.
Michael O’Riordan is the Managing Editor for TCTMD. He completed his undergraduate degrees at Queen’s University in Kingston, ON, and…
Read Full BioSources
Powell-Wiley TM, Poirier P, Burke LE, et al. Obesity and cardiovascular disease: a scientific statement from the American Heart Association. Circulation 2021;Epub ahead of print.
Disclosures
- Powell-Wiley reports no conflicts of interest.





Comments