Benefits of PCI for STEMI Not Attenuated in Patients With a Cancer History
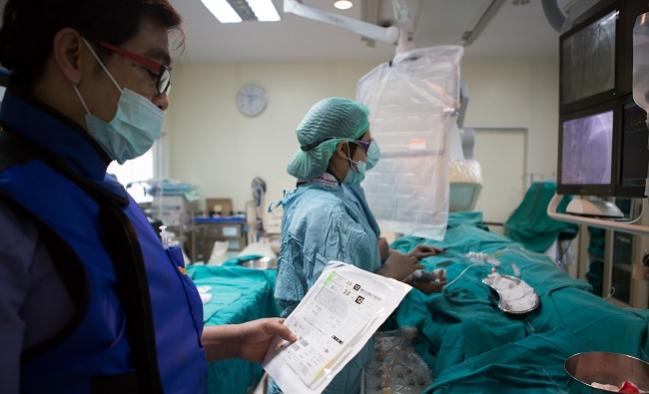
Having a history of cancer does not worsen outcomes for patients with STEMI who undergo primary PCI and should not be a barrier to revascularization and optimal therapy, a new study suggests.
Unfortunately, data on cancer patients treated with PCI are sparse because they are often excluded from randomized trials, and the limited information that is available is inconsistent in terms of whether they have worse acute and long-term outcomes than those without cancer, said senior author Joerg Herrmann, MD (Mayo Clinic, Rochester, MN), in an interview with TCTMD.
In the study led by Feilong Wong, MD (Mayo Clinic), and published online December 1, 2016, ahead of print in the Mayo Clinic Proceedings, the researchers followed 2,346 STEMI patients treated between November 2000 and October 2010 at their institution. Of these, 261 patients (11.1%) had a history of malignancy, a proportion that Herrmann noted is consistent with what has been previously reported in the DAPT Study.
From a cardiovascular standpoint, mortality was not increased among the group of patients with a cancer history compared with those without cancer either during hospitalization or in the 5 years following primary PCI, despite the former having a greater likelihood of hospitalization for heart failure. A subgroup of patients who had been diagnosed with cancer within the 6 months prior to experiencing STEMI, however, had in-hospital mortality rates that were seven times higher than patients without cancer, and they also had nearly triple the risk of dying from noncardiac causes over the long term.
At 5 years, patients with cancer had higher rates of all-cause (34.2% vs 16.8%; P < 0.001) and noncardiac death (30.0% vs 11.0%; P < 0.001) than those without cancer. “It’s absolutely clear that the mortality is solely due to cancer-related death in this group,” Herrmann said. “That alone is a very striking finding.”
He added that a main message of the study is that patients with cancer and STEMI benefit as much from intervention as any other group of patients.
An unusual feature of the study is that it included information on DNR/DNI orders, which were found to be similar among patients with and without cancer who died during the study (11.8% and 11.5%, respectively). According to Herrmann, the implication is that despite having cancer, patients were receiving optimal cardiac treatment and showed willingness to participate in that treatment. The authors also note that conservative treatment with suboptimal cardiovascular care in cancer patients could do more harm than good by limiting their future cancer treatment options, including pharmacologic and surgical therapies.
“These data should be reassuring for patients and physicians, because once you know a patient has a cancer diagnosis you almost take a step back and think about the bigger picture [in terms of] what will we accomplish by intervention,” Herrmann said. Taken together with other studies in the literature, he added, it would appear that those in whom optimal cardiac interventions should not be pursued “are more the exception than the rule.”
Cardio-Oncology Use Advocated
Although some chemotherapy regimens are known to have the potential for cardiovascular toxicity, the current study found no association between any specific chemotherapy regimen or radiation and increased risk of death.
To TCTMD, Herrmann said another observation of importance from the current study is that patients with a history of cancer were more likely to have shock at presentation and to have received intra-aortic balloon pumps. These findings are in line with the hypothesis that a cancer history may lower cardiovascular reserve. But they also suggest that these patients can benefit significantly from intervention given their low risk of cardiac mortality, he said.
Despite the reassuring nature of the study, Herrmann noted that the data also point to the fact that cancer patients with cardiovascular disease need to be treated with a multidisciplinary approach. The emerging field of cardio-oncology is vital to this effort, he observed.
“These patients need both oncology and cardiology care. If we work together, patients will see the best outcomes,” Herrmann said. “We are seeing more and more data supporting the concept of cardio-oncology. This can only be a good thing for our patients and for the doctors who are treating them.”
L.A. McKeown is a Senior Medical Journalist for TCTMD, the Section Editor of CV Team Forum, and Senior Medical…
Read Full BioSources
Wang F, Gulati R, Lennon R, et al. Long-term noncardiac (but not cardiac) mortality after primary percutaneous coronary intervention for acute ST-segment elevation myocardial infarction. Mayo Clin Proc. 2016;Epub ahead of print.
Disclosures
- Herrmann reports no relevant conflicts of interest.


Comments