Cardiologists Treating Syrian Refugees Call Missions an ‘Addictive’ Passion That Saves Lives
Cardiac diseases tend to get pushed “to the background” given the dire health needs of refugees. Now medical volunteers are trying to change that.

For a Syrian refugee who doesn’t know the next time his family will eat, if his home is still standing, or whether stability will ever return to his beleaguered country, a diagnosis of coronary artery disease or valvular regurgitation may seem inconsequential. Now, however, a dedicated team of cardiologists and surgeons has banded together to treat these conditions on the margins of the 7-year old civil war that has left an estimated half million dead.
Zaki Lababidi, MD (Gilbert Cardiology, Gilbert, AZ), who has now gone on two medical missions to Jordan with the nonprofit Syrian American Medical Society (SAMS) and serves as its Arizona chapter president, says his day-to-day clinical duties stateside are merely his “job.”
“Overseas, it’s not a job,” he told TCTMD. “You’re really doing it because of pure humanitarian cause. It just gives you a different feeling.”
Lababidi was born and raised in Damascus, Syria, although he moved to the United States after medical school to pursue internal-medicine and cardiology training. He started working with SAMS in 1998, when it was mainly an educational and networking organization. In 2011 when the Syrian conflict started, SAMS transformed into more of a relief operation, though it continued providing training for those working in the ICU, labor/delivery, and trauma wards. As the humanitarian crisis in the region persisted, it became apparent that the refugees, in additional to having myriad medical conditions related to the crisis, were also dealing with chronic cardiovascular issues and in need of specialized care.
In July 2016, after securing donated stents from a large device manufacturer, SAMS sponsored its first formal cardiology mission to Jordan—where the UN Refugee Agency estimates 655,000 Syrian refugees are currently living—with Lababidi in charge.
Knowing that the patients he’d treat would likely be unable to afford any postprocedural medications, Lababidi said he carried “17,000 Plavix pills in my suitcase.” The five interventionalists and one surgeon traveled to Jordan on their own dime; SAMS provides logistics but only pays for cath-lab time and case coordination. Over 6 days, the team performed 100 catheterizations (with about half of patients needing stents) and performed 15 bypass surgeries.
One patient Lababidi remembers from that trip was a 27-year-old “who came basically on his death bed” needing both mitral and aortic valve replacement due to endocarditis caused by rheumatic fever. Within a month after his operation, he had completely recovered. Without the mission, the patient would have faced “certain death,” Lababidi said. “It gives you the sense that you’re making a huge difference in people, not only improving quality of life like we do here in the US every day, but literally saving their lives. There was a [young adult] who basically got a life back that he wouldn't have had. . . . These kinds of patients stick in your mind.”
Stefan Harb, MD (LKH Graz Süd-West, Graz, Austria), who went on SAMS’ fifth mission to Jordan last July with four other interventional cardiologists doing an average of 12 procedures a day, told TCTMD that the treatment of refugees is remarkably different than the work he does back home. They’ve “put their disease in the background,” he explained. “They try to care for their families, they try to find a way to support themselves and their families and to build a new life. There are so many basic things [they need to tend to], so . . . many had been suffering for years.”
I have to be very aware of the fact that hopefully I do not hurt more than I help. Stefan Harb
One difficulty of participating in a mission like this, Harb continued, is the need to lessen individual ambition in order to “do the most necessary work.” For example, “you're not doing the CTOs—you're trying to do the LAD stenosis, you're trying to avoid complications,” he explained. Avoiding complications is especially critical in a refugee medicine setting, since the ability to follow-up is limited.“I have to be very aware of the fact that hopefully I do not hurt more than I help,” Harb said. “You have to be a lot more considerate in your actions.”
Challenges on Top of Challenges
What drives Mohammed W. Akhter, MD (UMass Worcester, MA), to keep going on medical missions to help Syrian refugees, using “basically all” of his vacation time to do so, is an inherent desire to help. “This is a part of the world that’s been forgotten by everybody,” he told TCTMD. “It seems the conflict has no end . . . . There’s very little being done in terms of financial support for these people. It's just horrendous when you look at the images.”
Sacrificing his vacation days seems “inconsequential,” by comparison. “You’re talking with people who are displaced from their homes, that have now been living in refugee camps for years—people that have lost everything.”
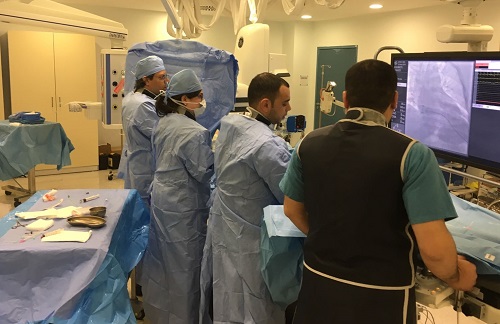 The work is not without challenges. The hours are long, physicians often have to travel to remote places to see patients, and jetlag also sets in. Additionally, Akhter said, “it's a resources-poor environment, so you're out of your comfort zone.” Certain wires or catheters that are common in most cath labs back home might not be readily available, the staff are less well trained, and the “promised” cath-lab time might abruptly disappear, he added.
The work is not without challenges. The hours are long, physicians often have to travel to remote places to see patients, and jetlag also sets in. Additionally, Akhter said, “it's a resources-poor environment, so you're out of your comfort zone.” Certain wires or catheters that are common in most cath labs back home might not be readily available, the staff are less well trained, and the “promised” cath-lab time might abruptly disappear, he added.
The patient population is also very different from what most of the volunteers treat at home. This is in part, Lababidi explained, because the prevalence of coronary artery disease is particularly high among refugees, due to psychological and physical stress as well as higher rates of smoking. “We are treating patients in their 30s, 40s, and 50s,” he said. “Very rarely do you see a patient in their mid or late 60s.”
Additionally, as refugees in the neighboring country of Jordan, their status means they often cannot receive the healthcare they need. Lababidi told the story of a patient who had gone to a Jordanian hospital complaining of chest pain for months, yet because he couldn’t afford the $8,000 advance payment, he was turned away. Lababidi treated this patient on his first mission and found a 99% block in his left circumflex and a 99% block in his right coronary artery. “He was crying and saying thank you very much,” Lababidi recalled, “if it wasn't for you I'd probably be dead and nobody would care, because I don’t have the money to pay.”
This is a part of the world that’s been forgotten by everybody. . . . It seems the conflict has no end. Mohammed W. Akhter
Language also plays a role. Harb doesn’t speak Arabic like most of the patients he treated in Jordan, so he used a translator. “This is quite an obstacle,” he said. “It takes more time just to find out if it's necessary to do the intervention.”
More than the translation, patients who have been suffering for years “present rather differently because they have become accustomed to their situation,” Harb further explained, adding that sometimes the help that’s needed most would come from a psychologist, not a cardiologist.
For physicians doing this work, the biggest personal test may not come until the mission is over, Akhter said. The “emotional and psychological burden” often can’t be processed until the volunteer clinicians arrive back home, he said. “Unfortunately, that’s the time when you’re back at work . . . so it’s sort of like worst-case scenario.”
It does take “a certain kind of person” to handle the specific stresses of a mission like this, he observed. Physicians “become hardwired to work with lack of sleep and all of that stuff, but I think the emotional reserve is probably not something that everyone has,” Akhter said. “I’ve always noticed that the mission itself goes by very quickly, but the aftereffects last a while when you're back.”
Harb said people at SAMS have encouraged him to talk about what he has experienced. “You don’t have to be the hero,” he said. “There is always fear involved and there is insecurity,” but having help from colleagues who feel similarly enables him to embrace his feelings as “natural.”
An Expensive Endeavor
There’s also the issue of funding. SAMS relies on donated stents and devices for all its missions, and Lababidi estimates that this amounts to “at least $200 to $300 thousand” per trip. To date, SAMS has worked with two corporate sponsors, but the organization is open to collaborating with others. The devices that have been donated are the “top of the line that are sometimes not even available” in the mission country, according to Lababidi.
While physician volunteers donate all their operating time, the organization pays local area hospitals for the use of their cath labs as well as for translators and transportation for the volunteers.
As a nongovernmental organization, SAMS collects contributions from supporters worldwide to continue its work. Only recently did the nonprofit secure device donations that enable volunteers on cardiology missions to conduct electrophysiology work, Lababidi reported. SAMS sent two electrophysiologists on its first mission to Egypt in November, and they were able to implant 10 devices for patients in need. Lababidi said they plan to expand their electrophysiology endeavors in Jordan this year.
But the costs associated with a PCI continue long after the procedure. “All of the medications that we give after stenting are very, very expensive, and if you were to buy them locally, the cost is prohibitive,” Akhter said, explaining that he, like Lababidi, has bought pills himself and transported them to Jordan.
“Maybe we can have a central repository of catheters, guidewires, [and] balloons” organized for the sole purpose of medical missions around the globe, Akhter suggested. “It can be done in a way that takes industry bias out of it, and then physicians and medical organizations can apply for these things. . . . I think you would see a lot more organized missions not just to Syria and Jordan, but to other places in Africa and South America and India. And I’m sure that there are people who are interested in doing this, they just don't have the resources to do it.”
Why Do It?
When Harb was first contemplating a mission to Jordan, it prompted a lot of soul-searching. “I would say: ‘Why are you doing this? Why are you going to this place? Is there some problem with you? Do you want to be a hero? Will it be useful? Will it be for nothing?” he told TCTMD, adding that his wife often chimed in with her own inquiries. In the end, she ended up accompanying him on the trip to help out with documentation.
Ultimately the ability to do more than “just give money” was gratifying for Harb. “If you find out that your actions are actually transformed into well-being, you directly have this feedback, and it’s very rewarding,” he said.
Lababidi, too, said he feels a “sense of responsibility” to continue this work: “I’m blessed to [have left] Syria when the turmoil was not even that bad to come to this country, and blessed to really have a great opportunity to pursue my career and my personal life. We see it as an opportunity to give back to the people of Syria and other people who are in great need.”
The humanitarian drive to “give back” is why many people go to medical school in the first place, he continued. With organizations like SAMS, “you have the opportunity to do just that. It’s a very pure relationship of providing patients in dire need with the treatment they need and nothing else,” Lababidi said, adding that mission work is “addictive.”
 Participating in these missions is also “a great learning experience,” according to Harb. “I was confronted with colleagues coming from the United States, from the UK, from Pakistan, from India, from all kinds of religious backgrounds and also from Syria itself . . . . So I got lots of chances to get some more insight” into the wider world.
Participating in these missions is also “a great learning experience,” according to Harb. “I was confronted with colleagues coming from the United States, from the UK, from Pakistan, from India, from all kinds of religious backgrounds and also from Syria itself . . . . So I got lots of chances to get some more insight” into the wider world.
Akhter agreed. The mission team “is like a band of brothers and sisters,” he said. “These are obviously people that are very similar to who you are, and that camaraderie [is] what you bring back with you.”
For Akhter, the experience he has received as a provider practicing refugee medicine is one of the things that keeps him going back. Calling medicine in the US today “more transactional,” in that a patient or insurance company pays for a service that physicians provide, he said he doesn’t always feel connected to the tradition of healing that has long drawn doctors to their field.
“When you go on a medical mission, it harkens back to the more historical sense of the profession, which is that you’re a healer, that you’re there to alleviate people's suffering,” Akhter explained. “It’s more altruistic and it’s less transactional, and because of that, the emotional satisfaction is way more than what you experience here” in the United States.
While he doesn’t dismiss the gratitude shown by his patients in Worcester after a successful procedure, the thanks he receives from patients on medical missions is of a different order, Akhter said. “Sometimes the fact that they can share their stories and sort of unload on us and tell us what they've been through [means] you’re sort of a witness to their suffering. They want to document it, and they want to tell people.”
Harb echoed those sentiments, saying, “I’m happy in Austria,” but said knowing what he can offer in a war-torn part of the globe is much more emotionally intense. He stressed that it’s not a question of taking one side or the other in the Syrian conflict, rather he said he feels strongly that “you have to do something. You have to organize something if you actually believe in helping everybody without political thinking and without thinking of who is an enemy and who is not.”
Akhter said he recognizes that he will never be able to fully comprehend what the refugees he’s treated have gone through, and what they continue to experience daily. “You do feel like this whole situation takes away people's dignity. There's no way I can give it back to them,” he remarked. The work he hopes to continue doing with SAMS is “sort of a drop in the bucket, but if we didn't even do that, it would be entirely hopeless.”

Photo Credits: Stefan Harb and Mohammed W. Akhter
Yael L. Maxwell is Senior Medical Journalist for TCTMD and Section Editor of TCTMD's Fellows Forum. She served as the inaugural…
Read Full Bio

Comments