Could Robotic PCI Play a Protective Role in Pandemics?
Some say COVID-19 might pave the way for more robotic procedures, but proof they cut disease transmission is lacking.
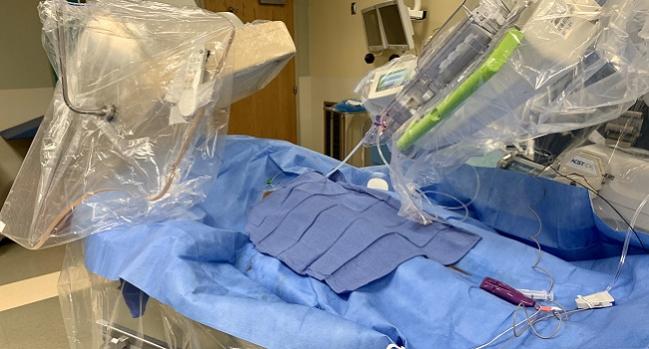
Robotic systems for coronary interventions have been touted as a way to improve workplace safety for interventionalists, reducing radiation exposure and easing orthopedic injuries related to wearing heavy lead. But what if removing interventionalists and others from the bedside could have the added benefit of reducing exposure to infectious diseases during a crisis like the ongoing COVID-19 pandemic?
Jon George, MD, director of the cardiac cath lab at Einstein Medical Center (Philadelphia, PA), hinted at that question on Twitter after his team performed their first robotic intervention on a patient presumed to be COVID-19-positive, noting that the robotic system allows personnel to maintain a 6-foot distance after access and enables them to take other safety precautions.
Speaking with TCTMD, he said there potentially is a role for robotic interventions in the context of an infectious disease outbreak, although he acknowledged that this would not completely protect the cath lab team from exposure to a pathogen.
“It allows you to minimize the amount or duration of exposure. It doesn’t completely eliminate exposure,” George said, pointing out that the operator still has to gain access to the artery and either the operator or a technician has to exchange equipment on the robotic arm. The interventional cardiologist could either serve both of these functions or have a technician on hand to cut down on the need to move back and forth between the cockpit with the robotic controls and the table.
“You could potentially operate and do the entire procedure with one person, or a maximum of two people, as opposed to having three or four people close to bedside,” George said.
Good in Theory, but Maybe Not Practical
George said the potential role of robotic interventions as a way to reduce risk of disease transmission during an outbreak has not really been discussed formally before, noting that his post on Twitter sparked “quite a bit of conversation” involving both the interventional community and Corindus (acquired last year by Siemens Healthineers)—the company that makes the CorPath GRX system. CorPath GRX remains the only robotic system approved in the United States and Europe for coronary and peripheral interventions.
You could potentially operate and do the entire procedure with one person, or a maximum of two people, as opposed to having three or four people close to bedside. Jon George
“A lot of the advantages of robotics has revolved around minimizing radiation exposure and then improving the precision and accuracy of delivering devices,” George said. “It had nothing to do with protection from a pandemic, so this is a new area.”
William Lombardi, MD (Heart Institute at UW Medical Center—Montlake, Seattle, WA), said his team has continued to perform robotic-assisted PCIs during the COVID-19 pandemic, and said there is certainly potential to reduce exposure by minimizing the number of people and shortening the time spent in the cath lab. He added, however, that they have not changed anything about how they’re use robotics in response to the crisis.
“I think as this continues to progress and the duration increases, we’ll probably start to look at some ways that we potentially can utilize this for those reasons, but we haven’t really thought about it yet,” Lombardi said. Ramping up use while the pandemic is ongoing would be difficult for most centers, he pointed out, because of the challenges associated with the need to provide training and education during a public health crisis.
At his center, Lombardi said, they’ve done 400 to 500 robotic cases in the last year-and-a-half, but “for a place that’s done 50, that’s going to be a bigger challenge, because you’re still really on your learning curve with how to use the technology and be comfortable with it.”
Ryan Madder, MD (Spectrum Health, Grand Rapids, MI), pointed out to TCTMD that the idea of using robotics to reduce infectious risks during a pandemic has never been studied, though there are possible benefits. “If the interventionalist did not have to scrub in to seat the guide catheter or get access, it could prevent the need for the interventionalist to use any personal protective equipment [PPE]. If they were outside the room, they wouldn’t have to burn through a mask and gown,” he said. Availability of PPE, or lack thereof, has been a continuing problem during the COVID-19 pandemic.
According to Lloyd Klein, MD (University of California, San Francisco), there are a couple of issues that need to be considered when thinking about a role for robotics during an outbreak.
During the current pandemic, there’ve been reports of patients presenting later with MI, which means more are coming in with mechanical complications associated with the infarct. Those types of cases are not generally the ones operators would be thinking about for robotic-assisted PCI, Klein said, adding, too, that there are certain morphologic and anatomic features, like bifurcation lesions, that an operator would want to know are absent before going ahead with a robotic procedure.
In addition, a major source of concern about exposure to SARS-CoV-2 in the cath lab revolves around patients going into cardiac arrest on the table, Klein said. Robotic assistance would not preclude the need to go in and resuscitate the patient.
Nonetheless, using a robotic strategy to lessen exposure risk “does make some sense,” Klein said. “It’s a good idea in theory, but in practice it may not be practical under these circumstances.”
Help From Afar
When it comes considering robotics to reduce risk to cath lab staff during an infectious disease outbreak, George said, the “golden egg we’re chasing” is fully remote PCI, or telestenting—having the operator control the robotic arm from the next room or even miles away at another center.
Feasibility studies have been done. Led by Madder, the REMOTE-PCI study, which included 20 patients, demonstrated technical and procedural success rates of 86.4% and 95.0%, respectively, when procedures were performed by an operator in a room down the hall. Later, Madder demonstrated the feasibility of telestenting in pigs from a distance of about 103 miles. And more recently, Tejas Patel, MBBS (Apex Heart Institute, Ahmedabad, India), successfully performed robotic-assisted PCI in five patients while sitting about 20 miles away.
“At least in the future if this were to be studied further and developed further, potentially if hospital systems lost interventionalists or had interventionalists put on the sidelines by active infections, you could disseminate interventional expertise from other areas around the world to those hospitals using remote robotics,” Madder said. “But we’re not ready for that yet. It’s only in concept form at this point and has not been attempted.”
You wish that technology had been developed further by the time this has occurred, because you could have really changed the exposure risk of a lot of staff [and] could prevent them from even coming to the hospital. William Lombardi
The next phase of research, he said, is testing the ability to perform remote PCI over very long distances. Last year, Madder, at the controls in Waltham, MA, performed 36 simulated PCI procedures in New York City and San Francisco, CA, over 5G wireless, dedicated fiber, and commercial public internet networks.
“What we demonstrated was not only is it possible for an operator to manipulate a robotic arm in a transcontinental fashion, but the round trip latency even over public internet was less than 200 milliseconds, which is completely acceptable as far as I’m concerned,” Madder said, noting that that level of latency was imperceptible to him.
In addition to the need for a focused clinical trial to demonstrate the safety and effectiveness of performing robotic PCI from miles away, George and Lombardi pointed to medicolegal challenges that would have to be overcome, at least in the United States, before it would be allowed.
“The whole remote PCI concept becomes incredibly favorable in a situation like this,” Lombardi said. “You wish that technology had been developed further by the time this has occurred, because you could have really changed the exposure risk of a lot of staff [and] could prevent them from even coming to the hospital.”
Preparing for the Future
Incorporating robotic-assisted procedures into a pandemic response is “an interesting idea,” Madder said, “but I think we still need to study it to make sure that it is safe to do and accomplishes the intended objective, which would be to decrease infection risk or disseminate interventional expertise to areas where their own interventional expertise may have been compromised by infection.”
Infectious risk in the cath lab depends on the type of pathogen and whether the room has negative- or positive-pressure ventilation, Klein pointed out, adding, though, that “ordinarily I would think that if you’re dressed appropriately for a straightforward procedure, the risk would be small.” If something went wrong, however, the risk would potentially rise. “I think that’s why the idea of robotic is appealing,” Klein said, “I just don’t know if it’s practically applicable.”
Looking ahead, the COVID-19 pandemic is going to lead to a lot of thinking across medicine about how things have been done and how they should change, Klein said, citing as an example changes in thinking about when patients should be ventilated as SARS-CoV-2 has spread around the world.
“I have no doubt that there are things in the cath lab that we do routinely that we’re going to have to rethink,” Klein said. “I sure hope that it makes us rethink infection and communicable diseases in the lab. I think that has been loose for a very, very long time, and I think that exposure to aerosols, especially in arrest situations, even if there’s not COVID, is something that we ought to be taking more seriously.”
He suggested that situations like the COVID-19 pandemic might get hospitals thinking more about purchasing robotic systems, which have made only a small dent in the marketplace thus far. “Up until now, people thought of robotics as a luxury, and it may be that it isn’t a luxury anymore. If we start thinking that we’re going to have more and more of these kinds of things, then it’s something that a hospital with a large volume has to start thinking about and being prepared for.”
Lombardi picked up a similar thread. “In every really bad thing, there’s an opportunity for change to allow for improvement, and there’s been a lot of discussions the last couple of years about robots. There’s been a lot of resistance, and there’s been some excitement. Most of that was around occupational health issues in regard to orthopedic injuries from wearing lead and cancer risks related to radiation.
“And maybe this is just another piece of the puzzle,” he continued, “where we look at this as an opportunity to further protect ourselves and allow for us to rapidly change how we practice healthcare to be more protective and more proactive and look at it as an opportunity to improve not just for the pandemic but also long term for our profession.”
Todd Neale is the Associate News Editor for TCTMD and a Senior Medical Journalist. He got his start in journalism at …
Read Full BioDisclosures
- George reports being consultant for Corindus and Siemens.
- Madder reports receiving research support from and serving on the advisory board for Corindus.
- Lombardi reports having had equity in Corindus until October 2019, when the company was acquired by Siemens Healthineers.
- Klein reports no relevant conflicts of interest.


Comments