CTO PCI Post-CABG Associated With Worse Outcomes
The confirmatory data can help patients and operators weigh the risks and benefits of doing the procedure, experts say.
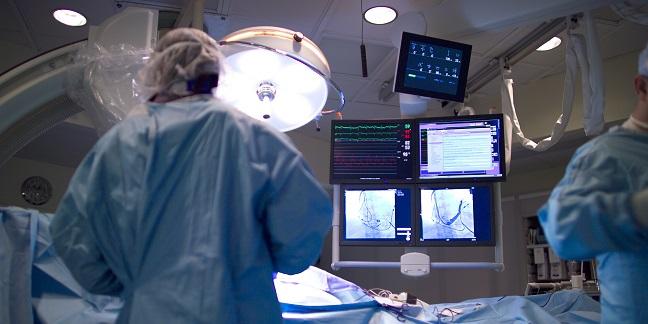
Patients undergoing PCI for chronic total occlusion (CTO) lesions have poorer outcomes and more complex procedures if they have previously undergone CABG surgery than if they have not, according to results of a new meta-analysis.
“For beginning operators, doing previous-bypass patients might not be the best way to learn CTO intervention,” senior author Emmanouil Brilakis, MD, PhD (Minneapolis Heart Institute, MN), told TCTMD, adding that these patients are likely going to be better treated by operators and at centers with more experience. “Secondly, even for more experienced operators, when tackling previous bypass . . . maybe allocate more time to the cath lab or anticipate more complexity.”
For the study, published online as a research letter yesterday ahead of print in JACC: Cardiovascular Interventions, Michael Megaly, MD (Minneapolis Heart Institute), along with Brilakis and colleagues included 8,131 patients (8,544 lesions) from four observational CTO PCI studies, including the PROGRESS CTO registry, that enrolled between 1999 and 2018.
A total of 2,163 patients had prior CABG, and they were more likely to be older, have more comorbidities, and have more complex lesions. Patients with prior CABG were also more likely to undergo retrograde CTO crossing attempts (34.7% vs 21.9%; P < 0.001).
Technical success was lower for patients with prior CABG (80.7% vs 86.5%), who also had longer fluoroscopy times (mean difference 16.9 min), and higher contrast use (mean difference 16.4 mL; P < 0.001 for all). This cohort also had a higher incidence of in-hospital mortality, coronary perforation, and MI but a lower incidence of cardiac tamponade compared with patients without prior CABG.
In-Hospital Outcomes
|
|
Prior CABG |
No CABG |
OR |
95% CI |
|
Mortality |
0.8% |
0.3% |
2.77 |
1.43-5.39 |
|
Coronary Perforation |
7.3% |
4.90% |
2.07 |
1.49-2.86 |
|
MI |
1.4% |
0.5% |
2.46 |
1.46-4.15 |
|
Cardiac Tamponade |
0.1% |
0.8% |
0.19 |
0.04-0.87 |
Both groups reported similar incidences of acute cerebrovascular events and vascular complications.
Helpful for Risk Stratification
Brilakis said that US operators need to be especially mindful of these findings given that “in the US, we have many more previous bypass patients coming to the cath lab compared with other countries. So it's just a matter of being aware of this and that this may be more difficult and require more time and have slightly lower success than if the patient did not have bypass.”
Commenting on the study for TCTMD, Creighton Don, MD (University of Washington, Seattle), said the findings were “pretty much expected” given prior individual reports. Still, meta-analyses like this one, he added, are helpful in “reviewing the data that's out there and confirming our suspicions.”
The study has implications for risk stratification, he explained. “If you have a patient who has minimal symptoms and it's a post-CABG patient with a very complex circumflex CTO, you may be more inclined to medically manage that patient than if it's someone who has a very straightforward CTO with the same symptoms,” Don said. “Or if you have someone who has no prior CABG with minor symptoms, you might be more inclined to do the procedure because you're weighing the risks and benefits.”
But it’s not only about decisions on the front end, he added. “One of the take-home points is that . . . when you're treating these patients to be very conscientious of these kind of complications [like perforation] that can happen and be ready to deal with them.”
Don agreed with Brilakis that patients with prior CABG undergoing CTO PCI are better off treated by experienced operators and at centers with appropriate backup. “Maybe some sites are better prepared to do these than others, and I think patients just need to be aware of that,” he said. “If your site has only done one CTO PCI on a post-CABG patient in the past 2 years, they should be aware that this is a high-risk procedure and potentially should be at site that is better prepared to manage it or has more familiarity with it.”
Despite what the aggregate data show, however, not every post-CABG or retrograde case is high risk, he stressed. “There are some patients [in whom] it’s quite easy.” Because of this, Don said he would like to see future studies demonstrate how to risk stratify patients better by anatomy. “I think the J-CTO score is somewhat inadequate in this situation, because . . . it doesn’t tell you anything about the distal bed or how good the retrograde option is or is not,” he explained.
One suggestion Brilakis had to better plan procedures for post-CABG patients is to perform coronary CT angiography. “[It] can really help clarify ambiguity, can help extend the distal vessel, and also help understand calcification in the good reentry zones,” he said. “Especially for bypass patients, who have a lot of calcium and a lot of complexities with sometimes occluded bypasses and ambiguous anatomy, doing coronary CT angiography can really be very useful.”
The overall message of the study, according the Brilakis: “We're making progress, but we're not there yet and more research and more education is needed for this group.”
Yael L. Maxwell is Senior Medical Journalist for TCTMD and Section Editor of TCTMD's Fellows Forum. She served as the inaugural…
Read Full BioSources
Megaly M, Abraham B, Pershad A, et al. Outcomes of chronic total occlusion percutaneous coronary intervention in patients with prior bypass surgery. J Am Coll Cardiol Intv. 2020;Epub ahead of print.
Disclosures
- Megaly and Don report no relevant conflicts of interest.
- Brilakis reports receiving consulting/speaker honoraria from Abbott Vascular, American Heart Association, Biotronik, Boston Scientific, Cardiovascular Innovations Foundation, CSI, Elsevier, GE Healthcare, InfraRedx, Medtronic, Siemens, and Teleflex; receiving research support from Regeneron and Siemens; and holding shares in MHI Ventures.


Comments