Experience Matters: Patients of High-Volume Operators Have Lower Mortality Rates After Left Main PCI
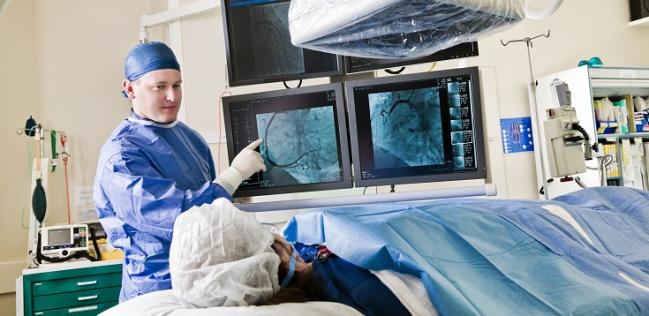
Interventional cardiologists with more experience in performing left main PCI achieve significantly better short-term and long-term outcomes when compared with operators who have less experience, a new study shows.
In an analysis of 1,948 patients who underwent unprotected left main PCI at a single center in China, those treated by an experienced operator—defined as a physician who performed at least 15 left main PCIs annually for 3 consecutive years—had significantly lower rates of cardiac death at 30 days and 3 years, report investigators.
“The volume or experience variable is extremely important, particularly in complex interventions, if you want to ensure the full benefit of the procedure,” senior investigator Philippe Généreux, MD (Hôpital du Sacré-Coeur de Montréal, Canada), told TCTMD. “For the first time, with left main PCI, we identify that the variables—operator experience and operator volume—are some of the strongest determinants of cardiac mortality after the intervention. There is almost a four-fold difference in mortality at 30 days, meaning that if the intervention is done by a high-volume operator, we can really ensure the benefit of the less invasive PCI procedure compared with surgery.”
The study, published online October 17, 2016, ahead of print in JACC: Cardiovascular Interventions, included left main procedures performed by 25 operators at Fu Wai Hospital (Beijing, China). Of these operators, seven were considered experienced in left main PCI, with experienced operators, on average, performing 25 left main procedures each year. In contrast, the inexperienced operators performed a mean of four left main PCIs each year. Between 2004 and 2011, 1,422 patients were treated by an experienced operator and 526 patients by an inexperienced interventionalist.
Cardiac mortality at 30 days was 0.5% for patients treated by an experienced operator and 2.1% for patients treated by an inexperienced interventionalist (P = 0.002). There was a trend toward a lower rate of definite/probable stent thrombosis among patients treated by experienced operators, but the difference was not statistically significant (0.4% vs 1.1%; P = 0.10). In the adjusted model, which accounted for the increased complexity of coronary disease and lesion type in the high-volume arm, this translated into a 66% lower risk of definite/probable stent thrombosis bordering on significance (P = 0.06).
At 1 and 3 years, there remained a significantly lower risk of cardiac death among patients treated by experienced operators. At 3 years, 2.5% of patients treated by experienced physicians died of cardiac causes compared with 4.6% of patients treated by inexperienced operators (P = 0.02). The same trend was observed when operators were stratified into tertiles based on their experience.
Davide Capodanno, MD (University of Catania, Italy), who was not involved in the study, said lesions in the left main artery are a “totally different animal” and require an excellent implantation technique to achieve optimal results. Unlike other arteries, there is no leeway for achieving only a “fair” procedural result. These latest findings showing improved outcomes with high-volume operators “demonstrate numerically what we have always suspected, and that is that experience plays a role,” he told TCTMD.
Even within the SYNTAX trial—a study comparing CABG versus PCI in patients with multivessel or left main coronary disease—there were centers who obtained excellent surgical results and poorer PCI results, he said. “It’s quite expected to have bad clinical outcomes when the procedure is not done very well in such a delicate point of the coronary arteries,” said Capodanno, referring to the left main.
Overall, the findings suggest a need for increased experience amongst operators tackling lesions in the left main coronary artery. This means an enhanced focus on teaching the procedure to less experienced physicians, as well as a responsibility for physicians to learn the right steps when doing left main interventions. “I think it’s also a call for standardization [of the procedure], and we will learn a lot from the upcoming EXCEL and NOBLE because many mandatory steps are included in the protocols of these studies,” said Capodanno.
EXCEL and NOBLE—two studies of PCI in left main coronary artery disease—will be presented at TCT 2016 in Washington, DC. In the United States at present, left main PCI is a class IIa or IIb recommendation—it is or may be reasonable—for low-to-intermediate risk patients.
Outcomes Linked With Volume in Other Procedures
To TCTMD, Généreux said that in other procedures, such as radial access PCI, chronic total occlusion (CTO) PCI, and TAVR, there is a strong relationship between operator experience and clinical outcomes, with outcomes improving as operators progress along the learning curve. In the RIVAL trial, for example, investigators showed that overall hospital volume and radial PCI volume were independently associated with a reduction in the risk of death, MI, stroke, and non-CABG major bleeding.
Their findings, he said, are not meant to push operators away from performing unprotected left main PCI, but they suggest highly experienced operators “should be in the room during complex cases to ensure appropriate results.” Généreux added that he would be in favor of clinical guidelines or recommendations for minimum volume requirements for operators performing left main PCI, or at the very least, the presence of an experienced operator in the cath lab while the procedure is performed.
“If you’re doing 35 PCIs a year, maybe you’re not the best person from a patient’s point of view to be doing these complex cases,” he said. “Of course, if you’ve been at this for 20 years and have had good results, that could be OK. But to be honest with the patient, and to be honest for the field, we should have public outcomes published and available as well as volumes published and available, which would help improve patient outcomes. If you’re not doing the numbers, and you want to learn to do these procedures, you can be paired with a high-volume operator.”
Revising Risk Algorithms?
In the study, researchers including lead investigator Bo Xu, MD (Fu Wai Hospital, Beijing, China), showed that being treated by a high-volume operator was associated with a 51% lower risk of cardiac death after adjusting for known cardiovascular risk factors. Importantly, adding operator experience to the SYNTAX and SYNTAX II scores improved the risk stratification model, increasing the discrimination capability of both scores. Based on those findings, Généreux and colleagues believe experience and volume should be incorporated into traditional risk-stratification algorithms when debating revascularization approaches.
“Operator volume and experience is not represented in any risk score, including the SYNTAX score,” said Généreux. “It’s always the missing variable, the elephant in the room. . . . The dogma of the SYNTAX score or any score, not taking into account the experience of the operator, or the experience of the center, could be extremely detrimental to patients. It’s the variable that likely impacts outcome the most after PCI.”
James Blankenship, MD (Geisinger Medical Center, Danville, PA), immediate past-president of the Society for Cardiovascular Angiography and Interventions (SCAI), noted that left main interventions are a relatively high-risk procedure, but that there is differential risk depending on individual patient characteristics. Distal left main lesions at the bifurcation of the left anterior descending and circumflex artery tend to be trickiest, he commented. “That being said, something going wrong anywhere [in the left main] can lead to death.”
Blankenship said there hasn’t been discussion at SCAI about volume requirements for physicians treating left main disease, but similar to CTO interventions, another technically challenging procedure, the consensus is that experience is important. The procedure should be learned carefully with proctoring and performed in centers where low-volume operators can receive backup if needed. If physicians are going to “dabble” in complex procedures, they’re going to get worse results, he said.
In an editorial, Ralph Brindis, MD (University of California, San Francisco) and Gregory Dehmer, MD (Texas A&M University School of Medicine, Temple, TX), note that US operators perform, on average, 59 PCIs each year according to data from the National Cardiovascular Data Registry (NCDR) CathPCI Registry. Data from the registry also suggest that US interventionalists perform just two unprotected left main PCIs each year, they add.
The editorialists suggest that “how many have you done” is a valid question when physicians are tasked with treating lesions in the left main coronary artery. If the lead of the Chinese researchers is followed, a “center of excellence” should include high-volume operators experienced in treating left main disease. To TCTMD, Généreux suggested the magnitude of difference in clinical outcomes between low- and high-volume operators is likely even larger in the US given that even the low-volume operators in the Chinese study were experienced by US standards.
Note: Généreux is a faculty member of the Cardiovascular Research Foundation, the publisher of TCTMD.
Michael O’Riordan is the Managing Editor for TCTMD. He completed his undergraduate degrees at Queen’s University in Kingston, ON, and…
Read Full BioSources
Xu B, Redfors B, Yang Y, et al. Impact of operator experience and volume on outcomes after left main coronary artery percutaneous coronary intervention. J Am Coll Cardiol Intv. 2016;9:2086-93.
Brindis RG, Dehmer GJ. The volume-outcome relationship revisited: does it matter for high-risk PCI? J Am Coll Cardiol Intv. 2016;9:2094-2096.
Disclosures
- Xu, Généreux, and colleagues report no conflicts of interest.
- Brindis and Dehmer report no conflicts of interest.


Comments