Heterozygous FH Diagnosed Late, Remains Undertreated
Physicians are missing a large opportunity to aggressively treat FH patients and prevent the onset of ASCVD, says expert.
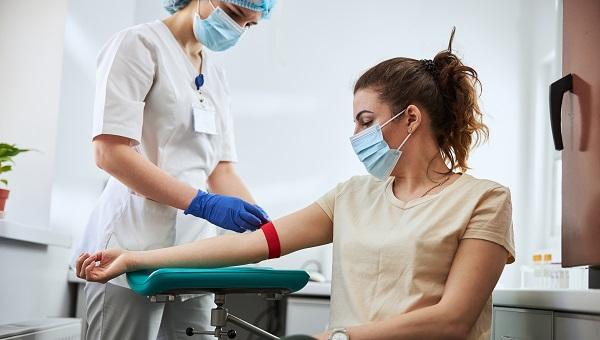
Patients with familial hypercholesterolemia (FH) often are diagnosed late in life and remain undertreated with lipid-lowering medications despite their increased risk for cardiovascular disease, according to new findings from a large observational study.
In this registry from the European Atherosclerosis Society (EAS) Familial Hypercholesterolemia Studies Collaboration (FHSC), which included more than 42,000 patients with FH, the mean age at the time of diagnosis was 44.4 years and coronary artery disease was already established in more than one in six patients.
Kausik Ray, MBChB, MD (Imperial College London, England), president of the EAS and lead investigator of the FHSC global registry, said a diagnosis in the mid-40s is a missed opportunity. “When you think about prevention, the earlier you start the better the prognosis is going to be, because you have a lot more time to slow down/arrest disease rather than trying to do it later on,” Ray told TCTMD. “That has important implications for screening, such as starting much, much earlier. It’s one of the things that we’d like to see happen, which is universal screening for cholesterol, certainly before the age of 20.”
The new study was published September 7, 2021, in the Lancet.
Patients Mostly Just on a Statin
The FHSC is an international collaboration of physicians treating patients in specialized clinics that are included in national, regional, or local FH registries. The FHSC data set consists of 61,612 patients from 56 countries, of whom 42,167 were aged 18 years or older with probable or definite diagnosis of heterozygous FH. At the time of entry into the registry, the mean age of participants was 46.2 years and 53.6% were women.
Overall, 40.2% of patients were diagnosed with FH before age 40 and just 2.1% before 18 years. At the time of diagnosis, 19.2% of patients had hypertension, 5.0% had diabetes, 23.5% were smokers, 17.4% had CAD, and 11.3% had premature CAD. Women, on average, were older than men at the time of diagnosis (median 46 vs 43 years; P < 0.001) and had significantly higher levels of total and LDL cholesterol.
Nearly 60% of all patients were treated with lipid-lowering medication, and the median LDL-cholesterol level for those on treatment was 4.23 mmol/L (163.57 mg/dL). For those not taking treatment, the median level was 5.43 (210.0 mg/dL). The prevalence of CAD increased progressively with increasing LDL cholesterol. For example, among those with levels ≤ 4.9 mmol/L (190.0 mg/dL), 6.4% had a diagnosis of CAD. In contrast, among those with LDL levels ≥ 8.5 mmol/L (328.7 mg/dL), the prevalence of CAD was 26.9%.
Of those taking lipid-lowering medications, 81.1% were taking statins, with or without another agent. Men were more likely than women to be treated with a high-intensity statin (16.6% vs 13.1%; P < 0.001), such as atorvastatin 80 mg or rosuvastatin 40 mg. Just 21.2% of all patients were taking combination therapy with two or more agents that included a statin, ezetimibe, or a PCSK9 inhibitor. Again, men were more likely than women to be treated with combination therapy (22.7% vs 19.9%; P < 0.001).
“If you look at global guidelines, what we found was that for the levels of cholesterol most people recommend—ie, less than 70 mg/dL or 1.8 mmol/L—only about 3% of the population got to that level,” said Ray.
Women fared worse than men, with only 2.0% of women getting to a target of < 70 mg/dL on combination therapy compared with 3.4% of men (P < 0.001). Given that so few were at goal and the prevalence of CAD increased with higher LDL-cholesterol levels, there is an urgent need to use multiple lipid-lowering agents to bring cholesterol down to acceptable levels, said Ray.
“It really means a move away from monotherapy towards using combination therapy,” he said. With these very high LDL levels, and patients’ relatively advanced age at the time of the intervention, “we’re really only putting a sticking plaster” with monotherapy, said Ray. Instead, patients will require two, three, or possibly four medications to lower LDL-cholesterol levels down to less than 70 mg/dL, or even lower depending on the patient’s 10-year risk of atherosclerotic cardiovascular disease (ASCVD). “The later you make the diagnosis, the greater the likelihood you’ll need three or four drugs, because you’ve missed all of these years and missed more disease,” he said.
As for PCSK9 inhibitors, Ray said there are still limitations to access. Slowly, uptake of the drugs is improving, he said, but overall use remains relatively low. For example, in the observational DA VINCI study, use of PCSK9 inhibitors in 2017-2018 was just 1%. In SANTORINI, an observational study of high- and very-high-risk patients recently presented at the European Society of Cardiology Congress, use of the monoclonal antibodies in 2020-2021 had increased to 4.1%.
“There are still barriers, but it is easier,” said Ray. With heterozygous FH, where patients have one abnormal gene, typically a pathogenic variant of LDLR, the PCSK9 inhibitors, or even inclisiran, which is now available in Europe, are ideal add-ons that can result in an 80% reduction in LDL-cholesterol levels, he said.
Current Prescribing Inadequate
In an editorial accompanying the study, Marina Cuchel, MD, PhD (University of Pennsylvania Perelman School of Medicine, Philadelphia), and Mary McGowan, MD (Dartmouth-Hitchcock Medical Center, Lebanon, NH), make similar statements: FH is diagnosed too late and current lipid-lowering prescribing is inadequate. While PCSK9 inhibitors can reduce LDL cholesterol, there is limited access to the drugs in low- and middle-income countries, a health disparity that they say must be addressed.
“Nevertheless, statins and ezetimibe are now inexpensive and readily accessible, and both should be used to their maximum extent,” write Cuchel and McGowan.
Proud to be one of 14 Egyptian investigators who contributed data to this important #FHRC project just published in @TheLancet
— Ahmed Bendary, MD (@drabendary) September 8, 2021
Read the article on: https://t.co/BY8sJtHjfW#familial_hypercholesterolemia pic.twitter.com/f8pmAubrsP
Like Ray, the editorialists also target the current discrepancies with respect to diagnosing and treating women with FH. The reason might be the perception that women have a lower risk of ASCVD compared with men. In the FHSC registry, women did in fact have lower rates of CAD and premature CAD compared with men. However, Cuchel and McGowan point out that FH women 50 years and older had higher untreated LDL-cholesterol levels than men of the same age and a similar risk of ASCVD.
Ray hopes these new FHSC data will help inform future policy decisions and be part of the push for universal cholesterol screening to find patients earlier. Universal screening for FH would first involve measuring cholesterol levels. “If the lipid panel is abnormal, that’s when next steps develop,” he said. “We’re not advocating genetic screening—that would be potentially very expensive—but it should start with screening cholesterol and then narrowing down towards genetics as required.”
Michael O’Riordan is the Managing Editor for TCTMD. He completed his undergraduate degrees at Queen’s University in Kingston, ON, and…
Read Full BioSources
Vallejo-Vaz, AJ, Stevens CAT, Lyons ARM, et al. Global perspective of familial hypercholesterolemia: a cross-sectional study from the EAS Familial Hypercholesterolemia Studies Collaboration (FHSC). Lancet. 2021;Epub ahead of print.
Cuchel M, McGowan MP. Familial hypercholesterolemia: too many lost opportunities. Lancet. 2021;Epub ahead of print.
Disclosures
- Cuchel reports grants from Akcea Therapeutics, Regeneron Pharmaceuticals, and REGENEXBIO, and personal fees from Amryt Pharma.
- McGowan reports honoraria from Kaneka and participation in advisory boards for Novartis and Regeneron; and serving as the Chief Medical Officer of the FH Foundation.
- KKR reports grants and personal fees from Amgen, Sanofi–Regeneron, Pfizer, Merck Sharp & Dohme, and Daiichi Sankyo; and personal fees from AstraZeneca, The Medicines Company, Kowa, Novartis, Lilly, Algorithm, Boehringer Ingelheim, AbbVie, Silence Therapeutics, Bayer, Esperion, Abbott, New Amsterdam, and Resverlogix.




Comments