High-Sensitivity Troponin Assays May Stratify Risk in Chronic CAD
An exploratory analysis suggests an elevated troponin level may identify patients who would benefit from revascularization.
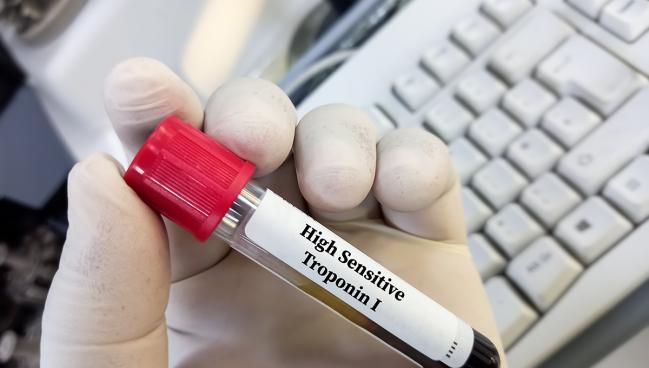
High-sensitivity cardiac troponin testing can identify patients with stable coronary artery disease who have a greater risk for MI or cardiovascular death, a study conducted in Scotland indicates.
That raises the possibility that implementing routine testing in an outpatient setting could help guide the management of patients with chronic coronary disease by finding those who require further testing or treatment, researchers say.
Indeed, an exploratory analysis suggested that in patients with troponin levels above 10 ng/L—but not in those with lower levels—coronary revascularization was associated with a lower risk of MI or CV death (5.2 vs 7.7 events per 100 patient-years).
The study, published online ahead of the August 8, 2023, issue of the Journal of the American College of Cardiology, “confirms the idea that troponin can be used to risk stratify these patients, it gives people a potential threshold to use, and also I think it steers towards future trials looking at selective coronary revascularization based on risk factors other than ischemia and using troponin as an objective measure of risk,” lead author Ryan Wereski, MD (British Heart Foundation Centre for Cardiovascular Science, University of Edinburgh, Scotland), told TCTMD.
Troponin Beyond the Acute Setting
Though high-sensitivity troponin testing is now well established in the setting of suspected ACS, there is emerging evidence that it might have value for assessing risk in patients with stable coronary disease as well. Guidelines recommend risk stratification of patients with chronic CAD using functional testing and invasive or coronary CT angiography, but, Wereski et al note, more than half of MIs occur in patients without obstructive disease, who might not be reliably risk stratified using these techniques.
Other objective tools are therefore needed, the investigators say, noting that high-sensitivity troponin testing is not currently recommended in outpatient settings.
“Studies have previously demonstrated the prognostic role of troponin in selected cohorts with asymptomatic coronary artery disease or a prior history of acute coronary syndrome,” they write. “However, the role of routine troponin testing in patients with stable angina and objective evidence of coronary artery disease has not been explored. It remains unclear whether testing would enhance risk stratification in this setting independent of conventional measures of cardiovascular risk and disease severity.”
Wereski and colleagues designed the MICA study to explore this question. They prospectively enrolled 4,240 patients who had symptoms suggestive of stable angina and were referred for outpatient coronary angiography from six secondary or tertiary care hospitals to the Royal Infirmary of Edinburgh. Cardiac troponin levels were measured before angiography using the ARCHITECTSTAT high-sensitivity troponin I assay (Abbott), with clinicians blinded to the results.
Overall, angiography revealed some degree of coronary disease in 92%, and the analyses focused on these 3,888 patients (median age 67 years; 30.4% women). About two-thirds had obstructive disease (stenosis ≥ 70% in at least one major epicardial coronary artery or stenosis ≥ 50% in the left main stem artery), and the rest had nonobstructive disease.
The median troponin concentration was low overall (3.3 ng/L), but it was higher in those with versus without CAD (3.4 vs 1.9 ng/L; P < 0.001).
Among the patients with CAD, most had troponin concentrations that were considered low, defined as < 5 ng/L (64.5%). Another 31.3% had intermediate levels (5 ng/L to the sex-specific 99th percentile) and 4.2% high levels (above the sex-specific 99th percentile).
Follow-up lasted a median of 2.4 years, and during this time, 6.4% of patients with CAD and 1.7% of those without coronary disease had an MI and/or died from cardiovascular causes (primary outcome).
In the CAD cohort, troponin concentrations were about twice as high in patients who had an event (median 6.7 vs 3.3 ng/L; P < 0.001). The rate of the primary outcome was roughly four times higher among those with high versus low troponin levels (6.13 vs 1.58 per 100 patient-years).
As a continuous measure, a rise in troponin concentration was associated with a greater risk of the primary outcome after adjustment for CV risk factors, CAD severity defined using the Duke prognostic index, and other factors affecting troponin values, including heart failure and renal dysfunction (adjusted HR 2.3; 95% CI 1.7-3.0 per log10 troponin increase).
Adding troponin concentration to the Duke prognostic index improved discrimination for the primary outcome (area under the curve 0.70 vs 0.63; P < 0.001).
The investigators identified 10 ng/L as the troponin threshold above which patients had a relative 50% increase in the risk of MI or CV death compared with levels below 5 ng/L. Of the patients with CAD, 16.7% had troponin levels above this cutoff, and this group experienced a 14.1% rate of the primary outcome during follow-up. “This information could help clinicians to identify those patients with chronic coronary artery disease who are most likely to benefit from treatment intensification,” Wereski et al write.
‘A Robust Barometer of Cardiovascular Health’
In an accompanying editorial, Yader Sandoval, MD (Minneapolis Heart Institute, Abbott Northwestern Hospital, MN), and Allan Jaffe, MD (Mayo Clinic, Rochester, MN), point out that high-sensitivity troponin testing has been evaluated in stable CAD before, with studies showing that increased levels of troponin are associated with greater inducible ischemia, worse LVEF and diastolic function, the presence of vulnerable plaque features, and a greater risk of major adverse cardiovascular events.
The findings of the current study reinforce the concept that this test can improve the risk stratification of patients with stable CAD, they say.
Speaking with TCTMD, Sandoval said the standard of care for the evaluation of these types of patients includes stress tests and coronary CT. “These are good tests and that's the reason we use them in clinical practice,” he said. “But even though they're good, they may sometimes not be available or possible in certain patients, and there are also patients without obstructive coronary disease on coronary CT or myocardial ischemia on functional testing that remain at risk. And this is where troponin, which is a widely available test and a recognized potent risk-stratification tool, may complement the evaluation of these patients.”
Cardiac troponin, he stressed, “has been demonstrated again and again to be a robust barometer of cardiovascular health and a really good measure of risk.”
The most unique finding of the study, Sandoval said, is the hypothesis-generating signal that patients with troponin levels above 10 ng/L might benefit from coronary revascularization, which contrasts with a prior analysis of the BARI 2D trial. The disparate findings could be related to differences in the troponin assays used or in the patient populations—all patients in MICA had symptoms, whereas a proportion of BARI 2D participants did not.
In a broader sense, the current analysis represents the evolution of high-sensitivity troponin as a test that has potential applications beyond the acute setting, Sandoval indicated.
“Guidelines do not recommend this at present in patients with chronic coronary artery disease,” he said. “We clearly still need more studies, more validation, but that's where this test is heading. It's shifting from a test being applied largely in the acute setting to one that is now increasingly applied in the outpatient setting in stable patients, such as in cardio-oncology applications, primary or secondary prevention, and pending more studies, maybe even risk stratification of patients with chronic coronary syndromes.” He noted, too, that this move to the outpatient setting could be facilitated by point-of-care troponin assays, which are not that far off.
Another potential application for high-sensitivity troponin testing could be for monitoring periprocedural myocardial injury in patients undergoing PCI, Sandoval said, adding that further studies are needed to validate that approach as well.
Wereski said that before recommending routine use of high-sensitivity troponin testing in outpatient settings, implementation studies are needed to determine how the results affect clinician judgment and patient outcomes related to changes in additional testing and/or treatment. He said his research group hopes to do a pilot study among patients coming in for coronary angiography in which clinicians will be given the results of troponin testing and any changes in testing and treatment will be recorded. That would precede any potential randomized trial evaluating the clinical impact of this strategy.
Todd Neale is the Associate News Editor for TCTMD and a Senior Medical Journalist. He got his start in journalism at …
Read Full BioSources
Wereski R, Adamson P, Daud NSS, et al. High-sensitivity cardiac troponin for risk assessment in patients with chronic coronary artery disease. J Am Coll Cardiol. 2023;82(6):473-485.
Sandoval Y, Jaffe AS. The evolving role of cardiac troponin: from acute to chronic coronary syndromes. J Am Coll Cardiol. 2023;82(6):486-488.
Disclosures
- The study was funded by the British Heart Foundation and supported by DataLoch, which is funded by the Data Driven Innovation program within the Edinburgh and South East Scotland City Region Deal.
- Wereski reports support from clinical research training fellowships from the Medical Research Council.
- Sandoval reports having been on advisory boards for Abbott Diagnostics, Roche Diagnostics, Philips, and Zoll, and holding multiple patents.
- Jaffe reports having consulted for Abbott, Roche, Siemens, Beckman Coulter, Ortho, Radiometer, Astellas, Spinchip, LuminraDx, and RCE technologies, and holding multiple patents.



Comments