Incidental Thrombi on Device Leads Common, but Seemingly Innocuous
There remains a need, however, for further studies to investigate potential longer-term consequences.
Roughly one out of every five patients with an implantable device who is undergoing lead extraction will have incidental thrombi found on the transvenous leads, new prospective data show. The clots seem to have little in the way of clinical significance, however, at least in the short term.
Indeed, the rate of major adverse clinical outcomes through a median follow-up of 9 months was not significantly different between patients with versus without lead thrombi (7% vs 5%; P = 1.00), according to researchers led by Gordon Ho, MD, and Prerana Bhatia, MD (both University of California, San Diego).
Postoperative hospital length of stay did not differ between groups either, they report in a study published online February 27, 2019, ahead of print in JACC: Clinical Electrophysiology.
Ho told TCTMD that thrombi are commonly seen on pacemaker and implantable cardioverter-defibrillator leads but that the appropriate management of these incidental findings is not clear. There has been some question about the need for anticoagulation, he added, but patients with thrombi were not routinely anticoagulated in the current cohort unless there was another indication.
“And yet we still found no differences in outcomes,” Ho said. “So potentially this study does suggest that it may be safe to not start anticoagulation for small thrombi.”
Moreover, there is a theoretical concern that using laser or mechanical sheaths can shear off thrombi from the leads during the extraction process and increase embolization risk, but there was no evidence of that occurring in this study, which “suggests that it is safe to extract these patients with these thrombi” without needing to convert to surgery, Ho said.
Commenting for TCTMD, Roger Carrillo, MD (Palmetto General Hospital, Hialeah, FL), agreed, saying the findings line up with his own data showing that small thrombi on leads are not associated with any major clinical events.
Still, he said, it’s important to use transesophageal echocardiography before lead extractions—as was done in this study—to document the presence of thrombi and guide appropriate follow-up for potential complications. “Not knowing about it, to me, is not a good strategy,” Carrillo said.
Dearth of Patient, Lead Characteristics Tied to Thrombi
The frequency and clinical significance of thrombi on transvenous leads in patients undergoing lead extraction are not well defined, with prevalence estimates ranging widely from 1.4% to 30%. The best strategy for managing these incidental findings is unclear.
Not knowing about [thrombi], to me, is not a good strategy. Roger Carrillo
To explore the issue, the investigators performed a prospective study of 108 patients with 237 transvenous leads who were referred for lead extraction for a noninfectious reason (most commonly device upgrade, lead fracture, or malposition). All patients underwent preoperative transesophageal echocardiography to look for lead thrombi. Lead extraction was performed using traction alone (13%) or traction combined with laser sheaths (81%) or mechanical sheaths (6%).
Overall, thrombi were found in 18.5% of patients and on 12.2% of leads. All were under 2 cm, and most (86%) were found in the right atrium rather than the right ventricle.
The only clinical characteristic associated with the presence of lead thrombi was younger patient age. No lead features were tied to the finding, and in particular, recalled leads were not more likely to have thrombi than others.
In terms of outcomes, there were no deaths, MIs, or symptomatic pulmonary emboli seen in patients with lead thrombi; one patient who was on warfarin before and after lead extraction had a stroke 3 months after the procedure. “This patient also had atrial fibrillation and subtherapeutic INRs which were a more likely etiology of his cerebrovascular accident than embolization of the lead thrombus,” the authors note.
Among patients without lead thrombi, there were four deaths, one TIA, and one MI.
Ho said that even though the study did not show any short-term consequences of lead thrombi, there is a need for further studies to evaluate any potential longer-term problems, such as the development of chronic thromboembolic pulmonary hypertension. To that end, his team continues to follow the current cohort.
In the meantime, Ho said, “I think these results give us more confidence that we can go ahead and safely extract and not really change our approach,” which includes not routinely anticoagulating patients with lead thrombi in the absence of other indications.
That’s consistent with Carrillo’s view. Noting that he does not start anticoagulation in the presence of lead thrombi unless there are other reasons to do so, he said, “It seems safe if you have these small thrombi to undergo a procedure like lead extraction.”
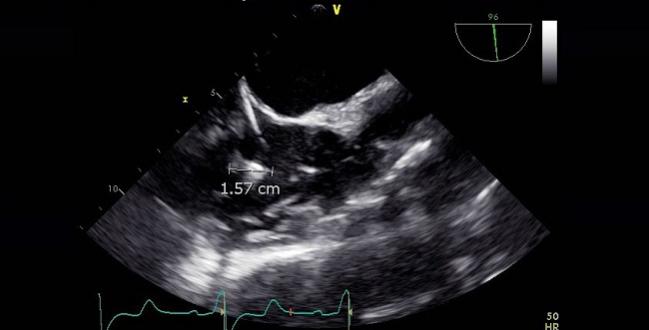
Photo Credit: Gordon Ho, MD. Mobile thrombus (1.6 cm) detected using periprocedural transesophageal echocardiography on an RV implantable cardioverter-defibrillator lead.
Todd Neale is the Associate News Editor for TCTMD and a Senior Medical Journalist. He got his start in journalism at …
Read Full BioSources
Ho G, Bhatia P, Mehta I, et al. Prevalence and short-term clinical outcome of mobile thrombi detected on transvenous leads in patients undergoing lead extraction. JACC Clin Electrophysiol. 2019;Epub ahead of print.
Disclosures
- Ho reports receiving fellowship support from Abbott Laboratories, Boston Scientific, Medtronic, and Biotronik and owning equity in Vektor Medical.
- Bhatia and Carrillo report no relevant conflicts of interest.


Comments