Infective Endocarditis Related to Injecting Opioids on the Rise in Ontario
Risk may vary by type of opioid, which could have implications for deciding which drugs are made available on the market, a researcher says.
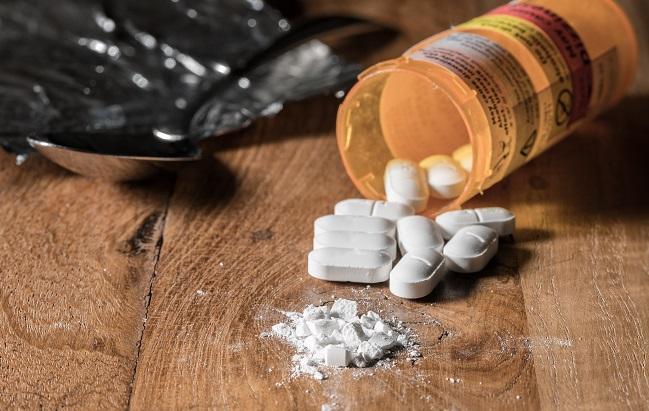
Rates of infective endocarditis (IE) related to injection drug use climbed during a recent 9-and-a-half-year period in Ontario, and the trend seems to be related to a steady increase in prescriptions for hydromorphone, new data show.
While the study highlights a “compelling temporal association,” investigators adopted a cautious tone, particularly when it comes to directly attributing prescriptions of hydromorphone with this severe complication of intravenous drug use.
Further research “should endeavor to draw closer links between exposure and outcome, using individual prescription drug exposure, urine toxicology results or sampling of used drug injection equipment,” lead author Matthew Weir, MD (Western University, London, Canada), and colleagues write in a study published in the January 28, 2019, issue of CMAJ.
Nonetheless, the investigators, including senior author Michael Silverman, MD (Western University), “believe that hydromorphone is a factor leading to our rising endocarditis rates.”
Canada, like the United States, is in the midst of an opioid epidemic. Many users crush oral opioids and dissolve them in a solution for injection use, a practice that carries a risk of IE, explained Silverman.
The current study came about after the researchers learned about differences in the way certain opioids are injected. Traditional controlled-release oxycodone (OxyContin; Purdue Pharma) dissolves much more easily than hydromorphone. Hydromorphone leaves a residue in the equipment used to prepare it for injection, so many users of the drug will use the same equipment repeatedly, a practice that is less likely to occur with oxycodone. That behavior, Silverman explained, could lead to a greater risk of contamination, bacteremia, and IE with hydromorphone.
Toward the end of 2011, Canadian regulators pulled traditional controlled-release oxycodone—the dominant long-acting opioid available—from the market, and Purdue Pharma introduced a new tamper-resistant formulation. The situation presented a natural experiment, and investigators hypothesized that the loss of the earlier formulation of controlled-release oxycodone would result in greater use of hydromorphone and, in turn, increased risks of bacteremia and IE.
When the group examined health administrative databases from Ontario, they identified 60,529 hospital admissions among people who inject drugs between April 2006 and September 2015.
Overall, 1.2% of patients had evidence of IE related to injection drug use, but the rate climbed steadily during the study period. Although there were 13.4 admissions per quarter on average in the period before traditional controlled-release oxycodone was removed from the market and 35.1 per quarter after, the regulatory move was not associated with an immediate uptick in related IE cases as the researchers had hypothesized.
“Rather, the risk of infectious endocarditis appeared to have increased earlier and in parallel with the rise in hydromorphone prescriptions,” the authors explain, noting that the proportion of opioid prescriptions that were for hydromorphone was 16% at the beginning of the study period and 53% at the end.
Silverman acknowledged that the study—which is subject to a number of limitations, including the use of administrative data and the lack of information on use of heroin and other illicit opioids—cannot establish a causal relationship between injecting hydromorphone and higher rates of IE, but he said that additional studies expected to be published soon bolster that connection.
“This isn’t the end of the story,” he said. “We do think we’re going to have even stronger data coming out soon about the association.”
For right now, the study “does raise the issue that hydromorphone, particularly the long-acting [formulation], may be . . . driving endocarditis rates,” Silverman said, noting that it has been thought that hydromorphone is less likely to cause addiction and overdose compared with oxycodone. “While those things may be true, it raises the issue that that switch may have increased another complication that we weren’t aware of.”
The study also highlights the need to investigate the way people are injecting different drugs because the risks might vary, Silverman said.
“We probably should not lump all drugs injected as [having] the same risk for endocarditis, and as we study this further, that may have policy implications in terms of which drugs are made available on the market,” he said. “Realizing that some will be diverted and used this way, we should be aware of the potential adverse effects.”
Todd Neale is the Associate News Editor for TCTMD and a Senior Medical Journalist. He got his start in journalism at …
Read Full BioSources
Weir MA, Slater J, Jandoc R, et al. The risk of infective endocarditis among people who inject drugs: a retrospective, population-based time series analysis. CMAJ. 2019;191:E93-E99.
Disclosures
- The study was supported by ICES Western, which is funded by an annual grant from the Ontario Ministry of Health and Long-Term Care. Core funding for ICES Western is provided by the Academic Medical Organization of Southwestern Ontario, the Schulich School of Medicine and Dentistry, Western University, and the Lawson Health Research Institute.
- Weir and Silverman report no relevant conflicts of interest.


Comments