Inferior Vena Cava Filter Use Fell After FDA Warning but Remains High
Pointing to probable overuse, one expert says doctors need to figure out a better way to identify patients who will most benefit from filters.
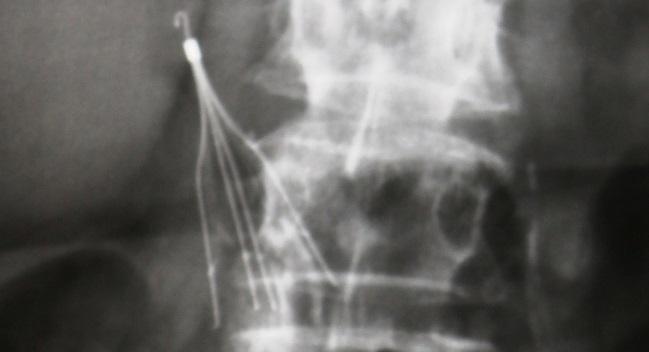
Use of inferior vena cava (IVC) filters declined in the United States following a 2010 safety communication from the US Food and Drug Administration (FDA), although the rate of implantation remains much higher than that seen in Europe, according to a new analysis.
“Given the short- and long-term complications associated with [filter] placement, the use of these devices should be mostly reserved for those patients with an absolute indication like active bleeding,” lead author Satyajit Reddy, MD (Temple University Hospital, Philadelphia, PA), and colleagues write. “Because the rate of [IVC filter] implantation in five large European countries is less than 3 per 100,000 population, we believe that the appropriate implantation rate in the United States should be similar to or lower than the rate observed in Europe.”
As the authors report in a research letter published online July 10, 2017, ahead of print in JAMA Internal Medicine, the rate of implantation in the United States in 2014, the final year of the study period, was 39.1 per 100,000.
In an accompanying editor’s note, Rita Redberg, MD (University of California, San Francisco), writes that the analysis “documents continued unacceptably high rates of IVC filter use after the FDA warning and continued lack of evidence of benefit.”
Citing “definite harms” associated with the filters and going further than recommending a reduction in implantation rates, Redberg argues that “there should be a moratorium on their use unless or until there are data showing efficacy greater than risk.”
But the senior author of the analysis, Riyaz Bashir, MD (Temple University Hospital), told TCTMD that he thinks that is “a little bit too aggressive a stance.”
Certain patients, including those with a blood clot who are actively bleeding, are prime candidates for IVC filter placement because they cannot receive anticoagulation, he said. “So I would not want the physicians’ hands to be tied behind their backs by not allowing them to put a filter in,” Bashir said, adding, “I think we should definitely reduce our filter implantation rates and every single filter implantation [should] be carefully decided based on individual situations.”
Commenting for TCTMD, Elliott Haut, MD (Johns Hopkins Medicine, Baltimore, MD), said a moratorium would be difficult to implement because IVC filters are FDA approved, widely used in situations deemed appropriate by physicians, and recommended by some (but not all) national medical societies in certain settings.
“I don’t think that’s a reasonable, even potential option. I just don’t know how they could logistically do that,” Haut said about Redberg’s proposed freeze on IVC use. “Now, I would say that I would strongly push for better research on the topic.”
Existing research is mixed, Haut said, pointing out that even though there are many studies suggesting that IVC filters do not have a clinical benefit, others indicate that implantation of the devices can reduce rates of pulmonary embolism (PE) and fatal PE. He added that he thinks there are legitimate differences of opinion about the benefits of filters, which at least partly explains why use remains high in the United States.
We know they help some patients. We just don’t know how exactly to pick the one-in-a-thousand person that’s going to need it and benefit from it the best. Elliott Haut
Still, “the rate is higher than it probably should be,” Haut said. But, he added, it could be that IVC filters are being overused in some patient populations and underused in others.
“We know they help some patients. We just don’t know how exactly to pick the one-in-a-thousand person that’s going to need it and benefit from it the best,” he said. “So the broad approach of putting tons and tons and tons in to prevent one fatal pulmonary embolism . . . is probably not cost-effective, probably not efficient, probably not safe for patients, but I think we have to figure out a better way to know which are the patients who are going to benefit from it.”
Complications and an FDA Warning
On August 9, 2010, JAMA Internal Medicine published a study showing that there was a high rate of potentially life-threatening fracture and embolization associated with two IVC filters manufactured by Bard. On the same day, the FDA issued a safety communication discussing 921 filter-related adverse events, including device migration, fracture, and thrombosis, that were reported over a 5-year period. The agency recommended removing filters as soon as protection against pulmonary embolism is no longer needed.
Reddy et al wanted to determine whether the warning had any effect on filter use in the United States, and they turned to the National Inpatient Sample. Between 2005 and 2014, an estimated 1.13 million patients underwent implantation of an IVC filter. The implantation rate increased by 22.2% from 2005 to 2010, but then declined by 29.0% from 2010 to 2014.
The reduction did not appear to be related to a change in hospitalizations related to venous thromboembolism, which remained steady during the latter part of the study period.
Other factors aside from the FDA warning could be playing into the decline in IVC filter use, the authors note. The reduction began 2 years before reimbursement for the procedure was decreased via bundling the associated Current Procedural Terminology codes, but lower reimbursement will likely drive implantation rates down in the future, they say. In addition, they say, it is possible that the introduction of non-vitamin K antagonist oral anticoagulants will impact use, although that remains unclear.
‘Dirty Little Secret’
One aspect of the debate on IVC filters that is starting to garner more attention is the “dirty little secret” that many of these removable filters are never retrieved, Haut said, noting that this can have a big impact on risk-benefit calculations. The risk part of the equation will be lower if a physician assumes the filter will be removed after a short period of time rather than left in place over the long term.
Redberg points out that there is evidence suggesting that the longer a filter is left in place, the higher the risk of fracture.
Thus, removing the filters as soon as possible—as recommended by the FDA—needs to be more strongly considered, Haut said.
Bashir agreed: “All physicians have to make sure that any time a filter goes in, there is a plan in place to make sure that that filter comes out because there are a lot of complications [from] leaving these filters in, and that’s a message that needs to be conveyed repeatedly to every physician.”
Todd Neale is the Associate News Editor for TCTMD and a Senior Medical Journalist. He got his start in journalism at …
Read Full BioSources
Reddy S, Lakhter V, Zack CJ, et al. Association between contemporary trends in inferior vena cava filter placement and the 2010 US Food and Drug Administration advisory. JAMA Internal Med. 2017;Epub ahead of print.
Redberg RF. Continued high rates of IVC filter use after US Food and Drug safety warning. JAMA Internal Med. 2017;Epub ahead of print.
Disclosures
- Bashir reports being a cofounder and holding equity interest in Thrombolex Inc.
- Reddy, Redberg, and Haut report no relevant conflicts of interest.


Comments