Lower Socioeconomic Status Linked to Worse In-Hospital Cardiac Arrest Outcomes
While discrimination by staff is one theory, other confounders may involve diagnosis and advocacy, Swedish research concludes.
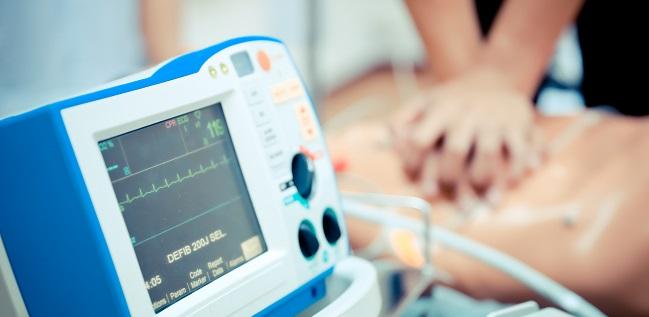
People with lower levels of education and/or income experience delays in CPR and worse survival after sudden, in-hospital cardiac arrest, a Swedish study confirms. The findings challenge the view that hospitalization serves to equalize care across patient groups, researchers say.
“Because the afflicted patients are already in the hospital, an association between cardiac arrest treatment and survival should less likely be due to structural socioeconomic status differences in access to care (e.g. proximity of emergency medical services),” Jens Agerström, PhD (Linnaeus University, Kalmar, Sweden) explained. On the contrary, however, their study of in-hospital cardiac arrests found that those on the low end of the socioeconomic spectrum also were less likely than those on the higher end to receive the monitoring and attention they need.
“It is troublesome that this group of patients is prioritized less when it comes to prophylactic treatment despite having a seemingly greater need for this due to poorer initial health,” Agerström and colleagues note. “The argument that they are too ill to receive such treatment appears invalid because the studied sample only contains patients who received CPR.”
They suggest that cardiac arrest teams may need more training in both recognizing their own bias and understanding how prejudicial treatment based on socioeconomic status can translate into discriminatory care. The study was published online last month in the European Heart Journal.
A Fairly Surprising Result
Commenting for TCTMD, Benjamin S. Abella, MD (University of Pennsylvania, Philadelphia), said the study is “provocative and suggestive that there may be a relationship between socioeconomic status and in-hospital cardiac arrest, although this is a fairly surprising result.” He further cautioned that there may be other potentially unmeasured confounders, which could have played a role in the findings that the authors should explore further.
“One of the things that they found was that socioeconomic status was linked to whether people were in monitored or unmonitored beds,” Abella commented. “When they then did a statistical analysis based on monitoring or unmonitoring, the CPR delivery relationship with socioeconomic status went away. So, it's not entirely clear to me that socioeconomic status truly played a direct role in whether people got CPR or not, but rather the kinds of diagnoses that people came in with may have been important.”
Using the Swedish Register of Cardiopulmonary Resuscitation, Agerström and colleagues examined data on 24,217 patients with in-hospital cardiac arrest between 2005 and 2018. Quartiles of socioeconomic status were determined based on highest level of completed education and annual income.
It's not entirely clear to me that socioeconomic status truly played a direct role in whether people got CPR or not, but rather the kinds of diagnoses that people came in with may have been important. Benjamin Abella
In most cases (59.1%), there was no CPR delay. The average duration of CPR was 16.2 minutes, and half of all patients survived. By education status, those with higher education were less likely than those with lower education to have a CPR delay (P = 0.012), with similar findings by higher versus lower income level (P = 0.038). Those in the highest education quartile also had shorter CPR duration than those in the lowest education quartile (P = 0.039), although the association between income and CPR duration was not statistically significant (P = 0.674).
While education status was not associated with CPR, patients with higher income were more likely to survive CPR than those with lower income (P = 0.004). Additionally, more higher-education patients survived to discharge with good neurologic outcome than lower-education patients (P < 0.001), and the same association was true for higher versus lower income (P < 0.001).
“The results revealed that highly educated patients (P < 0.001) and patients with higher income (P = 0.001) were significantly more likely to have their heart rhythm monitored prior to the onset of the [cardiac arrest], even with fixed effects for hospital and year in the regression and when controlling for demographic characteristics (age, gender, ethnicity) and comorbidity,” Agerström and colleagues write. Heart rhythm monitoring was associated with a variety of better outcomes, including less CPR delay, shorter CPR duration, and improved immediate and post-discharge survival.
Role of Support Systems and Family, Physician Advocacy
While the authors suggest that implicit bias and prejudices among hospital staff may be to blame for who is monitored and who gets faster CPR, Abella said he’s not entirely convinced, and reiterated that individual diagnoses and reasons for admission likely play a significant role.
“I can't say whether this was the case in Sweden, but often in the United States, patients with low socioeconomic status end up with more advanced infectious disease that could have been treated as an outpatient, such as more diabetic complications from not having good follow up. So, those patients would not necessarily end up on a monitored bed,” he said. “It stands to reason that people who are monitored will get CPR earlier and more often than people who are unmonitored.”
Another important potential confounder that correlates with socioeconomic status, Abella added, is family advocacy.
“Folks who are of a higher socioeconomic status and have more education often have better advocacy by their families, who also may be more sophisticated and understand how to pull the levers of the healthcare system more effectively and advocate for their patients to get monitored beds, or advocate for them to be near the nursing station and to be monitored more carefully,” he explained. “If you take away the CPR part, the fact that critical illness is better survived by [those with] higher socioeconomic status makes a lot of sense to me from the family advocacy standpoint.”
Lastly, Abella said physician advocacy could play a role, too.
“If you do not have a regular physician, or a good relationship with a physician, that definitely tracks with socioeconomics. So, when you're in the hospital, you may not have someone advocating for you from the physician side,” Abella said. While that scenario constitutes a kind of discrimination of its own, it’s not the same as saying that healthcare teams are openly discriminating against patients based on education or income.
“The interaction of socioeconomics and hospital-based care is important and worthy of study, but for me, this study, raises more questions than answers,” he added.
L.A. McKeown is a Senior Medical Journalist for TCTMD, the Section Editor of CV Team Forum, and Senior Medical…
Read Full BioSources
Agerström J, Carlsson M, Bremer A, et al. Discriminatory cardiac arrest care? Patients with low socioeconomic status receive delayed cardiopulmonary resuscitation and are less likely to survive an in-hospital cardiac arrest. Eur Heart J. 2020;Epub ahead of print.
Disclosures
- Agerström reports no relevant conflicts of interest.
- Abella reports having received speaking honoraria and research funding from BD.


Comments