Many Resuscitated Arrests Don’t Have an Underlying Cardiac Cause
Earlier recognition of noncardiac causes of out-of-hospital arrests may help boost the stubbornly low survival rates.
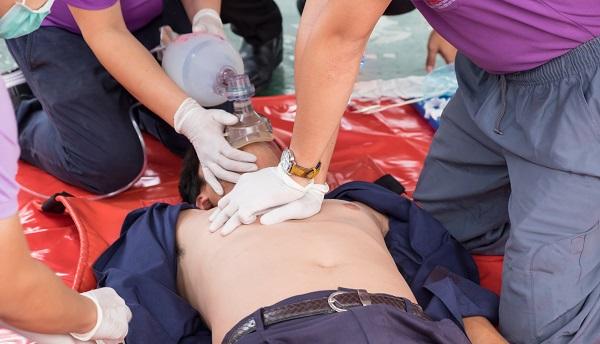
Though they’re called resuscitated sudden cardiac arrests, many such events do not, in fact, have an underlying cardiac cause, which has implications for both patient care and clinical research, investigators have found.
Of patients who suffered an out-of-hospital cardiac arrest (OHCA) and survived long enough to be hospitalized in San Francisco County over a roughly 4-year span, most (69.1%) had an underlying arrhythmic cause, but a sizeable minority (27.1%) had noncardiac conditions to blame. Another 3.8% were classified as “nonarrhythmic/cardiac.”
The distinction mattered when it came to the likelihood of a patient surviving that initial hospital stay. The vast majority of survivors (92%) had an underlying arrhythmic cause, and only one had a noncardiac cause. The bulk of the noncardiac group was made up of patients with underlying neurologic conditions like stroke, intracranial hemorrhage, and seizure, all of whom died.
These findings, published in the May 18, 2021, issue of the Journal of the American College of Cardiology, “suggest that conventional definitions of cardiac arrest poorly specify actual arrhythmic cause; specifying suddenness and separating the outcomes of resuscitated sudden cardiac arrests and sudden cardiac deaths may help to refine future analyses of OHCAs,” researchers led by Santo Ricceri, MD (University of Colorado Anschutz Medical Campus, Aurora, CO), write.
Moreover, they say, “early identification of nonarrhythmic sudden cardiac arrests, such as neurologic emergencies, may be a target to improve OHCA survival.”
What’s in a Name?
Senior author Zian Tseng, MD (University of California, San Francisco), explained to TCTMD that this study “is part of a multipronged effort that I’ve been undertaking for probably the last decade to really understand what we mean when we say sudden cardiac death,” as well as sudden cardiac arrest or OHCA. Definitions for each term can vary depending on the viewpoints of investigators from different specialties, and the terms are sometimes equated with one another, he added.
We keep saving the same cases. . . . How do we save the half that are not cardiac? Zian Tseng
In 2018, Tseng’s group reported results of the POST SCD study, which focused on patients who had an OHCA and did not survive long enough to be admitted to the hospital—ie, sudden cardiac deaths. Of the 525 cases that met World Health Organization (WHO) criteria for sudden cardiac death and were autopsied, 40% did not have an underlying cardiac cause and 56% were arrhythmic. “This is, on the face of it, a little bit of a surprise, but it shouldn’t be a shock. Because why should it necessarily be cardiac when somebody dies suddenly?” Tseng said, noting that ruptured aneurysm, stroke, pulmonary embolism, infection, or overdose, for instance, could be to blame.
For this latest study in JACC, the researchers zeroed in on the patients who had an OHCA during a similar time period but were excluded from POST SCD because they were resuscitated and survived to hospitalization (and thus, did not die suddenly). The underlying causes of the arrests in this analysis, which focused on the 133 resuscitated patients (mean age 67.4 years; 65.4% men) who met criteria for suddenness, were adjudicated based on in-hospital investigations rather than autopsy. Most of these patients (64.7%) died in the hospital, and the rest survived to discharge.
Arrhythmic causes were to blame for more than two-thirds of the resuscitated arrests in this study, higher than the 56% of patients who died suddenly in POST SCD and lower than the 92% of those who were resuscitated and ultimately survived to hospital discharge. “So the further along the chain of survival you get, you’re more likely to be cardiac,” Tseng said. “By the time you’re discharged and make it home or make it to my clinic with a defibrillator, you’re cardiac 92% of the time.”
That makes sense, Tseng explained, because resuscitation strategies—including defibrillators and CPR—are geared toward addressing arrhythmic causes. “Those are going to save the cardiac cases. The noncardiac causes are completely unaddressed by our resuscitation strategies,” he said.
That’s reflected in the factors that were independently associated with survival to discharge in this study. An arrhythmic cause (adjusted OR 5.29; 95% CI 1.38-20.34) and an initial rhythm of ventricular tachycardia/fibrillation (adjusted OR 19.26; 95% CI 5.25-70.59) were strongly associated with a greater likelihood of survival, whereas a history of prior stroke was associated with much lower odds of survival (adjusted OR 0.02; 95% CI 0-0.45).
Implications for Patient Care, Research
Tseng said there were a few major implications related to the findings of POST SCD and the current study. The first is that “maybe early identification of actual underlying causes of cardiac arrest would improve our dismal survival rates,” he said. Pointing specifically to the outcomes in patients with underlying neurologic causes, he added that “anything better than 100% mortality would be an improvement.”
He advocated for a “resuscitation-plus” approach that adds more elements to the current advanced cardiac life support measures in order to address potential noncardiac causes of OHCA. For instance, based on the recognition that drug overdose may be confused with cardiac arrest, Tseng suggested that naloxone (Narcan), which can reverse an opioid overdose, could be administered to all patients with an apparent cardiac arrest since there is little risk to using it. Indeed, the growing number of opioid-associated OHCAs led to the recent publication of a scientific statement by the American Heart Association, highlighting the distinct diagnostic and treatment requirements of arrests of this nature.
In addition, because many of the arrests in the current study were caused by neurologic conditions, there might be a way to enhance the rapid on-scene assessment to better identify patients who could benefit more from transfer to a stroke center rather than a cardiac cath lab or patients on oral anticoagulation or antiplatelet therapy who could benefit from reversal agents.
“The next steps would be to really understand and identify the prehospital predictors of these underlying causes to direct more-precise resuscitation strategies,” Tseng said.
Making changes to how OHCA is studied and defined will be important, too. “Until we target those underlying causes, we can’t improve our outcomes and we can’t really study the condition effectively. If you think about all the other studies that have lumped these cardiac arrests or sudden cardiac deaths together, half of the time they’re not cardiac,” which complicates genetic association or molecular studies, Tseng said. “It really requires a precision phenotyping approach, if you will, and that was the goal of our study.” A key takeaway, he added, is that resuscitated sudden cardiac arrest and sudden cardiac death “are not the same thing and should be separated as outcomes.”
Major changes are needed in how the medical community treats and discusses cardiac arrest, because OHCA survival rates have remained stuck at around 10% to 15% for years, Tseng stressed. “We keep saving the same cases. . . . How do we save the half that are not cardiac?”
In an accompanying editorial, Eric Stecker, MD, and Babak Nazer, MD (Knight Cardiovascular Institute, Oregon Health & Science University, Portland), underscore the seriousness of the situation as well, pointing out that “fully 85% of individuals who experience cardiac arrest due to a verified cardiac etiology will die, causing more premature loss of life than most cancers. This emphasizes the importance of efforts to prevent the onset of cardiovascular disease through treatment of the most-important modifiable risk factors: hypertension, elevated low-density lipoprotein, diet/obesity, and smoking.”
Todd Neale is the Associate News Editor for TCTMD and a Senior Medical Journalist. He got his start in journalism at …
Read Full BioSources
Ricceri S, Salazar JW, Vu AA, et al. Factors predisposing to survival after resuscitation for sudden cardiac arrest. J Am Coll Cardiol. 2021;77:2353-2362.
Stecker EC, Nazer B. The shadows of sudden cardiac death. J Am Coll Cardiol. 2021;77:2363-2365.Stecker EC, Nazer B. The shadows of sudden cardiac death. J Am Coll Cardiol. 2021;77:2363-2365.
Disclosures
- The study was funded by the US National Institutes of Health/National Heart, Lung, and Blood Institute (NIH/NHLBI).
- Tseng reports grants from the NIH/NHLBI and the US Centers for Disease Control and Prevention during the conduct of the study, and personal fees from Biotronik outside the submitted work.Tseng reports grants from the NIH/NHLBI and the US Centers for Disease Control and Prevention during the conduct of the study, and personal fees from Biotronik outside the submitted work.
- Stecker and Nazer report no relevant conflicts of interest.



Comments