Mortality Outcomes Similar Whether TAVR Performed in Hybrid OR or Cath Lab
While not necessary, experts argue that a hybrid OR is valuable in treating higher-risk patients with the necessary resources.
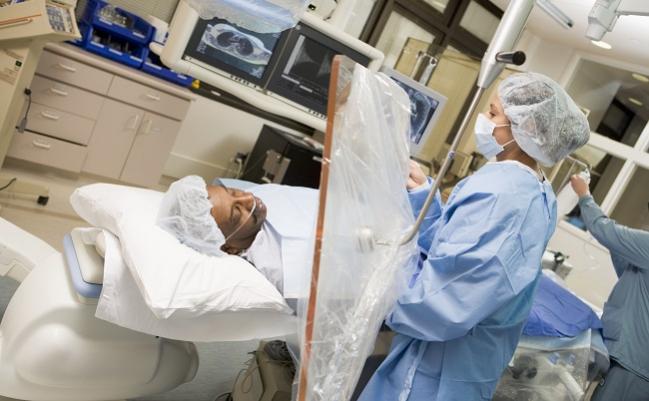
Mortality outcomes for patients undergoing TAVR in France are similar up to 3 years regardless of whether they underwent their procedure in a cath lab or a hybrid operating room (OR), according to new results from the FRANCE TAVI registry.
Despite high enthusiasm in recent years for building hybrid ORs—defined as a roughly 1,000-square-foot space equipped with high quality fluoroscopy and imaging monitors, a table that can accommodate operations and angiography, booms for anesthesia and perfusion equipment, surgical lighting, radiation safety features, and laminar airflow and positive pressure systems—in current and emerging TAVR centers worldwide, the estimated cost of between $1.2 and $5 million dollars has prevented many from doing so. These findings support the performance of TAVR in either location, argue the authors, led by Marco Spaziano, MD (Hopital Privé Jacques Cartier, Massy, France).
For their study, published in the November 12, 2018, issue of JACC: Cardiovascular Interventions, the researchers included 12,121 patients undergoing TAVR in either a cath lab (62%) or hybrid OR (38%) between 2013 and 2015 who were enrolled in the FRANCE TAVI registry. Notably, about one-quarter of centers used both locations for TAVR, but 63% of patients treated at these institutions were still operated on in a cath lab. Also, patients in the cath-lab arm were typically older and had higher risk scores, more CAD, and worse kidney function than those in the hybrid OR group, who had more peripheral vascular disease and a greater prevalence of previous cardiac surgery.
After adjustment for baseline patient differences, mortality was similar between the groups at 30 days. TAVR in the hybrid OR was associated with higher rates of major bleeding and infections, but procedures in the cath lab were linked with a greater prevalence of new pacemaker implantation and greater than mild paravalvular regurgitation.
30-Day Outcomes Based on TAVR Location
|
|
Hybrid OR |
Cath Lab |
P Value |
|
Mortality |
5.1% |
4.7% |
0.63 |
|
Major Bleeding |
6.3% |
4.8% |
0.006 |
|
Infections |
6.1% |
3.5% |
< 0.001 |
|
New Pacemaker Implantation |
15.6% |
14.6% |
0.006 |
|
Paravalvular Regurgitation > Mild |
10.6% |
9.2% |
0.003 |
The mortality outcomes between hybrid OR and cath lab procedures were similar at both 1 year (16.2% vs 15.8%; P = 0.91) and 3 years (36.4% vs 38.4%; P = 0.49). A sensitivity analysis that matched patients based on Logistic EuroSCORE, access site, and use of conscious sedation maintained these results, even when only including the patients treated at institutions that used both TAVR locations.
Until now, some experts have argued that performing TAVR in a hybrid OR rather than in a cath lab improves safety, Spaziano and colleagues write, but notably this study found higher rates of conversion to open surgery among patients treated in the former location. “It is unclear whether this is because of more acute complications (there were not differences between groups with respect to individual procedural complication rates), or because of availability and ease of conversion to surgery,” they write, noting that even so the conversion rates were less than 1% in both arms. Also, conversion to open surgery was not associated with mortality in multivariate models; rather, complications like annulus rupture and aortic dissection themselves were directly linked with poor outcomes.
The authors also write that because of the airflow systems installed, they had anticipated that the infection rate would be lower for procedures conducted in hybrid ORs. Most of the infections in those patients were due to pulmonary and urinary complications associated with endotracheal intubation and bladder catheterization and not so much surgical exposure, they explain.
Lastly, they note the importance of distinguishing between procedure location and procedure invasiveness, as choosing a hybrid OR over a cath lab does not necessarily portent a minimalist approach. “In the FRANCE TAVI registry, it seems that a minimalist approach may have been more commonly used in the cath lab group (as reflected by a higher rate of local anesthesia in the transfemoral subgroup),” Spaziano and colleagues write. “In contrast, the more common use [of] general anesthesia in the hybrid OR group did not translate into more intraprocedural [transesophageal echocardiography] guidance, which is expected in a standard approach.”
Notably, study co-author Thierry Lefèvre, MD (Hopital Privé Jacques Cartier, Massy, France), told TCTMD in an email that at his institution all transfemoral TAVR cases are performed in the cath lab by interventional cardiologists. “[The] hybrid OR is used only for nontransfemoral TAVI procedures or transfemoral TAVIs performed by the surgeons,” he said.
Further, “TAVI should become a PCI-like procedure in the majority of centers—the majority of cases being treated on local anesthesia, without [transesophageal echocardiography], urinary catheters,” Lefèvre argued. “Hybrid OR is nice to have for nontransfemoral TAVR or very complex hybrid procedures such as transapical mitral valve implantations.”
Higher Quality With Hybrid OR
In an editorial accompanying the paper, Kentaro Hayashida, MD, PhD (Keio University School of Medicine, Tokyo, Japan), poses the question of whether a hybrid OR is “a must-have or nice to have.” In Japan, TAVR centers are required to have hybrid ORs and so all 140 there do. In fact, he notes, Japanese registry data have suggested “that a hybrid OR may have played an important role to decrease the mortality of patients who developed severe complications during TAVR in the early learning curve in Japan.”
Hayashida says that it’s hard to know what the surgical conversion data indicate, given how low the rates were. “However, these results suggest that mortality after severe procedural complications may be associated mainly with the ‘suitability’ of surgical conversion, including severity of complications, general status, and availability of surgical conversion, rather than initial procedure location,” he writes.
Commenting on the paper for TCTMD, Isaac George, MD (NewYork-Presbyterian/Columbia University Irving Medical Center, New York, NY), said in an email that “TAVR can be and is being done safely in both a hybrid OR and the cath lab for most patients.” At his institution, higher-risk patients—those "with alternative access, high risk coronary or vascular anatomy, bicuspid valves, other anatomic issues”—currently undergo TAVR in the hybrid OR because it has “full cardiac and open/endo vascular capabilities,” George added.
The economic implications of this study are “less relevant” than some might think, he said, since the hybrid OR “always stays extremely busy with over 100% usage, as multiple specialties can use it. Thus, the trend has been to build more and more multispecialty type rooms that are versatile, not the other way around.
“The bigger issue is the quality aspect that [it] allows treatment for complex, high-risk anatomy,” he continued. “Those patients with higher tendency for major complications may have better ‘rescue’ rates from complications, that is facilitated by being in a hybrid OR with access to surgical instruments, staff, and perfusion. Straightforward, clean anatomy cases can fairly be done in both locations. However, it is the ability to safely treat the higher risk 5-8% of the population that distinguishes a top-level center.”
For this study specifically, George said “it’s a stretch” to call the cohorts equivalent given the retrospective nature of the data. “It is clear that hybrid patients are generally sicker and have more unfavorable anatomy. . . . This is an inherent selection bias as centers preferentially schedule high-risk patients in hybrid rooms over cath labs,” he commented.
Going forward, Lefèvre said, “it will be interesting to see a comparable analysis in other countries and nice to have a randomized study, but I’m not sure that we will see this kind of study in the future.”
Yael L. Maxwell is Senior Medical Journalist for TCTMD and Section Editor of TCTMD's Fellows Forum. She served as the inaugural…
Read Full BioSources
Spaziano M, Lefèvre T, Romano M, et al. Transcatheter aortic valve replacement in the catheterization laboratory versus hybrid operating room: insights from the FRANCE TAVI registry. J Am Coll Cardiol Intv. 2018;11:2195-2203.
Hayashida K. Hybrid operating rooms for transcatheter aortic valve replacement: a must-have or nice to have? J Am Coll Cardiol Intv. 2018;11:2204-2206.
Disclosures
- Lefèvre reports serving as a proctor for Edwards Lifesciences and Abbott and receiving lecture fees from Edwards Lifesciences and Abbott.
- Spaziano reports no relevant conflicts of interest.
- Hayashida reports serving as a clinical proctor for Edwards Lifesciences.
- George reports conflicts of interest with Edwards Lifesciences and Medtronic.


Oscar Berg