Need for Emergency Cardiac Surgery Is Rare After PCI
Even so, centers without on-site surgical backup must have protocols in place should the need arise, Mamas Mamas says.
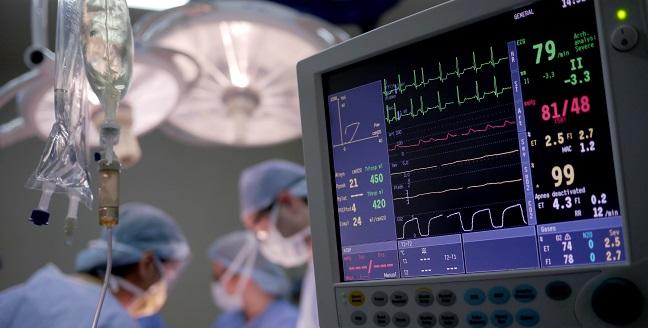
PCI complications that require emergency surgery don’t occur frequently, but when they do—not surprisingly—they’re associated with worse outcomes, national data from England and Wales indicate.
Of nearly 550,000 patients treated over an 8-year period, only 362 (0.07%) required emergency surgery for a complication, most frequently coronary or aortic dissection, coronary perforation, or cardiac tamponade, according to researchers led by Chun Shing Kwok, MBBS (Keele University, Stoke-on-Trent, England).
These patients had greater odds of 30-day mortality (16.0% vs 2.2%; OR 4.41; 95% CI 2.94-6.62) and in-hospital MACCE (14.4% vs 1.9%; OR 1.63; 95% CI 1.07-2.48) as well as a longer average hospital stay (11.2 vs 2.0 days) compared with their complication-free peers, the researchers report in a study published online June 7, 2020, ahead of print in the American Journal of Cardiology.
Those poorer outcomes should not be seen as an argument against allowing PCI at centers that lack on-site surgical backup, senior author Mamas Mamas, BMBCh, DPhil (Keele University), told TCTMD. “There is a whole body of evidence, including from the United Kingdom, to suggest that outcomes in these centers are no different compared to centers where surgery is present, and I think it’s really important to emphasize that these complications are really, really rare,” he said.
“What it does say, however, is that even if it’s a rare event, nonsurgical centers should have a protocol in place about what to do if [emergency surgery] is required,” because the outcomes are so much worse in this situation, he added.
Mamas said there are limited data on the requirement for emergency surgery after PCI, noting that the studies that have been done are relatively outdated. In recent years, PCI has become much safer, highlighting the need for this type of information, which can be useful during the informed-consent process, Mamas said.
For this study, the investigators examined data from the British Cardiovascular Intervention Society (BCIS), which collects data on 99% of all PCIs performed in England and Wales within the National Health Service. The analysis included 549,303 patients who underwent PCI—roughly two-thirds for ACS and one-third for stable angina—between 2007 and 2014. During that time span, the rate of emergency cardiac surgery declined from 0.09% to 0.06%. Mamas said that might be related to greater use of intravascular imaging and procedure planning and to improvements in available equipment, such as covered stents.
The factors most strongly associated with emergency surgery were:
- Receipt of circulatory support (OR 39.20; 95% CI 27.75-55.36)
- Aortic dissection (OR 28.39; 95% CI 14.59-55.26)
- Coronary dissection (OR 18.50; 95% CI 13.60-25.18)
- Coronary perforation (OR 7.86; 95% CI 4.27-14.46)
- Cardiac tamponade (OR 6.77; 95% CI 3.13-14.66)
In addition, the presence of on-site surgical backup was itself associated with greater odds of emergency surgery (OR 2.15; 95% CI 1.56-2.97), which Mamas called “slightly surprising,” and of 30-day mortality following emergency cardiac surgery (OR 1.26; 95% CI 1.20-1.33).
It could be that surgical centers tend to take on more complex patients, he said. But it might also reflect a phenomenon in which patients who have catastrophic PCI complications at nonsurgical centers don’t survive long enough to reach the operating room, resulting a somewhat healthier cohort of patients who survive a transfer from a nonsurgical to a surgical center and a sicker group treated with emergency surgery at hospitals with on-site backup.
In their paper, the researchers point out that there are multiple studies showing comparable PCI results in sites with versus without on-site surgical backup, including the CPORT-E trial, an analysis of data from the Swedish Coronary and Angiography and Angioplasty Registry (SCAAR), and a prior analysis of the BCIS database.
Todd Neale is the Associate News Editor for TCTMD and a Senior Medical Journalist. He got his start in journalism at …
Read Full BioSources
Kwok CS, Sirker A, Nolan J, et al. A national evaluation of emergency cardiac surgery after percutaneous coronary intervention and post-surgical patient outcomes. Am J Cardiol. 2020;Epub ahead of print.
Disclosures
- The study was supported by a grant from the Research and Development Department at the Royal Stoke Hospital. Kwok’s PhD tuition is supported by Biosensors International.
- Kwok and Mamas report no relevant conflicts of interest.


Comments