PFO and Migraine? New Study Zeros in on Atrial Septal Aneurysms
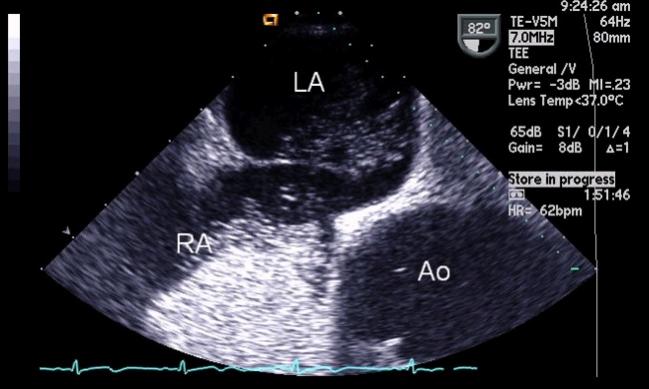
A new study is once again drawing the link between a patent foramen ovale (PFO) and migraine headaches—this time researchers are zeroing in on the subset of patients with both a PFO and atrial septal aneurysm (ASA). According to Roel J. R. Snijder MD (St. Antonius Hospital, Nieuwegein, the Netherlands), and colleagues, who recently published findings in the Journal of the American Heart Association, their cohort represents the largest series linking PFO plus ASA to migraine with aura.
PFO closure studies, they conclude, should focus on this specific intra-atrial anomaly.
Speaking with TCTMD, Snijder acknowledged that this field of research has struggled with enrollment problems and that limiting eligibility criteria even further will be problematic. “In our group of patients, which was quite a large group, we did find a very strong association between PFO with ASA and migraine with aura, but is it worth doing more research? Maybe,” he said. Migraine remains a big problem and for patients who have not responded to best medical treatment, there could be “benefit from PFO closure, but I don’t know that you’ll find a large enough group to do a randomized trial.”
Migraines and PFO: A Muddy History
A range of observational studies—although not all—have documented a link between PFO and migraine, and especially migraine with aura. The hypothesis linking the two conditions is that microemboli or vasoactive components of platelets crossing the PFO may play a causative role, theories supported by observations that high-dose antiplatelet drugs seem to be helpful in some migraine sufferers. However, three randomized trials to date, MIST, PRIMA, and PREMIUM, have all failed to show a benefit of PFO closure over a sham procedure—or medical therapy in the case of PRIMA—in reducing migraines. MIST was also plagued by misconduct and a lengthy libel suit.
The current study looked at 2,349 consecutive patients undergoing transesophageal echocardiography at two centers. Of these, 889 patients had tests that included agitated saline “bubble” exams and also completed migraine questionnaires.
PFO was found in 23.2% of the patients, with 6.9% having PFO plus ASA. Subjects who commonly experienced migraine plus aura were significantly more likely to have PFO plus ASA than were patients with no migraine history (18.1% versus 6.1%, 95% CI 1.86-7.44). Of note, neither PFO without ASA nor isolated ASA were significantly associated with migraine or migraine plus aura.
Snijder says that while his center closes PFOs for prevention of recurrent cryptogenic stroke, he and his colleagues do not use closure devices for the treatment of migraine. He himself thinks that the microthrombi hypothesis is worth exploring further, but acknowledges that even the PFO closure for stroke trials “had a lot of critics—that’s the nicest way to say it.” As such, while he thinks the connection hinted at in his paper is important for the field, he couldn’t say whether future studies could possibly find enough patients with PFO, ASA, migraine, plus aura to move forward.
Other Possibilities
Peter Wilmshurst, MD (Royal Stoke University Hospital, Stoke-on-Trent, England), the MIST co-principal investigator who ultimately blew the whistle on trial conduct and reporting, reviewed Snijder et al’s paper for TCTMD. For Wilmshurst, the study helps cement a hypothesis observed in previous publications, namely that the prevalence of migraine with aura is related to the degree of right-to-left shunting. “The degree of shunting across a PFO is largely related to its diameter,” Wilmshurst said in an email. “Atrial septal aneurysms—ie, very mobile atrial septa—are present in people with the largest PFOs. So one should not be surprised that migraine with aura is associated with atrial septal aneurysms, which are a surrogate marker for the diameter of the PFO and hence of the degree of shunting.”
Also commenting on the paper for TCTMD, Robert J Sommer, MD (Columbia University Medical Center, New York, NY), was not persuaded that patients with both PFO and atrial septal aneurysm are the only subgroup in whom research should move forward. He noted that 40% of patients with migraine plus aura have a PFO—“that’s well documented”—but said reducing this to patients who also have ASA would limit potential study populations to just 18% of migraineurs.
“I can tell you, we’re doing a lot of migraine research and we know that there are patients with large PFOs, patients with small PFOs, patients with and without atrial septal aneurysms, and even patients without aura who respond to therapy, so I think it’s an interesting and large collection of patients.”
To TCTMD, Sommer said he believes he and his coinvestigators “are literally on the verge of a major breakthrough” in migraine treatment. They are pursuing a different migraine treatment, one also potentially related to the microemboli PFO hypothesis. The TRACTOR trial is testing ticagrelor for refractory migraine among patients with both migraine and PFO, based on the possibility that microemboli themselves are making their way to the brain, or that vasoconstrictive compounds released by platelets may reach the cerebral circulation and trigger migraine.
He also has additional device-based trial ideas in the planning stages that are based on the notion that P2Y12 inhibitors “may not only be a treatment for migraine [but] may also be the test we need to pick the correct patients who are going to respond to PFO closure, . . . because migraine is a multifactorial disease and only in some patients is the PFO causative. In many, the PFO is incidental. But if we can figure out who is going to respond before we do the closure, [we could] have a fantastically positive study.”
Of Snijder’s paper, however, Sommer concluded: “I don't think it breaks any new ground.”
Image courtesy of Robert J Sommer.
Shelley Wood was the Editor-in-Chief of TCTMD and the Editorial Director at the Cardiovascular Research Foundation (CRF) from October 2015…
Read Full BioSources
Snijder RJR, Luermans JGLM, de Heij AH, et al. Patent foramen ovale with atrial septal aneurysm is strongly associated with migraine with aura: a large observational study. J Am Heart Assoc. 2016;Epub ahead of print.
Disclosures
- Study authors report having no conflicts.
- Sommer disclosed research and education conflicts with both St. Jude Medical and Gore. AstraZeneca is funding the TRACTOR study.


Comments