September 2022 News Roundup
This month features a STEMI just after ICD placement, heat waves and heart failure, the fight against misinformation, and more.

Every month, Section Editor L.A. McKeown curates a roundup of recent news tidbits from journals and medical meetings around the globe.
Although disparities in acute MI care between urban and rural dwellers have narrowed over the last 18 years, patients presenting to hospitals in rural areas still have 15% higher adjusted in-hospital mortality and are less likely to be treated invasively than those in urban areas, according to a study published in Cardiovascular Revascularization Medicine.
Data on more than 70,000 TAVIs and surgical aortic valve replacements in aortic stenosis patients under age 60 indicate that the transcatheter treatment results in fewer procedural complications but similar short-term mortality. Reporting in Cardiovascular Revascularization Medicine, investigators say their analysis of the Nationwide Readmissions Database also suggests no significant difference between the two procedures in 30-day readmission rates.
 In an effort to combat misinformation about COVID-19 vaccines, the University of Chicago Pritzker School of Medicine has begun a course for first-year medical students on scientific communication and misinformation. “We hope that scientific communication becomes an explicit component of medical education, equipping trainees to reach broad populations, build trust with underserved communities, and combat misinformation to empower patients,” a group of trainees participating in the Chicago course write in a letter to the editor published in Academic Medicine.
In an effort to combat misinformation about COVID-19 vaccines, the University of Chicago Pritzker School of Medicine has begun a course for first-year medical students on scientific communication and misinformation. “We hope that scientific communication becomes an explicit component of medical education, equipping trainees to reach broad populations, build trust with underserved communities, and combat misinformation to empower patients,” a group of trainees participating in the Chicago course write in a letter to the editor published in Academic Medicine.
A survey of physicians, nurses, and others suggests that remote monitoring in cardiac rehab has taken off substantially since the start of the COVID-19 pandemic, with 65% of respondents saying they started using remote monitoring technology within the last 2 years. The most widely used devices cited by survey respondents were Holter monitors (42%), wearable ECG patches (40%), blood pressure monitors (45%), and ECG wrist monitors (42%).
In JACC: Case Reports, physicians from a New York hospital report an unusual case of an elderly woman who experienced acute STEMI shortly after receiving a biventricular implantable cardioverter-defibrillator (ICD). The patient underwent a hybrid procedure that involved unscrewing the LV lead and then performing emergent left heart catheterization, which showed a 100% distal occlusion of the second obtuse marginal artery. They conclude that mechanical obstruction of a coronary artery in this setting is rare and “has not been documented as a known complication of biventricular ICD placement.”
 A French study suggests that patients with heart failure are at risk for weight loss during heat waves, which may lead to hypotension and renal failure. In ESC Heart Failure, the researchers suggest that telemonitoring could help alert clinicians to weight loss and/or notify patients who are losing weight that it may be due to the heat and they should contact their healthcare provider about temporarily cutting back on their diuretics.
A French study suggests that patients with heart failure are at risk for weight loss during heat waves, which may lead to hypotension and renal failure. In ESC Heart Failure, the researchers suggest that telemonitoring could help alert clinicians to weight loss and/or notify patients who are losing weight that it may be due to the heat and they should contact their healthcare provider about temporarily cutting back on their diuretics.
Five-year follow up of the ISCHEMIA-CKD trial continues to show no difference in rates of cardiac death or all-cause death between patients randomized to an invasive versus conservative strategy for the management of chronic CAD in the setting of advanced chronic kidney disease. The findings were presented at ESC Congress 2022 and showed the risk of death in these patients to be close to 40% by 5 years.
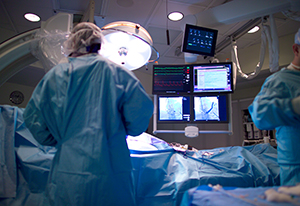 A state-of-the-art paper published in JACC: Cardiovascular Imaging reviews uses of intravascular imaging in daily CV cath lab practice as well as outcomes data supporting its use. The authors say that although adoption of intravascular imaging has been spotty in the United States, dedicated intravascular imagers could be a helpful addition in many labs to assist in performing the tests and interpreting the results.
A state-of-the-art paper published in JACC: Cardiovascular Imaging reviews uses of intravascular imaging in daily CV cath lab practice as well as outcomes data supporting its use. The authors say that although adoption of intravascular imaging has been spotty in the United States, dedicated intravascular imagers could be a helpful addition in many labs to assist in performing the tests and interpreting the results.
A study of ankle-brachial index (ABI) in hospitalized patients with acute coronary syndromes found a stepwise increase in adverse events and death in those with clinical and subclinical PAD versus those without PAD. Routine ABI in the hospital may enhance risk stratification and improve prognosis regardless of whether PAD symptoms are evident, the researchers conclude in Frontiers in Cardiovascular Medicine.
L.A. McKeown is a Senior Medical Journalist for TCTMD, the Section Editor of CV Team Forum, and Senior Medical…
Read Full Bio


Comments