Similar Rate of Radial Artery Occlusion After Manual and Mechanical Compression
One operator said the occlusion rate at 24 hours remains too high, suggesting more work is needed to reduce this complication after transradial access.
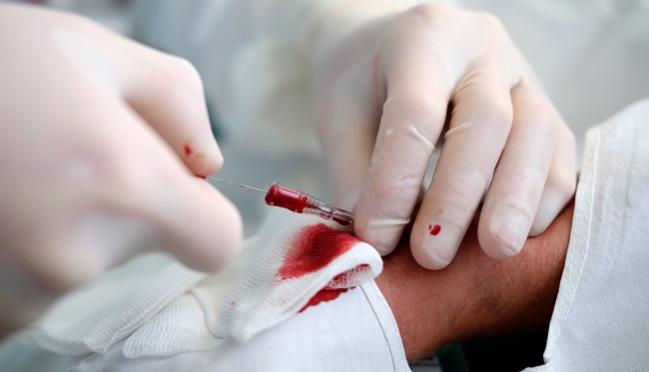
(UPDATED) For patients undergoing transradial coronary angiography, manual and mechanical compression of the puncture site result in similar rates of radial artery occlusion, although the time required for complete hemostasis is significantly shorter with manual compression, a new study shows.
Still, despite showing that manual compression was an “effective, safe, and less time-consuming method” to achieve hemostasis, lead investigator Dimitrios Petroglou, MD (Aristotle University of Thessaloniki, Greece), and colleagues say the results are likely to have limited applicability in clinical practice.
The manual compression protocol “will probably be driven by the need for larger involvement of postprocedural care team with repeated point-of-care evaluation of radial flow, making a rather simplistic and inexpensive process of hemostatic compression significantly more complex.”
Senior investigator Antonios Ziakas, MD (Artistotle University of Thessaloniki), told TCTMD the study took a lot of effort because it was difficult to convince five hospitals, including his own, to randomize patients to manual compression. Not only that, but the study required one or two individuals from each cath lab to perform manual compression so that the technique was standardized and consistent.
“You can imagine what would have happened if every day a different person, especially a different intern in cardiology, was doing manual compression for the study,” he said. “The difficult thing was to have someone doing this in five public hospitals in Greece, where there is no dedicated person for this.”
Mladen Vidovich, MD (University of Illinois Hospital and Health Sciences System, Chicago, IL), who wasn’t involved in the study, said the vast majority of US operators use mechanical compression devices, mainly because of the costs of labor associated with manual compression.
“If you were to do an economic subanalysis of this study—I don’t think they have the data—I would suspect manual compression is completely impractical,” he said. “I don’t know how I would implement this in my daily routine. Although it’s shorter, 20 minutes of nursing time is expensive.”
To TCTMD, Vidovich said the study shows manual compression is feasible, which is particularly important in some parts of the world where mechanical compression devices are prohibitively expensive. And while the manual approach is very effective, he said, “it all comes down to labor—that’s where the rubber hits the road.”
Also commenting on the study for TCTMD, Michael Savage, MD (Thomas Jefferson University Hospital, Philadelphia, PA), said radial artery occlusion is an important issue and the most common complication of transradial catheterization.
“Clinically this complication is often asymptomatic due to the collateral circulation and dual blood supply that perfuses the hand in most people,” he said in an email. “Nevertheless, symptomatic radial artery occlusion has been reported and may result in pain, paresthesias, and reduced function of the affected extremity. In addition, radial artery occlusion precludes use of the artery as an access site for future repeat catheterization procedures.”
The present study, however, is unlikely to change most operators’ clinical practice for a number of reasons, Savage added. Not only are the pneumatic bracelets used for mechanical compression relatively cheap—approximately $20—the study only looked at lower-risk patients undergoing diagnostic cath and treated with smaller 5-Fr catheters. This excludes patients treated with larger catheters and patients undergoing PCI, where more intensive anticoagulation is used.
Samir Pancholy, MD (The Commonwealth Medical College, Scranton, PA), one of the MEMORY investigators, told TCTMD that the study has important implications for cath labs outside the United States where manual compression is frequently used, particularly in developing countries that can’t afford the additional cost of mechanical compression. In those settings, labor is also significantly cheaper.
“Our problem in the US is that skilled labor is much more expensive than the band,” he said.
MEMORY: Shorter Hemostasis With Manual Pressure
The MEMORY study, which was published online June 4, 2018, in JACC: Cardiovascular Interventions, included 589 patients undergoing diagnostic coronary angiography via the radial artery with a 5-Fr sheath. With manual compression, pressure was applied to the puncture site for 10 minutes or longer to control bleeding (radial artery patency was checked every 1 to 2 minutes by transient manual compression of the ulnar artery and evaluated by plethysmography). With mechanical compression, an inflatable air-filled wrist bracelet (Vitatech Pressure Bandage, KDL Medical Group) was applied to the puncture site.
To TCTMD, Ziakas said they conducted the study because radial artery occlusion is one of the main complications of radial catheterizations, even though the problem is often not fully realized by radial operators. “Furthermore, in transfemoral angiography there are conflicting data comparing manual compression with closure devices and still some ‘femoralists’ consider manual compression better,” said Ziakas.
The incidence of radial artery occlusion at 24 hours—the study’s primary endpoint—was 12% in those treated with manual compression and 8% in those treated with mechanical compression (P = 0.176). In a logistic regression analysis, one adjusted for contrast volume used and heparin dose, the method of hemostasis was not associated with the risk of radial artery occlusion.
Several variables, including the number of arterial puncture attempts, activated clotting time, radiation time, and patency of flow in the radial artery during hemostasis, were all independent predictors of radial artery occlusion. Patent hemostasis, for example, was associated with a 92% lower risk of occlusion.
Mean hemostasis duration was significantly shorter with manual compression—22 minutes versus 119 minutes—but there was no difference in hematoma formation or hemorrhage at the access site, nor was there any significant difference in access-site complications.
Vidovich pointed out that the rate of radial artery occlusion at 24 hours, which was approximately 10% in both arms, is higher than would be expected.
“Radial artery occlusion is an issue, but I would almost say this study asks more questions than it answers,” Vidovich told TCTMD. “It’s a small study but they had high rates of radial artery occlusion, although it is at 24 hours. If you look at the data, the rate goes down over time. When you look at 7 days, 28 days, or 3 months, it wouldn’t look so bleak, but clearly, the early rate of radial artery occlusion is high.”
In the study, the researchers measured the diameter of radial artery, which was 2.8 mm at the distal end. “These are reasonably big radial arteries for small sheaths,” said Vidovich. “If you had an Asian population, you’d have much smaller arteries.” Patients with small radial arteries tend to be at a higher risk for radial artery occlusion, he noted.
Savage also noted the rate of radial arterial occlusion seemed high by current standards, but pointed out there was significant variability between centers, with occlusion ranging from 1% to 14%. “This raises the question as to the equivalency of techniques among the centers,” he said. “For example, one potential confounder was the lack of standardization for use of intra-arterial vasodilators.”
In the PROPHET-II study, the rate of radial artery occlusion at 24 hours was 4.3% with patent hemostasis alone and as low as 1% with patent hemostasis plus ulnar artery compression, he noted.
Pancholy, who led the PROPHET II study, said that while the rate of radial artery occlusion might be lower in randomized trials, 10% is closer to real-world practice. Although it is mostly asymptomatic, at a minimum the loss of the radial artery takes away an access site for future procedures, he noted.
“I think we tend to underplay it,” said Pancholy. “I often hear, ‘We just don’t see it that much.’ Well, we don’t see it because it’s asymptomatic for the most part. It’s not completely without consequence, but it’s just patients don’t feel the need to complain about it because the symptoms aren’t excruciating.”
Small Percentage of Pain or Paresthesia
In an editorial accompanying the study, Frederic Resnic, MD, and Arjun Majithia, MD (Lahey Hospital and Medical Center, Burlington, MA), said these new data highlight radial artery occlusion as an important complication, one that can be significantly underrecognized in clinical practice.
To reduce the risk of radial artery occlusion, Resnic and Majithia recommend adequate anticoagulation at the time of angiography, use of low-profile sheaths, avoiding repeat access of the radial artery, and following the Society for Cardiovascular Angiography and Intervention’s transradial working group’s recommendations to achieve patent hemostasis.
“We have to redouble our efforts to get [the rate of radial artery occlusion] lower,” added Vidovich. “What are we not doing right now? I don’t think it should be 10%.”
Ziakas agreed, telling TCTMD the interventional community needs to focus on lowering the rate. One of the main barriers at the moment is that operators assume radial artery occlusion doesn’t occur at their institution, or that the rate is very low. For this reason, people have expressed surprise the MEMORY study showed a rate as high as it did at 24 hours. “We definitely need real world data on radial artery occlusion,” said Ziakas.
Michael O’Riordan is the Managing Editor for TCTMD. He completed his undergraduate degrees at Queen’s University in Kingston, ON, and…
Read Full BioSources
Petroglou D, Didagelos M, Chalikias G, et al. Manual versus mechanical compression of the radial artery after transradial coronary angiography: the MEMORY multicenter, randomized trial. J Am Coll Cardiol Intv. 2018;11:1050-1058.
Resnic FS, Majithia A. Just the right pressure to optimize post-radial access care. J Am Coll Cardiol Intv. 2018;11:1059-1061
Disclosures
- The authors and editorialists report no relevant conflicts of interest.


Comments