Some Reassurances, Some Sobering Truths About Dialysis Needs After TAVR
New insights from the STS/ACC TVT Registry may help physicians give better numbers to patients grappling with what might happen post-TAVR, experts say.
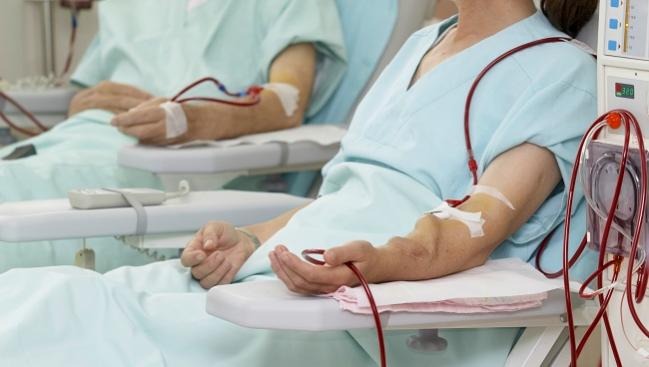
New research is adding fresh insights—and some reassurances—for physicians and patients concerned about the risks of dialysis following TAVR.
According to James W. Hansen, DO (Lahey Hospital and Medical Center, Burlington, MA), and colleagues, who dug into numbers captured in the Society of Thoracic Surgeons/American College of Cardiology (STS/ACC) TVT Registry, one in three patients with stage 4 chronic kidney disease (CKD, defined as glomerular filtration rate [GFR] of 15 to 29 mL/min/m2) will be dead within a year of undergoing TAVR. Approximately one in six of these stage 4 CKD patients will require dialysis.
Those numbers may not come as much of a surprise to interventional cardiologists and nephrologists, Hansen told TCTMD. Nor perhaps will the finding that TAVR patients with stage 5 CKD (GFR <15 mL/min/m2) faced even higher risks, with more than one in three requiring dialysis within the first 30-days postprocedure, rising to almost two in three by 1 year.
To physicians weighing the options for patients with severe aortic stenosis, the results should serve as a sober reminder that “ending up on renal replacement therapy may be an unacceptable outcome to some patients,” Hansen et al write in the October 23, 2017, issue of JACC: Cardiovascular Interventions.
But where the new data may be most useful is among patients with stage 3 CKD (GFR of 30 to 59 mL/min/m2).
All patients with CKD stages 3, 4, or 5 had a statistically higher likelihood of ending up on dialysis, both at 30 days and again at 1 year, Hansen told TCTMD. “But what I think is very compelling and actually very reassuring about this data is that people with CKD stage 3 had a relatively low rate of dialysis at 30 days and 1 year. It was statistically higher than the control group, but in terms of absolute risk it was not tremendously different.”
This should be somewhat reassuring, particularly to nephrologists and general practitioners, who might assume the risks to be higher. “For CKD stage 3 patients, their risk is real—it is not zero—but it was probably overestimated at least clinically,” Hansen said.
Dialysis: The Other ‘Hard’ Endpoint
Patients with severe renal insufficiency were typically excluded from the pivotal trials that helped establish TAVR as an alternative to surgery, or as the best option for nonsurgical patients. Indeed, severe renal disease is often a reason why patients are turned down for surgery and sent for transcatheter replacement instead.
As Hansen and colleagues write, however, while preprocedural GFR predicts acute kidney injury (AKI) after TAVR, and AKI itself increases the risk of death and rehospitalizations, risk calculators typically do not include specific GFR cut points to estimate the risk of renal replacement therapy after TAVR. Moreover, they write, the “true incidence” of this need after TAVR is unknown.
For their study, Hansen et al linked 4 years of data from the STS/ACC TVT Registry (2011-2014) to the Centers for Medicare & Medicaid Services database, looking specifically at renal replacement therapy or death postprocedure at 30 days and 1 year.
“The thing that really inspired this project,” Hansen said, “was actually a patient with CKD who was otherwise a great candidate for TAVR, who he came to us and informed my colleague that his nephrologist had said: ‘If you get a TAVR, you will end up on dialysis.’ And that got us thinking, well, how does he know that?”
Acute kidney injury has been relatively well studied after TAVR, Hansen continued, “but dialysis is an interesting endpoint because it’s a hard endpoint and it’s one that patients view with a certain caution. We’ve all had the patients that say: ‘I’d rather die than go on dialysis.’”
We’ve all had the patients that say: ‘I’d rather die than go on dialysis.’ James W. Hansen
To look into this question, Hansen and colleagues looked at rates of death and new dialysis according to preprocedure GFR, both as a continuous variable and according to CKD classifications based on GFR cut points. CKD stages 1 and 2, representing GFR rates of 60 mL/min/m2 or higher, were used as the control.
They found that risk of death and new dialysis were significantly increased with GFR less than 60 mL/min/m2 as compared with GFR above that level, but that the risk was particularly marked when GFR fell below 30 mL/min/m2.Moreover, for patients with GFR less than 60 mL/min/m2, a difference as small as 5 mL/min/m2 was associated with a measurable difference in rates of death, renal replacement therapy, or both at 30 days and 1 year.
Adjusted HR (95% CI) Based on Preprocedural GFR (mL/min/m2)
|
|
30-Day Mortality |
1-Year Mortality |
30-Day Renal Replacement Therapy |
1-Year Renal Replacement Therapy |
|
GFR 30-60 |
1.27 (1.11-1.45) |
1.27 (1.18-1.38) |
2.64 (2.02-3.43) |
2.41 (1.94-3.01) |
|
GFR 15-30 |
1.90 (1.48-2.44) |
1.75 (1.50-2.03) |
9.82 (7.16-13.47) |
9.34 (7.06-12.34) |
|
GFR < 15 |
1.14 (0.40-3.24) |
1.32 (0.71-2.45) |
36.66 (21.93-61.28) |
42.75 (29.01-62.98) |
“Dialysis is often an afterthought, as an outcome, but it is both clinically and personally important to the patient,” Hansen said. But the current numbers hint that at least in patients with a GFR higher than 30 mL/min/m2 that risk has previously been somewhat overestimated, he added. “This should be reassuring to cardiologists and nephrologists, and even the primary care physicians who are reluctant to refer their patients because of their kidney disease.”
A Role for Kidney-Sparing Strategies
Commenting on the study for TCTMD, Jonathan Byrne, MD (King's College Hospital, London, England), agreed that the findings are reassuring and in particular add to the information on dialysis, since much of the work conducted in the setting of renal dysfunction and TAVR has looked at creatinine rise and fall after TAVR, rather than the harder endpoint of renal replacement therapy.
“This does show some nice and interesting data, in particular on the rates of renal failure among the patients we see frequently for TAVR, with a GFR in the range of 30-59 mL/min/m2, and [in this group] we don’t have very high rates of renal replacement therapy,” Byrne said. “It’s reassuring that in the group we practice most of our medicine on, we don’t have a stratospherically high rates of renal replacement therapy.”
Byrne also noted that patients studied in the current paper were treated at a time when transapical procedures and other techniques were more common. It may be that rates of renal replacement therapy may drop still further using less invasive techniques, newer devices, smaller sheaths, less rapid pacing, less vascular injury, less sedation and contrast, etc. He added, however, that his “gut feeling” is that these advances will help patients with moderate CKD, but that the highest-risk patients “will always be high risk, no matter what we do.”
In an accompanying editorial, Israel M. Barbash, MD, and Amit Segev, MD (Tel Aviv University, Ramat Gan, Israel), point out that high-risk patients, those with GFR <30 mL/min/m2) represent “a small minority of the entire TAVR population, less than 6% of the patients.”
In this respect, they continue, “the manuscript by Hansen et al provides the physician invaluable information by identifying a small subgroup with an extremely high risk of [renal replacement therapy] or death. Physicians should be advised that patients with severely reduced GFR who experience additional comorbidities beyond chronic kidney disease may not benefit from TAVR because of high short- and long-term hazard. If a procedure is planned, these patients should be meticulously informed of the high risk for postprocedural renal replacement therapy and mortality.”
Both the editorialists and Byrne make the point that specific measures for reducing kidney injury in patients at high risk for dialysis should be considered including reducing or eliminating the use of contrast dye before and during the procedure, and optimizing hydration, potentially using emerging technologies designed to optimize flushing.
New Insights Into CKD, End-Stage Renal Disease, and TAVR
Also appearing in the same issue of JACC: Cardiovascular Interventions is a paper detailing the risk of in-hospital mortality and periprocedural outcomes, including AKI, among patients with CKD and end-stage renal disease undergoing TAVR. The study, led by Tanush Gupta, MD (Albert Einstein College of Medicine, Bronx, NY), is the second such paper in recent weeks to address TAVR outcomes in advanced kidney disease, relying again on data from the National Inpatient Sample. Not surprisingly, the paper reached very similar results to that of Mohananey et al, concluding that the proportion of patients with CKD or end-stage renal disease undergoing TAVR has increased in recent years, with in-hospital mortality decreasing slightly over this same period. AKI, however, particularly cases requiring new dialysis, was associated with a sevenfold increase in hospital-based mortality and has not declined with time.
Shelley Wood was the Editor-in-Chief of TCTMD and the Editorial Director at the Cardiovascular Research Foundation (CRF) from October 2015…
Read Full BioSources
Hansen JW, Foy A, Yadav P, et al. Death and dialysis after transcatheter aortic valve replacement. An analysis of the STS/ACC TVT Registry. J Am Coll Cardiol Intv. 2017;10:2064-2075.
Barbash IM, Segev A. The plan was to replace the valve, not the kidneys. J Am Coll Cardiol Intv. 2017;10:2076-2077.
Gupta T, Goel K, Kolte D, et al. Association of chronic kidney disease with in-hospital outcomes of transcatheter aortic valve replacement. J Am Coll Cardiol Intv. 2017;10:2076-2077.
Disclosures
- Segev reports serving on the advisory board for Medtronic.


Comments