Vasopressor/Steroid Combo Jump-starts Circulation for In-Hospital Cardiac Arrests
Despite this boost, however, mortality and neurological function were unaffected in the randomized VAM-IHCA trial.
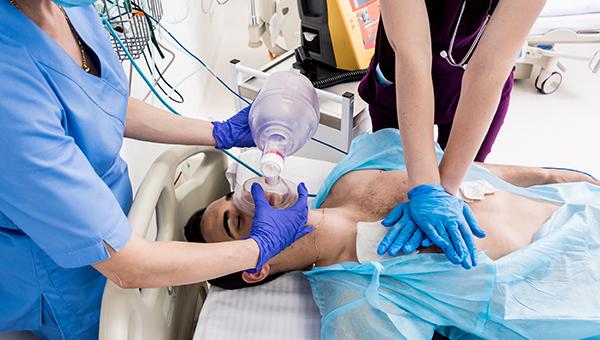
For patients with in-hospital cardiac arrest (IHCA), adding a vasopressor and steroid shortly after epinephrine improves return of spontaneous circulation (ROSC), according to the randomized VAM-IHCA trial.
Yet unlike smaller studies that have come before, the latest failed to show any reduction in mortality or gain in neurological function with vasopressin/methylprednisolone. Its results were published Wednesday in JAMA.
“On one hand, I was surprised that there was an improvement in return of spontaneous circulation but no sign of a benefit in survival or favorable neurologic outcome. I had thought that all outcomes would have shown no difference or a difference in the same direction,” lead author Lars W. Andersen, MD, PhD (Aarhus University Hospital, Denmark), told TCTMD in an email. That said, it’s not uncommon for drugs in cardiac arrest to improve ROSC while having a smaller effect on long-term outcomes, he added.
The reason why this ROSC benefit didn’t translate into better mortality is “the million-dollar question,” one for which he doesn’t know the answer, said Andersen.
Back in 2009 and 2013, two randomized trials led by Spyros D. Mentzelopoulos, MD, PhD (National and Kapodistrian University of Athens Medical School, Greece), showed promise for these medications. But with a combined total of 368 patients in the studies and lack of later confirmation, the strategy hasn’t been adopted by US and European cardiac arrest guidelines.
Niklas Nielsen, MD, PhD (Helsingborg Hospital, Sweden), who didn’t take part in any of the aforementioned research, commented to TCTMD that vasopressin/methylprednisolone “is definitely a combination that’s worth looking into.” Some are already using this strategy, either systematically or as a rescue, he added, but there aren’t definitive numbers on how commonplace it is.
Indeed, less is known about IHCA in general compared with out-of-hospital cardiac arrest, Nielsen said. Part of the issue, he suggested, is that IHCA “is a little bit of a forgotten disease,” perhaps because it’s more heterogeneous and spans across specialties depending on where in the hospital it occurs.
VAM-IHCA
For VAM-IHCA, Andersen et al analyzed results for 501 patients (mean age 71 years; 64% men) with IHCA at 10 Danish hospitals between October 15, 2017, and January 21, 2021. Study participants were randomized to placebo or to vasopressin (20 IU)/methylprednisolone (40 mg) after their first dose of epinephrine, to be followed by up to four additional doses of the study drug/placebo after each epinephrine administration.
Two-thirds of the patients had experienced IHCA while receiving care in standard medical or surgical units, and 90% presented with an initial shockable rhythm. After cardiac arrest, it took a median of 5 minutes to deliver epinephrine and 8 minutes to administer the study drug.
ROSC, the study’s primary endpoint, was achieved in 42% of the group receiving vasopressin/methylprednisolone and 33% of controls (P = 0.03) at a median of 16 and 18 minutes, respectively. By 30 days, survival was statistically similar between the two study arms but numerically higher with placebo (12.0% vs 9.7%; P = 0.48), while the rate of favorable neurological outcome, defined as a Cerebral Performance Category score of 1 or 2, was 7.6% in both groups.
Among patients with ROSC, adverse events included hyperglycemia (77% with the drug combo vs 73% with placebo) and hypernatremia (28% vs 31%, respectively).
To TCTMD, Andersen elaborated on potential reasons why more ROSC didn’t equal higher survival and better neurological outcome.
“The goal of the intervention is to restart the heart. The drugs are not neuroprotective,” he explained. “It is possible that the intervention restarts the heart on patients that have irreversible neurological damage and therefore die later on. Another potential explanation is that the intervention does have an effect on long-term outcomes, but we were not able to detect it in the current trial.” Andersen stressed that VAM-IHCA wasn’t powered for these 30-day outcomes.
“Based on the current evidence, I would not recommend for or against the use of the combination for in-hospital cardiac arrest,” he advised.
What to Make of the Data?
Presenting their published data virtually on the website Critical Care Reviews, the researchers also shared results from an individual-patient-data meta-analysis combining VAM-IHCA with the two Mentzelopoulos trials, for a total of 869 patients.
Still, this effort arrived at largely the same conclusions as the main paper. The effect on ROSC diminished over time across the studies, with odds ratios of 7.84, 3.19, and 1.65, to arrive at 2.09 (95% CI 1.54-2.84) in the combined cohort. At hospital discharge, both survival and neurological function were similar in the intervention and placebo groups.
Additionally, for ROSC, the combined data set showed a trend favoring vasopressin/methylprednisolone when the time to study drug was within versus exceeding 6 minutes (P = 0.10).
“If you pool them together, it seems extremely clear that this drug combination increases the return of spontaneous circulation,” Nielsen noted. “When it comes to the more-important outcomes”—survival and neurological function—“it looks like there is a trend toward benefit, but that was not statistically significant.”
Regardless, ROSC “might in itself be a relevant outcome, because it’s the first step towards good future outcome. If you don’t get return of spontaneous circulation, you will certainly die. But if you [do get it], then the medical community may have the possibility to save your brain and body function,” he observed.
Mentzelopoulos, speaking during the online broadcast, drew attention to several differences between his studies and VAM-IHCA. Among them were use of hydrocortisone to address postresuscitation shock in the former and a longer delay to study drug in the latter.
What the new trial suggests is that “there is a quite narrow temporal window for a meaningful use of vasopressor administration in combination with steroids. And I think that to achieve the best result during CPR, these drugs should be administered as soon as possible,” said Mentzelopoulos, who called for larger studies on the topic.
Andersen agreed. “We need a larger trial powered for patient-centered long-term outcomes. Some trials are in the planning phase, but it is unclear whether they will give us the answer,” he told TCTMD.
An editorial in JAMA by Jason Haukoos, MD (Denver Health and the University of Colorado School of Medicine), and colleagues also reaches the conclusion that additional research is needed, specifically trials powered for survival with good neurological function. “Until then, the use of vasopressin and steroids for patients with in-hospital cardiac arrest is not ready for usual care but may be considered when patients remain unresponsive to more-conventional treatments,” they write.
Caitlin E. Cox is Executive Editor of TCTMD and Associate Director, Editorial Content at the Cardiovascular Research Foundation. She produces the…
Read Full BioSources
Andersen LW, Isbye D, Kjærgaard J, et al. Effect of vasopressin and methylprednisolone vs placebo on return of spontaneous circulation in patients with in-hospital cardiac arrest: a randomized clinical trial. JAMA. 2021;Epub ahead of print.
Haukoos H, Douglas IS, Sasson C. Vasopressin and steroids as adjunctive treatment for in-hospital cardiac arrest. JAMA. 2021;Epub ahead of print.
Disclosures
- Andersen reports receiving grants from Aarhus University Research Foundation, the Department of Clinical Medicine at Aarhus University, and Independent Research Fund Denmark, as well as nonfinancial support from Amomed Pharma GmbH, which provided trial drug during the conduct of the study.
- Nielsen reports no relevant conflicts of interest.
- Haukoos is supported, in part, by grants from the National Institute on Drug Abuse, the Centers for Disease Control and Prevention, the National Heart, Lung, and Blood Institute, and the Department of Defense.



Comments