Very Low LDL Levels Best in Secondary Prevention: Ez-PAVE
The trial findings complement the updated US dyslipidemia guidelines that promote early and intensive LDL lowering.
NEW ORLEANS, LA—Lowering LDL cholesterol to less than 55 mg/dL reduces the risk of major cardiovascular events in patients with atherosclerotic cardiovascular disease (ASCVD) better than does a higher target of less than 70 mg/dL, according to new randomized data.
Among more than 3,000 patients in South Korea enrolled in the Ez-PAVE trial, those randomized to the intensive target had a 33% lower 3-year risk of cardiovascular death, nonfatal MI, nonfatal stroke, any revascularization, or hospitalization for unstable angina compared with those assigned to the more conventional threshold.
“These findings provide the randomized evidence for more intensively lowering LDL strategy for secondary prevention consistent with the current guideline recommendations,” said Byeong‑Keuk Kim, MD (Yonsei University College of Medicine, Seoul, Republic of Korea), who presented the findings today in a late breaking session at the American College of Cardiology 2026 Scientific Sessions.
The results, which were simultaneously published in the New England Journal of Medicine with first author Yong‑Joon Lee, MD (Yonsei University College of Medicine), complement the recently released American dyslipidemia guidelines, which recommend targeting LDL lower and earlier.
Karen Aspry, MD (Brown University Health, East Greenwich, RI), who discussed the findings during a media briefing, called Ez-PAVE an example of a “real-world approach to how clinicians should be titrating to a lower target using ezetimibe, which many are not doing.” Using this drug over PCSK9 inhibitors is also more cost-effective, she pointed out. “As much as we do like them and use them, we have to always think about cost.”
That said, the results of Ez-PAVE “are not that surprising given that we know from IMPROVE-IT and also some observational data from Europe showing that dual oral therapy post-ACS targeting LDL down to 55 achieves better outcomes,” Aspry added. Also, the fact that unstable angina was included in the primary endpoint is a strength of the study, given that women tend to present with unstable angina more so than nonfatal MI.
IMPROVE-IT investigator Christopher Cannon, MD (Brigham and Women’s Hospital, Boston, MA), told TCTMD that Ez-PAVE is an example of yet another study promoting “the same message” that dropping LDL leads to fewer events. “It’s nice to see that, once again, the benefits of lowering LDL cholesterol,” he said. “This is really saying that 55 is our new goal and we need to really embrace that and work hard to get patients to that goal.”
Further, Cannon said, having “fresh data” on the heels of the new American dyslipidemia guidelines “will hopefully help with implementation of [them].”
Ez-PAVE Results
Ez-PAVE included 3,048 patients with known ASCVD (mean age 64.4 years; 20.9% women) randomized to two LDL-cholesterol targets: less than 55 mg/dL or 70 mg/dL between 2021 and 2022 at 17 South Korean sites.
Those randomized to the less than 55 mg/dL target were allocated to treatment with a statin alone or statin plus ezetimibe. In the less than 70-mg/dL group, patients were also allocated to treatment with a statin alone or statin therapy plus ezetimibe. Combination therapy with ezetimibe used rosuvastatin, while rosuvastatin or atorvastatin were the agents used in monotherapy. This ensured that patients randomized to the two LDL targets were evenly treated with the different lipid-lowering strategies, although medication adjustments were encouraged over time to make sure patients were meeting goals.
Notably, uptitrating statin dosages and adding ezetimibe were recommended before introducing PCSK9 inhibitors. The baseline median LDL cholesterol was 76 mg/dL.
Over a median follow-up period of 3 years, LDL cholesterol was reduced to 56 mg/dL in the intensive-target group and 66 mg/dL in the less intensive-target cohort. Use of ezetimibe, high-intensity statins, and PCSK9 inhibitors were all higher among patients randomized to the lower LDL threshold at 1 month as well as 1, 2, and, 3 year follow-up. Overall, 3.6% of patients in the study stopped LDL-lowering therapy or lowered their dose despite not meeting goals, primarily due to experiencing adverse events.
By 1 month, 31.2% and 59.4% of patients in the intensive- and less-intensive targets, respectively, had reached their assigned LDL target. These rates increased to 42.9% and 67.2% at 1 year, 53.3% and 67.7% at 2 years, and 60.8% and 68.1% at 3 years.
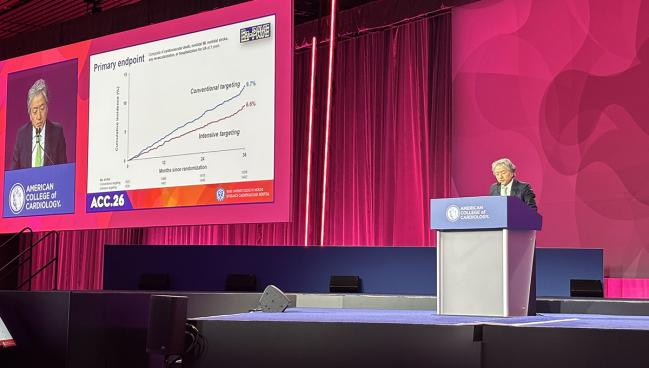
The rate of primary endpoint events was significantly lower for those trying to achieve the stricter versus conventional LDL target (6.6% vs 9.7%; HR 0.67; 95% CI 0.52-0.86). Rates of both nonfatal MI (0.8% vs 1.7%; HR 0.46; 95% CI 0.23-0.91) and any revascularization (4.8% vs 7.5%; HR 0.63; 95% CI 0.47-0.84) were significantly lower with 55 mg/dL compared with 70 mg/dL.
Results were similar in all subgroup and sensitivity analyses except there was no benefit to intensive LDL lowering for the primary endpoint in women (7.0% vs 5.7%; HR 1.22; 95% CI 0.66-2.28), whereas there was an advantage in men (6.5% vs 10.8%; HR 0.59; 95% CI 0.45-0.79).
This was likely due to the study being underpowered for women, Kim told TCTMD. However, he pointed out that maintenance of lipid-lowering therapy differs between men and women, adding that his team plans to study this further in the future.
Looking at safety, there were no differences between the groups in the incidence of new-onset diabetes, worsening glycemic control, statin-associated muscle symptoms leading to changes in therapy dose or regimen, cancer diagnosis, cataract surgery, elevation of the aminotransferase level, and elevation of the creatine kinase level. Notably, though, patients assigned to the more versus less intensive LDL target had a lower incidence of elevation of creatinine (1.2% vs. 2.7%; P = 0.004).
‘Robust, Clear’ Findings
“It’s a moderate sized trial and I think . . . the treatment effect is bigger than one might have expected,” Cannon commented. “But it’s robust, clear, [and] there’s nothing ambiguous about the findings. The curves separate early [and] they’re steady.”
In clinical practice, getting patients to an LDL of 55 rather than 70 mg/dL involves a “newer conversation,” Cannon said. “To get less than 55, it will often take more than just high-dose statins and ezetimibe. About a third of people would need a PCSK9, and it may be even a bit higher than that if you add in some statin tolerance.”
Adding an injectable drug could be a big ask particularly for lower-risk patients, although the increasing prevalence of GLP-1 receptor agonists is likely lowering the barrier to these kinds of treatments for many, according to Cannon. “That’s spilling over to cholesterol that people say: ‘Oh yeah, I take Wegovy. No problem. I’ll take the PCSK9s.’ So that is getting a little easier.”
In an accompanying editorial, Jeffrey L. Probstfield, MD, and Kelley R.H. Branch, MD (both University of Washington School of Medicine, Seattle), write that the mechanism of benefit observed in the trial “is not entirely clear.” It’s possible that the South Asian population studied might be more apt to benefit from reaching lower LDL levels, they say, but also high adherence and the benefits of combination therapy might have played roles.
“We have little data on how risk reduction may differ in a South Asian population as compared with other populations, but the current trial suggests that the benefit for South Asian patients with atherosclerotic cardiovascular disease is the same as or greater than that in other populations,” the editorialists write. “Whether the findings from the current trial can be extrapolated to other, non-South Asian populations requires additional study.”
While Ez-PAVE was the first trial of its kind in a South Asian population, Cannon said he’s not worried about generalizability. “It’s so consistent with every other trial ever done in lipid lowering in whatever population,” he commented.
Additionally, Cannon made “nothing” of the sex differences observed in the subgroup analysis, as it was not powered to look at this. “Every analysis of lipid lowering shows that it’s the same in men and women,” he said.
The data don’t make clear whether primary prevention patients should also be targeting LDL cholesterol levels below 70 mg/dL, according to Probstfield and Branch.
“The Ez-PAVE trial firms the foundation of lipid guidelines in secondary prevention and potentially paves the way for more definitive trials to evaluate targeted LDL cholesterol levels in other populations, with other treatment combinations, and with other LDL cholesterol goals for primary prevention,” they conclude.
Yael L. Maxwell is Senior Medical Journalist for TCTMD and Section Editor of TCTMD's Fellows Forum. She served as the inaugural…
Read Full BioSources
Lee Y-J, Lee S-J, Kim JW, et al. Intensive LDL cholesterol targeting in atherosclerotic cardiovascular disease. N Engl J Med. 2026;Epub ahead of print.
Probstfield JL, Branch KRH. Paving the road toward targeted lipid lowering. N Engl J Med. 2026;Epub ahead of print.
Disclosures
- The Ez-PAVE trial was funded by an investigator-initiated grant from the Cardiovascular Research Center (Seoul, South Korea) under a contract with Yuhan Corporation (Seoul, South Korea).
- Kim reports receiving grants and research support from Abbott Vascular, Biotronik, Boston Scientific, CGBIO, ChongKunDang, Daewoong Pharmaceutical, Genoss, Medtronic, MicroPort, Sam Jin Pharmaceutical, and Yuhan Corporation and honoraria or consultation fees from Amgen, AstraZeneca, DIO Medical, Hanmi, and Novartis.
- Branch reports receiving grants from and serving as a consultant to Bayer, Amgen, Novartis, and Kestra and serving as a consultant to Nanox.
- Probstfield reports no relevant conflicts of interest.
- Canon reports receiving research grants from Amgen, Better Therapeutics, Boehringer-Ingelheim, Novo Nordisk; salary support from Colorado Prevention Center Clinical Research, which gets research grant support from Amgen, Bayer, Cleerly, Esperion, Lexicon, and Silence; consulting fees from Amryt/Chiesi, Amgen, Applied Therapeutics, Boehringer-Ingelheim, BMS, CSL Behring, Genomadix, Lilly, Janssen, Milestone, Novartis, Pfizer, Rhoshan, and Tremeau; and serving on data and safety monitoring boards for Areteia, Cortera, Novartis, Novo Nordisk, ROMTherapy, and the Veterans Administration.





Comments