Women’s Risk for CVD Seen at Lower BP Thresholds Than Men
The data suggest a need to reassess optimal sex-specific systolic ranges and their relationship to treatment goals.
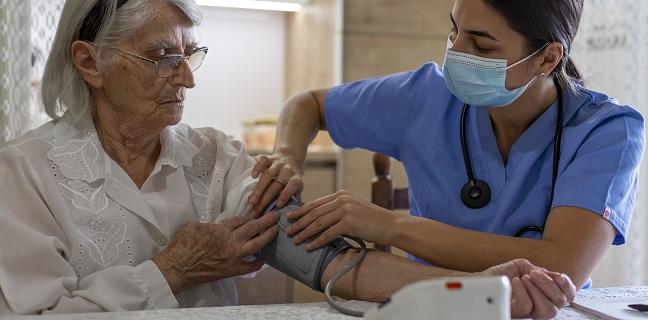
Compared with men, women have a lower range of optimal blood pressure and are therefore at higher risk for CV disease and events at systolic levels typically believed to be “normal,” new research concludes.
“We've been assuming up to this time that 120 is the number to worry about, and anything under 120 is totally fine and safe for both women and men,” said senior author Susan Cheng, MD (Cedars-Sinai Medical Center, Los Angeles, CA). “It turns out it's probably fine and safe for men, but not necessarily for women.”
In an analysis of participants from four large community-based cohorts, Cheng’s group found that women who had CV disease, stroke, MI, or heart failure (HF) consistently had BP levels that were 10 mm Hg lower to as much as 50 mm Hg lower than men who experienced the same events.
The study builds on previous work by Cheng and colleagues demonstrating through serial blood-pressure measurements taken over decades that hypertension begins years earlier in women than men.
“I think at this point, we really can't ignore it,” Cheng told TCTMD. “Male and female anatomy and physiology is different, and that's probably why things look different as risk factors accumulate over the life course and the manifestations of cardiovascular disease end up being different in males and females as they age.”
Important Considerations for MI Risk
Published in Circulation and led by Hongwei Ji, MD (Affiliated Hospital of Qingdao University, China), the analysis included 27,542 men and women from the Framingham Heart Study, the Multi-Ethnic Study of Atherosclerosis (MESA), the Atherosclerosis Risk in Communities (ARIC) study, and the Coronary Artery Risk Development in Young Adults (CARDIA) study.
We've been assuming up to this time that 120 is the number to worry about, and anything under 120 is totally fine and safe for both women and men. It turns out it's probably fine and safe for men, but not necessarily for women. Susan Cheng
Over a mean length of 28 years, 44% of women developed nonfatal or fatal CV disease including MI, HF, or stroke. Multivariable analyses found that having systolic BP of 100-109 mm Hg relative to systolic BP of < 100 mm Hg was associated with incident CVD in women, while for men the risk was associated with a higher systolic BP of 130-139 mm Hg.
For MI, women saw risk at a systolic BP of 110-119 mm Hg, while the risk for men was not apparent until systolic BP of 160 mm Hg or higher. HF risk was associated with systolic BP ranges of 110-119 mm Hg in women and 120-129 mm Hg in men. Likewise, stroke risk systolic thresholds were 120-129 mm Hg in women and 140-149 mm Hg in men.
Once they got to systolic BP levels of 160 mm Hg or higher, women had higher hazard ratios than men for CV disease (HR 3.50 vs 2.02), MI (HR 3.67 vs 1.62), HF (HR 3.37 vs 2.74), and stroke (HR 3.56 vs 2.32).
Analyses of interactions by age found that the association between systolic BP and CV disease risk was more pronounced in younger versus older women (median age < 52 vs ≥ 52 years). No age interaction was seen in men.
Cheng said while the findings will need further validation, the combination of the earlier work showing lower hypertension thresholds for women than men, coupled with the new data linking those lower thresholds to outcomes, points toward a need to fully understand what the optimal healthy systolic range is for women. She added that the MI data in particular should send the message to women that the risk of an MI due to high blood pressure is just as important and relevant as the risk of stroke.
“If the average blood pressure is really hanging out above 110 for women and above 120 for men, there is a real measurable and statistically significant risk for myocardial infarction,” Cheng noted. “We've known that all along. But until we had the chance to sit down and look very carefully and rigorously at these data, at least for me personally, it wasn't as profound or obvious a truth.”
According to Cheng, research into sex-specific differences in BP is only just beginning, with much more work needed on understanding treatment goals for women separate from men, which starts with understanding their lower systolic BP thresholds and how those change as they age.
“People do become more heterogeneous in their risk profiles, in their comorbidities, and in the medications they're taking as they age,” she said. “We need to get better at personalizing and tailoring and optimizing blood pressure care around each individual.”
L.A. McKeown is a Senior Medical Journalist for TCTMD, the Section Editor of CV Team Forum, and Senior Medical…
Read Full BioSources
Niiranen Ji H, TJ, Rader F, et al. Sex differences in blood pressure associations with cardiovascular outcomes. Circulation. 2021;143:761-763.
Disclosures
- Ji and Cheng report no relevant conflicts of interest.



Comments