AHA Details Accurate BP Measurement in Updated Scientific Statement
“We wouldn’t accept laboratory values that weren’t accurate, so why should we accept these exam measurements not being accurate?” an author asks.
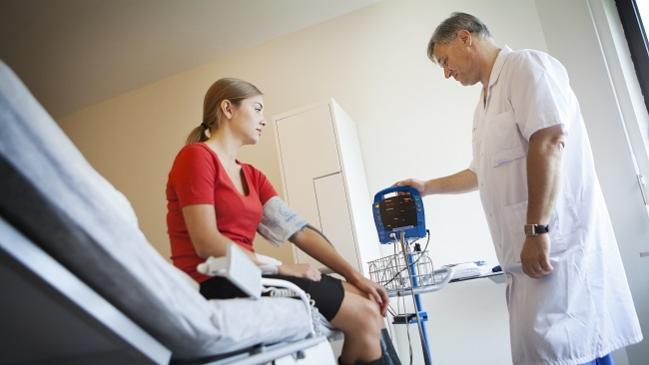
Clinicians have a new resource to turn to when it comes to accurately measuring blood pressure in the form of an updated scientific statement from the American Heart Association (AHA).
A lot has changed since the last statement was published in 2005, with more evidence supporting use of oscillometric devices—versus auscultatory methods—to measure BP, mounting data on the importance of masked hypertension and its relationship with increased cardiovascular risk, and the growth of home BP monitoring.
Paul Muntner, PhD (University of Alabama at Birmingham), chair of group that wrote the updated statement, which was published online today ahead of print in Hypertension, put the importance of accurate BP measurement in a broad context.
“The rates of heart disease and stroke have been declining in the US over the past 40 years, and a lot of that has been due to better control of blood pressure,” he told TCTMD. “However, hypertension is still very common and still accounts for a large proportion of heart disease and stroke in the US, and for us to reduce rates of heart disease and stroke even further, I think it’s important to accurately measure blood pressure so that treatments can be given to the people who will benefit most.”
In the latest comprehensive hypertension guideline released in 2017, the AHA, the American College of Cardiology, and nine partnering organizations lowered the bar for a hypertension diagnosis, such that 46% of US adults are now considered hypertensive. Correct measurement of BP is seen as critical to the diagnosis and management of the condition, but in practice, the quality of BP readings varies widely.
This new statement, which goes into more detail about measuring BP than did the guideline, provides the information needed to ensure the best readings. “The accurate measurement of blood pressure is important and we wouldn’t accept laboratory values that weren’t accurate, so why should we accept these exam measurements not being accurate?” Muntner said. “Therefore, there’s a need to recognize the importance of training and retraining to measure blood pressure and using devices that are accurate.”
One of the major changes over the past 15 years, Muntner said, is the accumulation of data supporting use of oscillometric devices, which don’t require as much training as the auscultatory approach, for measuring BP in the office. In particular, automated devices simply the process by having a preset waiting period of 3 to 5 minutes before the cuff inflates, by taking multiple measurements that can be averaged, and by allowing office staff members to leave the patient resting quietly, the ideal situation for assessing BP. They also reduce the possibility of human errors.
The statement highlights key points for accurate office measurement, including selection of appropriate cuff sizing and placement, proper patient positioning, number of measurements at a visit, and frequency of BP measurement.
But there can be significant differences between BP measured in the office and that measured elsewhere, and the authors also provide an extensive overview of out-of-office techniques, such as ambulatory BP monitoring (ABPM) and home monitoring.
ABPM, which is preferred over home monitoring, can identify various BP patterns, including white coat and masked hypertension. The latter phenomenon, in which BP is normal in the office but raised outside the clinic, was just being uncovered at the time of the last scientific statement on measuring BP. New data have shown that it is associated with a doubling in the risk of heart disease or stroke.
When ABPM is not an option, either because it’s not available or the patient won’t tolerate it, home BP monitoring can be an alternative. This can also be used to detect white coat or masked hypertension and, like ABPM, can be used to monitor antihypertensive drug efficacy in treated patients.
The biggest challenge regarding home BP monitoring is that many commercially available devices have not been validated, and it’s important that patients are educated about the need to buy devices that have been shown to be accurate and can automatically store BP readings for later review by their physician, Muntner said.
The authors of the statement note that in addition to main ways to assess BP, there are a variety of newer techniques that have been developed in recent years. They mention finger cuffs, wrist monitors, ultrasonography techniques, tonometry, smartphone technology, wearable sensors, and cuffless BP monitors.
Muntner again stressed the importance of verifying that any modality used to measure BP has been shown to be valid, pointing out that “there just needs to be awareness that some of the mobile health blood pressure monitors aren’t accurate.” Some of the wrist monitors have been validated, he added. “I think it’s just important to make sure that people measure their blood pressure correctly when using them.”
Another exciting area, Muntner said, is having pharmacists measure BP or having patients measure their own BP using kiosks that can be found in grocery stores, health clubs, and other places. That “just provides another opportunity for patients to take control of their health and monitor their blood pressure,” he said.
The scientific statement closes with sections discussing BP measurement in specific populations, BP variability, and protocols for validation of BP monitors and device calibration.
Correction: An earlier version of this story misquoted Dr. Muntner.
Todd Neale is the Associate News Editor for TCTMD and a Senior Medical Journalist. He got his start in journalism at …
Read Full BioSources
Muntner P, Shimbo D, Carey RM, et al. Measurement of blood pressure in humans: a scientific statement from the American Heart Association. Hypertension. 2019;Epub ahead of print.
Disclosures
- Muntner reports no relevant conflicts of interest.


Comments