Breast Calcifications May Hold Important Clues for CV Risk Stratification
Included in a special “Go Red for Women” issue of Circulation are several papers emphasizing collaboration between cardiologists and oncologists.
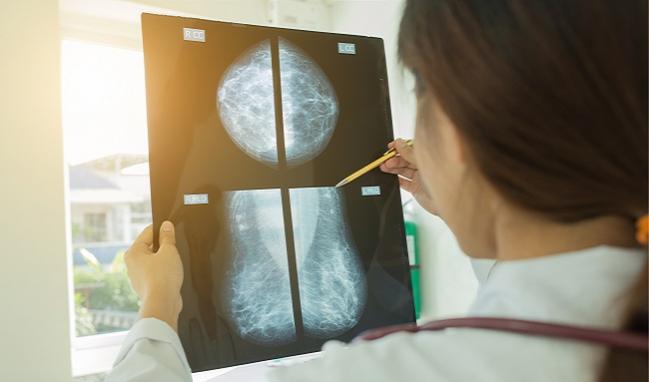
Improved understanding about the significance of calcified arteries detected on mammograms and more collaborative efforts between oncologists and cardiologists are two ongoing areas of research that may help change women’s healthcare for the better. In two new reports that appear as State of the Art papers in a special “Go Red for Women” issue of Circulation, published February 19, 2019, researchers outline the importance of each.
In one report, Quan M. Bui, MD, and Lori B. Daniels, MD (both University of California, San Diego), review what is known about breast arterial calcification (BAC) found on mammograms and its potential role as a risk factor for cardiovascular disease. In their paper, the researchers say a recent meta-analysis indicates that more than 12% of women undergoing breast cancer screening have some degree of BAC. Factors associated with a higher likelihood of calcification in the breast include age, diabetes, number of live births, chronic kidney disease, and personal history of CAD or CAD risk equivalents.
According to Bui and Daniels, the presence of BAC in at least one breast may increase the risk of developing CAD and dying from cardiovascular disease. It also has been associated with heart failure risk and is thought to be an early marker of vascular stiffness and endothelial dysfunction. Research also suggests that BAC is strongly associated with coronary artery calcium (CAC) and may be related to risk of subclinical CAD in asymptomatic women. Like calcium in the breast, CAC was considered an incidental finding on imaging until it was studied in depth and a scoring method for it was developed.
“Given the strength of the association between BAC and CVD, we propose that radiologists should begin universally reporting the presence of BAC on all mammograms as an important next step forward,” Bui and Daniels write. “Furthermore, we suggest that the reports include a statement in fine print noting the association of BAC with CAC and that its significance depends on the overall cardiovascular risk profile and clinical correlation. This would be similar to the verbiage in use today for incidental findings on other diagnostic studies (ie, pulmonary nodules on CAC studies).”
Although reporting BAC is not currently standard practice, it should be “relatively easy for radiologists to identify and report,” Bui told TCTMD in an email.
Mammography has the potential to alter the course of the two leading causes of death in women, breast cancer and heart disease, through comprehensive counseling on shared modifiable risk factors. Quan M. Bui
“At this time, there are no clinical practice recommendations that include BAC assessment due to a lack of prospective studies,” he added. “Retrospective studies suggest an association between BAC and cardiovascular disease, but formal recommendations would be premature.”
Another reason to encourage reporting of BAC and communicating the significance of it with patients, he said, is that it provides evidence of a risk that can be readily seen.
“We believe that there is truth to the sentiment that ‘a picture is worth a thousand words’ and that seeing calcifications in the breast arteries may empower patients to participate in their medical care,” Bui observed. “Mammography has the potential to alter the course of the two leading causes of death in women, breast cancer and heart disease, through comprehensive counseling on shared modifiable risk factors.”
Better Collaboration Urged Once Again
For women with a diagnosis of breast cancer, co-management of cardiovascular risks by oncologists and cardiologists is another area of much ongoing research. Increasing awareness of how to manage preexisting or emergent cardiovascular disease in women with breast cancer is "an active work in progress," noted Ana Barac, MD, PhD (MedStar Heart and Vascular Institute/MedStar Washington Hospital Center, DC), senior author of another report, in an interview with TCTMD.
Barac, who is chair of the American College of Cardiology’s (ACC) cardio-oncology section, said one area of focus currently is in providing education and resources to be used in fellowship training for both oncologists and cardiologists. In their paper, Barac and colleagues—led by Rachel Barish, MSN (MedStar Georgetown University Hospital Physicians Group, Washington, DC)—outline the cardiovascular concerns associated with contemporary, multimodality breast cancer treatment and address clinical questions such as which breast cancer patients are at increased risk for cardiac dysfunction and which preventive strategies minimize risk before and during initiation of cardiotoxic breast cancer therapy. They also discuss surveillance and monitoring approaches for cardiac dysfunction during and after chemotherapy.
To TCTMD, Barac said better survival of patients with breast cancer has afforded “the luxury of discussing late effects” of treatment and has hastened the need to fill research gaps related to bringing cardiovascular care to this population. While funding has been a problem in the past, she noted that the National Cancer Institute and the National Heart, Lung, and Blood Institute have issued joint program announcements for cardiotoxicity research. Additionally, the ACC will launch a new journal dedicated to cardio-oncology research later this year, Barac said.
Encouraging cardiologists and oncologists to partner early is another important piece of the puzzle, she observed.
“It’s time for a paradigm change,” Barac said. “Right now, we exist in two different worlds.” She added that the new report published in Circulation this week is an effort to bridge learning between the two specialties by including information and references that should be helpful to both.
L.A. McKeown is a Senior Medical Journalist for TCTMD, the Section Editor of CV Team Forum, and Senior Medical…
Read Full BioSources
Bui QM, Daniels LB. A review of the role of breast arterial calcification for cardiovascular risk stratification in women. Circulation. 2019;139:1094-1101.
Barish R, Lynce F, Unger K, Barac A. Management of cardiovascular disease in women with breast cancer. Circulation. 2019;139:1110-1120.
Disclosures
- Bui and Barish report no relevant conflicts of interest.


Comments