COVID-19 Patients With Arterial Leg Thromboses Risk Amputation and Death
A small study of patients treated early in the pandemic shows poor outcomes when leg symptoms are involved.
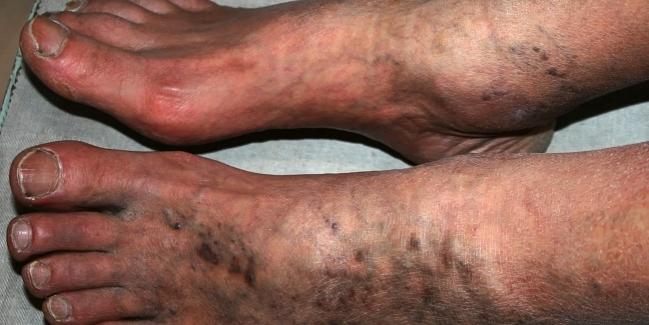
Some patients with COVID-19 develop symptomatic arterial thrombosis in their legs that is difficult to eradicate by usual means and portends worse outcomes, new data show.
The small study of COVID-19 patients treated in New York City in March and April 2020 corroborates accumulating evidence of unusual thrombotic activity and varied presentation among patients infected with the virus.
Speaking with TCTMD, Inessa A. Goldman, MD (Montefiore Medical Center, Bronx, NY), said early in the pandemic she began noticing patients presenting with extensive lower-extremity thrombosis on an order of magnitude much greater than she was used to seeing. Not only was it unusual to have so many patients presenting with arterial thrombosis, it was frequently bilateral.
“We were seeing [patients like this] often, and it was really very striking and caught our attention,” she said. “So, we started looking at what happened to these patients, and indeed they did not do very well.”
The paper was published online July 16, 2020, in Radiology.
Dangers of Long, ‘Gelatinous’ Clots
For the study, Goldman and co-investigators Meir H. Scheinfeld MD, PhD (Montefiore Medical Center), and Kenny Ye, PhD (Albert Einstein College of Medicine, Bronx, NY), retrospectively examined data on 16 patients with COVID-19 who underwent CT angiography of the lower extremities in March and April 2020. Only five COVID-19 patients had leg symptoms alone, with all others having a combination of leg symptoms as well as fever, cough, dyspnea, altered mental status, or hypoxia. A matched-control cohort of 32 patients without COVID-19 who had undergone CT angiography of the lower extremities between the months of January and April in 2018, 2019, and 2020 was used for comparison.
Every COVID-19 patient had at least one thrombus on imaging compared with 69% of controls (P = 0.02). Additionally, the leg thrombi were proximal in 94% of the COVID-19 patients versus 47% of controls (P < 0.001). Even with three different scoring systems, the mean thrombus scores in the COVID-19 cohort were significantly higher than those without the virus.

Treatment included thrombectomy, oral anticoagulants, and amputation. A significant difference in efficacy of thrombectomy was evident, with COVID-19 patients being more likely to need amputation following attempts to remove the clot. To TCTMD, Goldman said re-clotting and inability to establish perfusion was not uncommon, adding that a recent Italian study has described thrombi in some COVID-19 patients as being “unusually gelatinous and very long.”
Goldman and colleagues also found that even when patients who died were excluded, those who had COVID-19 were still more likely than controls to need limb amputation (P = 0.02)
Attention to Legs Important
“I think it's important to remember that this was at the very beginning of the pandemic and the average age of these patients was 78,” Goldman cautioned. “We are hopeful that we are a little bit further along now in our ability to treat these patients.”
Still, she said the message for physicians is to pay attention to the legs in patients with confirmed or suspected COVID-19. “Coldness, or pain, or discoloration sometimes can be the only symptoms. We had that among some of our patients,” she added. “So, I think it's important for clinicians to be aware of this and just maintain suspicion. If patients have these kinds of symptoms, especially with a history of COVID, it's important that they get to the [emergency department] and get evaluated.”
While pseudo-chilblains, or “COVID toes,” have been reported in some patients in the absence of COVID-19 symptoms, or even in the absence of a positive test, Goldman said none of the patients with lower extremity arterial thrombosis had the curiously purple toes.
“I really don't think it's the same phenomenon,” she said, adding that COVID toes “may represent some degree of microthrombosis of minute distal vessels.”
In an email, Behnood Bikdeli, MD (Brigham and Women’s Hospital, Boston, MA), who led a recent state-of-the-art review of antithrombotic and anti-inflammatory strategies that appear promising for COVID-19 patients, called this “another interesting study.” While the most common form of thrombotic disease associated with COVID-19 is venous thromboembolism, he said information on patients with peripheral arterial thrombosis is a new addition.
“The open question that many of us are trying address with randomized studies is how to mitigate the outcomes of these patients,” he added.
L.A. McKeown is a Senior Medical Journalist for TCTMD, the Section Editor of CV Team Forum, and Senior Medical…
Read Full BioSources
Goldman IA, Ye K, Scheinfeld M. Lower extremity arterial thrombosis associated with COVID-19 is characterized by greater thrombus burden and increased rate of amputation and death. Radiology. 2020;Epub ahead of print.
Disclosures
- The authors report no relevant conflicts of interest.


Comments