Even in Ideal Patients, Surgeons Aren’t Doing Multiarterial CABG
A leading proponent of the technique says its time for surgeons to upgrade their skills or refer to those who have them.
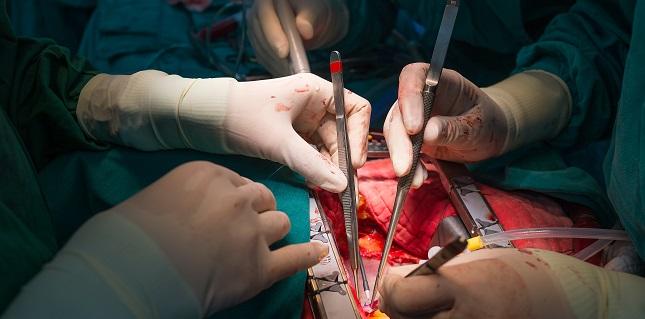
There’s more evidence that even in ideal candidates for the procedure, US surgeons are not performing multiarterial CABG, a technique known to reduce the risks of death, MI, and repeat revascularization.
Among all patients aged 50 years or younger without common comorbidities treated between 2008 and 2018 in the US, the vast majority of surgeons used multiarterial grafting (MAG) in fewer than 25% of cases, according to registry data from the Society of Thoracic Surgeons (STS).
Mario Gaudino, MD (Weill Cornell Medicine, New York, NY), and colleagues report their study results today as a research letter in the Journal of the American College of Cardiology.
Speaking with TCTMD, Gaudino said that his aim with this analysis was “to be a little bit provocative.”
“We know that these patients are not receiving multiple arterial grafting in the United States. There have been previous analyses showing that less than 10% of patients get more than one arterial graft,” he commented. “However, the typical excuse that we as a surgeons use to defend ourselves is: well not all patients benefit from arterial grafting, not all patients fit the criteria to use more than one arterial graft.”
Surgeons are a little bit like fishermen. . . . They will always tell you stories. Mario Gaudino
Surgeons, he continued, will argue that their patients are too sick, too old, that they need other concomitant procedures, or have prohibitive comorbidities. “But you know what? Surgeons are a little bit like fishermen. . . . They will always tell you stories. I wanted to know how things are in reality,” said Gaudino.
A Study of Surgeons, not Patients
“These are the average, low-risk patients that have an operative risk that is well, well below 1% and that come to the hospital to have an elective coronary arterial bypass operation, and these are the patients that based on guidelines, and based on everything we know, [where] you should use multiple arterial grafting,” Gaudino said.
Of the more than 123,000 patients identified between 2008 and 2018, 17,403 had undergone MAG, but the rate of MAG did not significantly increase from the beginning of the study period (9.6%) to the end (13.3%, P for trend = 0.81). Bilateral internal thoracic artery (BITA) was the most common MAG approach (66.1%), while 8.3% of patients received three or more arterial grafts, with BITA plus radial artery being the most common.
But of the 2,671 surgeons captured in this analysis, only three surgeons used MAG in more than 75% of cases, 6% used MAG 25% to 50% of the time, and 87% used MAG in fewer than 25% of cases. Another 6% of surgeons never used a multiarterial approach at all. High-volume surgeons who commonly performed off-pump procedures were also more likely to be high MAG operators (61%), whereas high-volume on-pump CABG surgeons tended to do more single arterial graft procedures (74%).
“Our results show that in the STS database from 2008 to 2018, the use of MAG was extremely low and did not significantly increase, even in an almost ideal CABG population where the use of MAG was recommended by guidelines,” the authors conclude.
Gaudino pointed out that the paper does not include information on patient outcomes. “The thing about this analysis is that it’s a paper on surgeons, not so much on patients,” he told TCTMD. “I didn’t want to do another observational study looking at the use of multiple arterial grafting. . . . That has been done literally hundreds of times and we know the results.”
Instead, “our question is, first of all, what are the surgeons doing? And unfortunately the answer is they are not using multiple arterial grafting and, as I say, they are not following guidelines because guidelines suggest that you should. Second, who are the surgeons who use multiple arterial grafting more often? And I think it’s interesting to see that it’s not so much the volume or the number of CABG cases that they are doing per year, but it’s more the type of coronary surgeon [they are],” he observed.
Joanna Chikwe, MD (Cedars-Sinai Medical Center, Los Angeles, CA), commenting on the paper for TCTMD, zeroed in on this observation. “The big surprise to many will be just how widely individual surgeons vary in their usage, even in this young, super low-risk population,” she said. “Our own research previously showed this in a New York population of patients and also showed the impact this has on long-term life expectancy. This tells us we have really failed to convey a compelling message or any real accountability around multiarterial revascularization.”
Driving Change
Gaudino noted that CABG is considered the “bread and butter” of cardiovascular surgery, representing “60% of what we do as a profession,” so surgeons have been reluctant to accept CABG as something that should be a specialized procedure, one to refer to someone else, the way they do aortic or mitral valve surgeries. But these data point to the fact that some surgeons have become coronary experts and in Gaudino’s opinion, every service should have one coronary specialist on the team who would perform multiarterial grafting in the candidates who require the more complex procedure. This may be young patients, but also very elderly, more complex cases as well, he added.
This tells us we have really failed to convey a compelling message or any real accountability around multiarterial revascularization. Joanna Chikwe
“Even a surgeon who has no specific training can learn relatively quickly how to go from the traditional operation to the use of the mammary and the radial artery, and that will be the right solution for many of the patients who need more than one arterial graft,” Gaudino said. “And then, also, the surgeon needs to acknowledge and accept that there are patients where the use of the radial artery alone is not enough and they require more complex techniques if you want to give them the operation that they need and deserve. And for those patients there is no shame in referring to someone that is a coronary specialist.”
He added: “Everyone can do a CABG, but not everyone can do the right CABG for the right patient. And if we don’t change our mentality, there will be patients who could benefit and instead they will receive an operation that is easier for the surgeon, but is not what they really need.”
Patient sex was the strongest predictor of whether or not a patient would get MAG in this series, with women being 50% less likely to get the more-complex procedure.
“The underutilization in young women suggests that our focus on short-term outcomes like incisional complications, and even transfusion, is driving practice away from more demanding strategies that are all about improving long-term outcomes,” Chikwe said, adding that it is cardiologists who could help to drive practice change, “just as they were instrumental in driving increased use of the left internal mammary artery. The other change that helped get left internal mammary use from less than 80% to above 99% was including it as a surgeon-specific metric in regional and national quality benchmarking. A similar strategy could really improve our use of multiarterial revascularization.”
Eagerly awaited randomized data from the ROMA trial may also help tip the scales. Gaudino, who is leading the trial, gave an update on the study. He noted that while so many other clinical trials have been paused or cancelled during the COVID-19 pandemic, “ROMA has been resilient” because of its international scope.
“While the Chinese sites were shut down, the European sites were enrolling [and] when the European sites were shut down, the Canadian sites were enrolling. We've had probably a 10-15% reduction in enrollment, but we’ve been able to continue, so 2025 is a still reasonable [time frame]. We may be 6 months behind because of the pandemic but more or less that is the time line.”
Shelley Wood was the Editor-in-Chief of TCTMD and the Editorial Director at the Cardiovascular Research Foundation (CRF) from October 2015…
Read Full BioSources
Gaudino M, Rahouma M, Habib RH. Surgeons’ coronary bypass practice patterns in the United States. J Am Coll Cardiol. 2020;76:1714-1718.
Disclosures
- The study authors and Chikwe report no relevant disclosures.


Comments