Femoral Operators Get Bad Rap in Observational Studies, HEAT-PPCI Suggests
Rod Stables says it’s likely wrong to condemn experienced, skilled, and fastidious femoral operators based simply on their choice of access site.
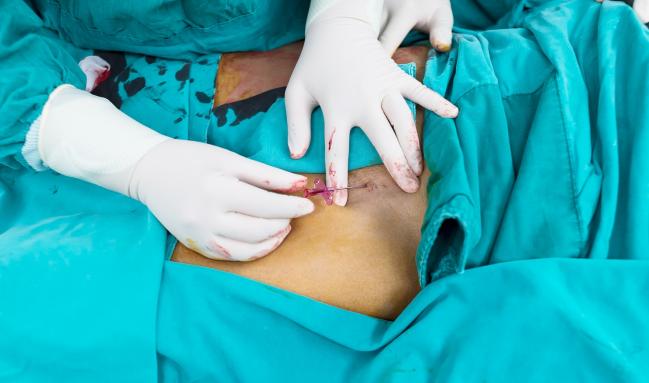
A new analysis of the HEAT-PPCI trial suggests that transfemoral operators might be unfairly maligned, with data showing that physicians experienced with the femoral approach achieve outcomes as good as those achieved by transradial operators.
Published January 16, 2019, in the American Heart Journal, the new study found that when investigators analyzed clinical outcomes by the operators’ default access site choice, there was no significant difference in short-term clinical event rates between procedures performed by transfemoral versus transradial operators. Rates of major bleeding between the two groups also were similar.
“It does suggest that it’s probably wrong to assume that every single femoral operator, especially those that are experienced, skilled, and fastidious, are necessarily underperforming,” senior investigator Rod Stables, MD (Liverpool Heart and Chest Hospital, England), told TCTMD. “We can’t condemn all of them merely based on their approach.”
The updated European Society of Cardiology clinical guidelines for the management of STEMI recommend transradial PCI (class I recommendation) based on several randomized clinical trials, including the large MATRIX study, showing that transradial access in primary PCI is associated with lower mortality and fewer bleeding risks. In the United Kingdom, where radial access is a national quality metric, the latest data from the British Cardiovascular Intervention Society (BCIS) showed that more than 87% of all interventions are performed via the radial artery.
We can't condemn all of them merely based on their approach. Rod Stables
In explaining the rationale for the new analysis, Stables, a high-volume transradial operator, said that at the time of HEAT-PPCI, he was aware of several transfemoral operators at their hospital with excellent clinical outcomes.
“I knew that for more than a decade, their performance in terms of adverse events had never strayed away from the institutional norms,” he said. “So it prompted us to think, if the mere performance of femoral access as a matter of routine creates the adverse outcomes, these operators should have been in trouble for more than a decade, but they weren’t. That prompted us to look at the data in a more measured way.”
Deeper Dive Into HEAT-PPCI
HEAT-PPCI was a single-center, randomized controlled trial comparing unfractionated heparin versus bivalirudin in the treatment of patients with suspected STEMI. When patients were recruited into the trial, they were treated by an operator assigned to the primary PCI case by a rota system, with the arterial access route determined by operator preference. If a physician performed 90% of cases via the radial or femoral artery, that access site was considered their default position.
In total, 1,804 patients went to the catheterization lab for an angiogram, with 1,472 operators opting for transradial access and 332 for transfemoral access. In the head-to-head comparison, use of the radial artery was associated with significantly lower risks of MACE, all-cause mortality, and major and minor bleeding at 28 days compared with transfemoral access.
Clinical Outcomes at 28 Days by Access Site
|
|
All Radial (n = 1,472) |
All Femoral (n = 332) |
P Value |
|
MACE |
6.2% |
10.8% |
0.003 |
|
Mortality |
3.7% |
8.1% |
0.001 |
|
Major Bleeding |
2.6% |
6.6% |
0.001 |
|
Access Site-Related Major Bleeding |
0.3% |
2.1% |
< 0.001 |
|
Minor Bleeding |
8.0% |
18.7% |
< 0.001 |
|
Access Site-Related |
4.0% |
16.6% |
< 0.001 |
“I’m very much a radial operator and do passionately believe that radial is the best option,” said Stables. “It has many, many advantages in different domains, and should be the way of the future.” Nonetheless, a superficial look at their data is an example of how observational studies can lead to conclusions probably not substantiated by the evidence. If you only compared radial versus femoral access in a straight-up comparison, said Stables, “the femoral outcomes look truly appalling” and yet it wouldn’t represent the “complete clinical picture.”
When the analysis was stratified by operators who used their preferred access site, investigators observed no significant difference in the 28-day MACE rates. Similarly, mortality and major bleeding rates were similar between operators who defaulted to their radial and femoral access sites. Rates of minor bleeding remained higher in the transfemoral arm.
Clinical Outcomes at 28 Days by Default Radial and Femoral Operators
|
|
All Radial (n = 1,575) |
All Femoral (n = 229) |
P Value |
|
MACE |
7.0% |
7.0% |
0.97 |
|
Mortality |
4.6% |
3.9% |
0.63 |
|
Major Bleeding |
3.1% |
4.8% |
0.18 |
|
Access Site-Related Major Bleeding |
0.5% |
1.7% |
0.055 |
|
Minor Bleeding |
9.0% |
16.6% |
< 0.001 |
|
Access Site-Related |
5.2% |
14.0% |
< 0.001 |
The researchers also analyzed clinical outcomes among default transradial operators who performed PCI via the femoral artery. Here, the 28-day MACE rate was 18% among patients treated with femoral access by a default transradial operator, a rate that was significantly higher than the 6.7% observed in femoral cases performed by femoral operators (P = 0.003). Mortality and major bleeding rates were also significantly higher when default transradial operators went with the femoral artery.
To TCTMD, Stables stressed that HEAT-PPCI is a single-center study and that while it represents real-world clinical practice, it has modest external validity. More importantly, the number of femoral procedures performed in the study is small, as were the number of femoral operators. For that reason, he urged caution interpreting the results.
Sukhjinder Nijjer, MBChB, PhD (Imperial College, London, England), who was not involved in the study, said that while he trained extensively in femoral access, physician trainees who came after him often have very little exposure to this approach. After switching over to primarily transradial interventions, “I do sweat a little bit when we do a femoral procedure,” he said. “Going to the groin does cause a slight pause.”
For Nijjer, the study suggests that transradial operators aren’t doing well enough when forced into the femoral domain. “It makes sense,” he said. “When we aren’t doing a lot of femoral procedures, it does ‘de-skill’ you. In the days when I used to do 12 or 15 femoral procedures in a day, we wouldn’t bat an eyelid. Now, when I’m doing one, I do have to think a little bit.”
Observational Data Limited
Like Stables, Nijjer cautioned that just 18% of patients in HEAT-PPCI underwent transfemoral PCI, which limits the conclusions. Nonetheless, it’s striking to observe that when a radial operator switches over to the femoral approach, there is a significant and substantial increase in major adverse cardiac events and major and minor bleeding. He noted that closure devices were used in 64.8% of patients treated transfemorally, which is a lower rate than it would be today, particularly in STEMI patients treated with an assortment of antithrombotic drugs; this might have led to the higher rate of bleeding in default radial operators performing transfemoral interventions.
“Why wouldn’t you put a closure device in?” said Nijjer. “It might be because you’ve punctured too low, and the closure device is no longer safe or indicated. That might happen in the hands of somebody who doesn’t do default femoral cases.”
I do sweat a little bit when we do a femoral procedure. Going to the groin does cause a slight pause. Sukhjinder Nijjer
When physicians are training fellows, if there is a need for femoral access, many radial operators don’t feel comfortable allowing the fellow to make the puncture, mainly because they don’t feel comfortable making the puncture themselves, said Nijjer. “This creates a vicious cycle where the fellows won’t be very good femoral operators because they haven’t had a lot of experience doing the punctures and things,” he said. “This tends to be because we’re doing high-risk cases [via the femoral artery]. We don’t want to make a mess of the femoral puncture before the complex case.”
Stables pointed out that if a transradial operator performs a femoral procedure, it’s usually for a good reason. The patient may be in cardiogenic shock, or they might require an intra-aortic balloon pump (IABP), a ventricular assist device such as Impella (Abiomed), or a temporary pacing wire. In HEAT-PPCI, patients treated with femoral access by default radial operators had higher rates of previous MI, CABG, PCI, venous access use, and IABP use than patients treated transfemorally by femoral operators.
“A radial operator performing a femoral procedure is probably a marker of enhanced risk,” said Stables.
Nijjer said that while the BCIS advocates for radial-access interventions, physicians should still maintain their femoral skill set in low-risk patients. “That way when we do the high-risk cases or the STEMIs that need a femoral approach, we can do them very safely,” he said.
Michael O’Riordan is the Managing Editor for TCTMD. He completed his undergraduate degrees at Queen’s University in Kingston, ON, and…
Read Full BioSources
Blake SR, Shahzad A, Aggarwal SK, et al. Radial versus femoral vascular access in ST-elevation myocardial infarction: are the results of femoral operators unfairly represented in observational research. Am Heart J. 2019;Epub ahead of print.
Disclosures
- Stables reports grants from The Medicines Company and AstraZeneca during the conduct of HEAT-PPCI.
- Stables reports grants from The Medicines Company and AstraZeneca during the conduct of HEAT-PPCI. Nijjer reports no relevant conflicts of interest.


Comments