ICD Benefit Questioned in Patients With Chronic Kidney Disease
Implantation of the device was associated with an increase in hospitalizations in this subset and no impact on mortality.
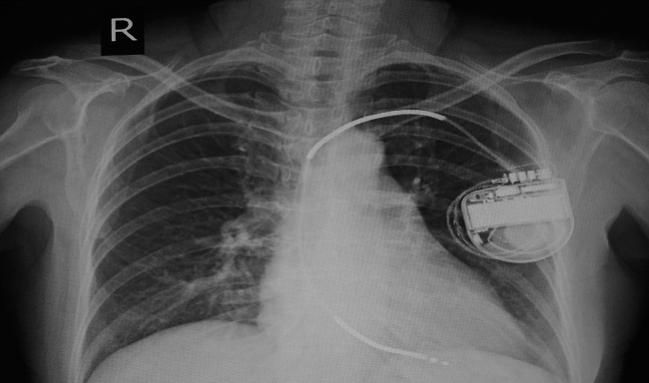
Patients with chronic kidney disease (CKD) and heart failure may not be getting the same benefits associated with use of an implantable cardioverter-defibrillator (ICD) as patients with heart failure alone, an observational analysis suggests.
“We were actually quite surprised by the results,” lead author Nisha Bansal, MD (University of Washington, Seattle) told TCTMD. “We had hoped that ICDs would be associated with improved survival, but in fact we found that ICD implantation in this population was associated with no difference in survival. And then, moreover, ICD implantation was associated with an increased risk of hospitalization, suggesting possible increased morbidity associated with ICD implantation.”
ICDs are commonly used in patients with heart failure, but prior studies have indicated that patients with CKD often don’t respond to standard cardiovascular therapies the same way as other patients, Bansal said. Additionally, patients with CKD have been underrepresented in randomized trials establishing the benefits of ICDs.
To explore the issue, the investigators examined data on ICD-eligible patients with CKD and heart failure with reduced ejection fraction (40% or less) who were enrolled in one of four Kaiser Permanente healthcare systems between 2005 and 2012. The analysis included 1,556 patients with an ICD matched by age, CKD status, and high-dimensional propensity score to 4,321 individuals who did not receive an ICD.
The findings, published online February 5, 2018, ahead of print in JAMA Internal Medicine, should prompt physicians to be more cautious when mulling ICD implantation in their patients with CKD, Bansal observed. In the CKD subset, patients implanted with an ICD did not have a reduction in all-cause mortality (adjusted HR 0.96; 95% CI 0.87-1.06), but they did have higher risks of hospitalization for heart failure (adjusted RR 1.49; 95% CI 1.39-1.60) and hospitalization for any reason (adjusted RR 1.25; 95% CI 1.20-1.30).
During a mean follow-up of 3.1 years, 43.2% of patients died from any cause, 32.7% were hospitalized for heart failure, and 69.6% were hospitalized for any reason. After adjustment for demographics, comorbidities, and cardiovascular medication use, only rates of hospitalization differed between the ICD and no-ICD groups.
It is possible, Bansal speculated, that the increase in hospitalization was related to device complications, including infections and bleeding. She acknowledged, however, that the data could not be used to look specifically at device-related complications.
Bansal said these findings, from what is likely the largest observational study conducted in this area, are thought-provoking. “They’re certainly not definitive, but I do hope that the data from this study prompt more interest in performing a clinical trial to test the efficacy of ICD implantation in patients with chronic kidney disease,” she concluded.
Todd Neale is the Associate News Editor for TCTMD and a Senior Medical Journalist. He got his start in journalism at …
Read Full BioSources
Bansal N, Szpiro A, Reynolds K, et al. Long-term outcomes associated with implantable cardioverter defibrillator in adults with chronic kidney disease. JAMA Intern Med. 2018;Epub ahead of print.
Disclosures
- The study was supported by grants from the National Heart, Lung, and Blood Institute, the National Institute of Diabetes and Digestive and Kidney Diseases, and the US Department of Health and Human Services.
- Bansal reports no relevant conflicts of interest.


Comments