Meta-analysis Affirms Colchicine’s Myriad CV Benefits
Still, a confusing rise in non-CV death merits close scrutiny in upcoming trials to inform the risk-benefit balance.
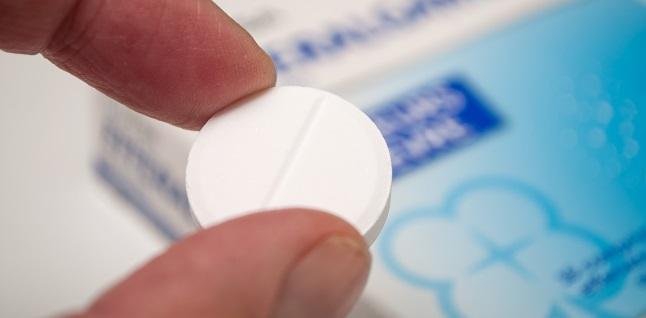
Low-dose colchicine reduces not only MACE but also MI, stroke, and the need for coronary revascularization among patients with known CAD, according to a new meta-analysis that sought to better tease out the anti-inflammatory’s protective effects.
The combined data set includes results for more than 11,000 patients, drawing from LoDoCo2, released during last year’s European Society of Cardiology Congress, as well as the 2013 LoDoCo trial, a 2013 study of colchicine in diabetic patients, the 2019 COLCOT trial, and the 2020 COPS trial. Altogether, the studies capture the evolving body of evidence that increasingly supports the inflammatory hypothesis in cardiovascular disease.
A strength of the meta-analysis is that “we aligned all the endpoints from the various papers, because each paper has its own endpoints, its own definitions,” said Jan H. Cornel, MD (Northwest Clinics, Alkmaar, and Radboud University Medical Centre, Nijmegen, the Netherlands), one of the study’s two senior authors and a principal investigator for LoDoCo2.
While further analyses can be done as follow-up accrues, “these are the most-compelling, most-concise data we have now in the cardiovascular field,” he told TCTMD. There’s robust evidence from the rheumatology field, where the drug has long been given to treat gout, showing chronic use is safe, he said. But there are concerns unique to patients with cardiovascular disease, who might also be taking additional medications like statins that could potentially interact with colchicine. While the news on safety is positive so far, “we are not there yet, . . . because we don’t have real long-term data,” which are especially needed for rare events like death, he said.
Indeed, the meta-analysis did show an increase in noncardiovascular death among colchicine-treated patients. Only time and additional study can reveal whether this “signal” is real, said Cornel.
One pleasant surprise, he said, is that the pooled data pointed to a reduction in stroke, something that is hard to show in a single trial due to its rarity. “Stroke in cardiology is not often witnessed and noted, so . . . you have a low power. But when you combine it, you see a consistent very strong effect on stroke,” said Cornel, adding that this preliminary finding will hopefully be confirmed in the CONVINCE trial.
Overall, said Cornel, the meta-analysis supports the concept that anti-inflammatories represent a third mode of prevention alongside lipid-lowering agents and antiplatelets. “I think the case is stronger and stronger,” he said.
The new paper, with lead authors Aernoud T.L. Fiolet, MD (University Medical Centre Utrecht, the Netherlands), and Tjerk S.J. Opstal, MD (Northwest Clinics and Radboud University Medical Centre), was published online recently in the European Heart Journal.
Fewer MACE
On behalf of the Colchicine Cardiovascular Trialists Collaboration, Fiolet et al identified five randomized trials with a total of 11,816 patients. All had established CAD, 46.9% were within 30 days of ACS when first enrolled, and 53.1% had chronic coronary disease. Nearly nine in 10 had a history of ACS. Among the patients with details on baseline medication use, 94.8% were taking antiplatelet therapy, 96.4% were on statins, and 74.7% were taking beta-blockers.
The primary efficacy endpoint of MACE, including MI, stroke, or CV death, occurred in 578 patients. Colchicine decreased the pooled relative risk of this composite as well as MI, stroke, and coronary revascularization. There was no difference in all-cause death; however, there was a trend toward less cardiovascular death and, in the opposite direction, a trend toward more non-CV death with colchicine.
Outcomes With Versus Without Colchicine
|
|
RR |
95% CI |
|
MACE (MI, Stroke, CV Death) |
0.75 |
0.61-0.92 |
|
MI |
0.78 |
0.64-0.94 |
|
Stroke |
0.54 |
0.34-0.86 |
|
Coronary Revascularization |
0.77 |
0.66-0.90 |
|
Death All-Cause CV Non-CV |
1.08 0.82 1.38 |
0.71-1.62 0.55-1.23 0.99-1.92 |
The reduction in the primary endpoint was similar regardless of whether patients had ACS or chronic disease and whether they were men or women.
Safety data from COLCOT, COPS, and LoDoCo2 showed no difference in hospitalizations for infection, including for pneumonia in particular, or for gastrointestinal disorders based on whether patients were taking colchicine. In addition, there was no difference in new cancer diagnoses.
A Signal for Non-CV Death?
Aruna D. Pradhan, MD (Brigham and Women’s Hospital, VA Boston Medical Center, MA), who wrote an accompanying editorial, says the results for non-CV mortality are “appropriately highlighted” by the investigators.
“While not statistically significant at the alpha level of 0.05, this observation should prompt careful scrutiny of completed trials and meticulous data collection in ongoing trials in order to amplify safety signals,” she notes, asking: “How alarmed should we be by the information presented?”
One reassurance is that the causes of noncardiovascular death were what would be common in a population of older adults with heart disease, says Pradhan. “There was no apparent imbalance in unusual causes of noncardiovascular death that would imply drug toxicity, although all counts are low and three of the included trials did not provide cause-specific data, thereby limiting interpretability. So perhaps noise and not signal, but inconclusive based on the available data.”
Cornel said that, from his perspective, “there’s no biological reason” why there would be a rise in noncardiovascular mortality with colchicine. It may be that deaths from a cardiovascular cause are being misclassified, he suggested. For instance, a person who dies by drowning may have had an arrhythmia that led to the accident.
Another possibility relates to competing risks, Cornel continued. “This is an elderly population. There are comorbidities. And when you live a little bit longer because of an advantage in cardiovascular death, of course you are at risk for something you couldn’t have [had otherwise]—you cannot die twice.”
Pradhan also proposes this explanation: “Is it possible that the increased occurrence of noncardiovascular death in the colchicine group is due to a life-extending reduction in cardiovascular death that renders these high-risk individuals susceptible to other fatal exposures? Death from cardiovascular disease is delayed long enough for competing causes of death to take effect.” Without considering these competing risks, underlying mortality trends might be distorted, she observes.
Luckily, there are no fewer than nine colchicine trials on the way with cardiovascular or total mortality as prespecified endpoints, expected to enroll more than 12,000 participants, Pradhan says. These include CONVINCE in patients who’ve had ischemic stroke or TIA, as well as CLEAR SYNERGY in patients who’ve undergone PCI for acute MI, COLICA in acute heart failure, COP-AF in patients who’ve undergone major thoracic surgery, CONVERT-MI in PCI, IMPROVE-PVI Pilot in peripheral vascular interventions, COCS in the post-CABG setting, Effect of Colchicine in Patients With MI, and CADENCE in patients who’ve had stroke/TIA.
Caitlin E. Cox is Executive Editor of TCTMD and Associate Director, Editorial Content at the Cardiovascular Research Foundation. She produces the…
Read Full BioSources
Fiolet ATL, Opstal TSJ, Mosterd A, et al. Efficacy and safety of low-dose colchicine in patients with coronary disease: a systematic review and meta-analysis of randomized trials. Eur Heart J. 2021;Epub ahead of print.
Pradhan AD. Time to commence or time out for colchicine in secondary prevention of cardiovascular disease? Eur Heart J. 2021;Epub ahead of print.
Disclosures
- Fiolet and Cornel report no relevant conflicts of interest.
- Pradhan reports receiving investigator-initiated research support from Kowa Research Institute and serving as co-principal investigator of the PROMINENT trial.



Comments