Nitroglycerin Given Early or Late Fails to Prevent Radial Artery Occlusion: PATENS
Operators are still looking for the best way to minimize or eliminate RAO so the artery can be used for future procedures.
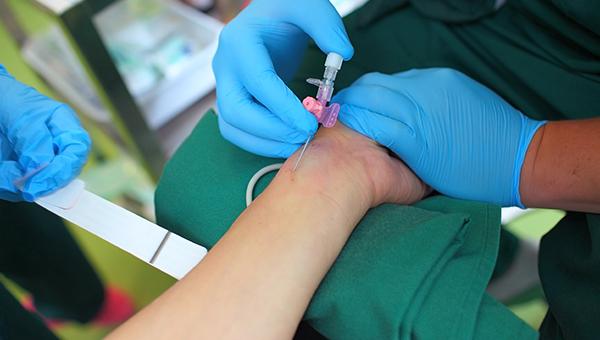
Administering nitroglycerin during the course of transradial cardiac catheterization fails to reduce the risk of radial artery occlusion, according to results from the large PATENS trial.
Whether nitroglycerin was administered early upon sheath insertion or just before the sheath was removed did not impact the occurrence of radial occlusion, report investigators.
Preserving the radial artery for future interventions is critical given that transradial access is associated with lower rates of vascular and bleeding complications and a lower risk of mortality in high-risk patients, lead investigator Roberto Léo da Silva, MD (Instituto de Cardiologia de Santa Catarina, Brazil), told TCTMD. “Nowadays, it’s common for patients to need one, two, or three procedures” over their lifetime, he said.
While radial artery occlusion was once considered a “unique” phenomenon, there is increasing recognition that it can pose a real challenge for patients and operators. Today, “even with the best practices, the incidence is still 2% to 3%,” said da Silva.
Nitroglycerin is commonly used in the cath lab as a prophylactic vasodilator to prevent radial artery spasm. Researchers speculated that nitroglycerin, by limiting inflammation and intimal hyperplasia that results from trauma to the radial artery with transradial access, might also promote regional flow and facilitate patent hemostasis.
More Than 2,000 Patients Randomized
The 2 x 2 factorial study, published this week in JACC: Cardiovascular Interventions, and scheduled for presentation at upcoming the American College of Cardiology Scientific Sessions, included 2,040 patients randomized to either 500 µg of nitroglycerin or placebo early (upon sheath insertion) or late (just before sheath removal) during cardiac catherization at three high-volume centers in Brazil between 2017 and 2021.
Patients were eligible for randomization if the operator used transradial access and 5- or 6-Fr sheath size during coronary angiography or PCI. All patients received an initial intraarterial dose of heparin (5,000 IU) with sheath insertion, and additional doses were given with coronary interventions.
At the completion of the procedure, hemostasis was achieved by a staff member blinded to randomization. A pneumatic compression device was used to assist hemostasis at the arterial puncture site, and the wristband was adjusted to the lowest possible pressure. Radial artery patency was evaluated with vascular duplex Doppler ultrasound within 24 hours of removing the compression band.
We need to try to do better for our patients. Roberto Léo da Silva
The incidence of radial artery occlusion was not significantly different with nitroglycerin when administered early compared with placebo (2.5% vs 2.3%), nor was the incidence any different compared with placebo when administered late (2.3% vs 2.5%). Analyses showed no benefit of nitroglycerin in any of the subgroups, and a test for interaction revealed no sex-based differences. There was also no significant interaction between diagnostic and therapeutic procedures in the occurrence of radial artery occlusion.
The early administration of nitroglycerin was associated with a trend toward less radial artery spasm compared with placebo (10.8% vs 13.4%; P = 0.067). In multivariate analysis, arterial spasm and requiring more than one puncture attempt were predictors of radial artery occlusion at 24 hours. In PATENS, all arterial punctures were obtained without ultrasound guidance.
“Unfortunately, our study showed there was no difference in the rate of radial occlusion with the use or not of nitroglycerin,” said da Silva. He added that while their study reported quite a low rate of radial occlusion overall, there is a need for improving best practices to reduce this risk even further. “We need to try to do better for our patients,” he said.
Adhered to Best Practices
In an editorial, Ziyad Ghazzal, MD, and Omar Chaabo, MD (both American University of Beirut, Lebanon), also comment on the very low overall rate of radial artery occlusion (2.4%), which can be attributed to providing adequate procedure anticoagulation, following a dedicated hemostasis protocol, and using an adjustable closure device set at the lowest possible compression pressure.
The editorialists point out that while the study showed that nitroglycerin given late was not associated with reduced occlusion rates, this doesn’t mean that vasodilator therapy administered at the beginning of a transradial procedure should be discontinued.
“[T]he use of vasodilator therapy at the time of radial sheath insertion will still be routinely used in the prevention of radial artery spasm in order to lessen patient discomfort, ease catheter manipulation, and reduce changes produced by local trauma that could potentially result in radial artery occlusion,” Ghazzal and Chaabo write. “In particular, the widely used combination of nitroglycerin and verapamil should not be disregarded and should be similarly prospectively tested for their effect on spasm and radial artery patency.”
To TCTMD, da Silva said future studies might test verapamil, other vasodilators, or different combinations for preventing radial occlusion. He noted that animal studies have even hinted that nitric oxide-eluting sheaths can decrease spasm and inflammation, as well as reduce the risk of thrombosis. “Perhaps, it might be a way to go,” said da Silva.
Michael O’Riordan is the Managing Editor for TCTMD. He completed his undergraduate degrees at Queen’s University in Kingston, ON, and…
Read Full BioSources
Da Silva RL, de Andrade PB, Dangas G, et al. Randomized clinical trial on prevention of radial occlusion after transradial access using nitroglycerin (PATENS trials). J Am Coll Cardiol Interv. 2022;Epub ahead of print.
Ghazzal Z, Chaabo O. Preserving the golden access: importance of best practices. J Am Coll Cardiol Interv. 2022;Epub ahead of print.
Disclosures
- Authors and editorialists report no relevant conflicts of interest.



Comments