Obesity May Boost Thrombotic Events in Contraceptive Users, Review Suggests
The association highlights the importance of discussing CV health early in a woman’s reproductive years, an expert says.
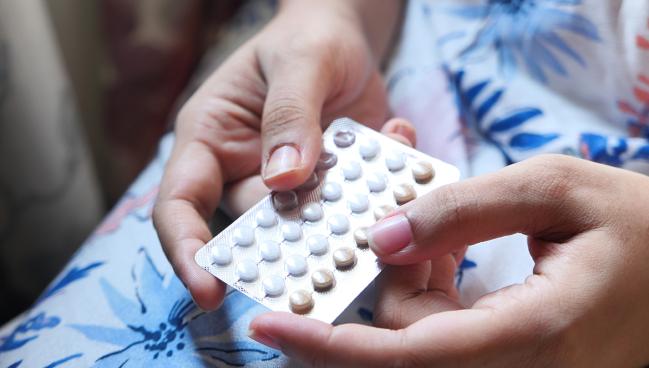
Being overweight or obese may increase CV risk, mainly the risk of venous thromboembolism (VTE), in women of reproductive age taking combined oral contraceptives (COCs), a new review suggests.
While the link between increased risk of thromboembolic events and COCs containing estrogens has been known for decades, the analysis of existing literature indicates a high likelihood that the combination of being overweight or obese potentiates risk of thromboembolic events compared with women who are not overweight.
In the review article by Giuseppe M.C. Rosano, MD, PhD (IRCCS San Raffaele Pisana, Rome, Italy), they cite a large population-based study showing that having a body mass index (BMI) of more than 25 but less than 30 (overweight) was associated with a 1.7-fold increased risk of VTE in women in the general population, while having a BMI of > 30 (obese) was associated with a 2.4-fold increased risk of VTE. But when those women took COCs, their risks increased dramatically, to twelvefold in the overweight group and 24-fold in the obese group compared with normal-weight women not taking COCs.
“The combination of obesity and COCs use appears to potentiate the pro-inflammatory state in young women and trigger the cardiovascular risk increase,” Rosano and colleagues write in ESC Heart Failure. They say this apparent synergistic effect of obesity and COCs on thromboembolic risk must be considered when prescribing hormonal contraception.
Commenting on the review for TCTMD, Kathryn J. Lindley, MD (Washington University Medical Center, St. Louis, MO), said it highlights the continued rise in prevalence of overweight and obesity among women of childbearing age, which is a risk factor not only for thromboembolism, but also long-term CVD.
“Combined hormonal contraceptives do carry an increased risk for all patients for developing thromboembolism, and it is certainly a higher risk for patients who are overweight or obese, who are smokers, and who have other predisposing factors, including certain underlying cardiovascular conditions,” Lindley said. “However, the important things to think about when we're putting this into context for patients is that the risk is still substantially lower than the risk of thromboembolism during pregnancy and the postpartum period.”
Both the review authors and Lindley say the concerns regarding COCs combined with excess body weight should spur conversations about other forms of contraception that are safer, including those that contain only progestin.
Rosano and colleagues point to several studies and a meta-analysis included in their review that support the suggestion that neither the levonorgestrel-releasing intrauterine device (IUD) nor subcutaneous contraceptive implants significantly increase the risk of VTE or other cardiometabolic events, including MI, stroke, hypertension, or diabetes. The one exception is the injectable progestin-only option depot medroxyprogesterone (DMPA), which they say was associated with a 2.6-fold increased risk of VTE in a systematic review and meta-analysis.
“I would say that we typically would want to prioritize the long-acting reversible methods of contraception, such as the IUD or the subdermal implant, both for safety and effectiveness reasons for patients with obesity or other underlying cardiovascular risk factors,” Lindley commented. “It's important that we not only work with those patients to help them find ways to address their obesity, but also help them find safe and effective ways to help prevent unplanned pregnancies.”
Rosano and colleagues agree, saying their recommendation is “to exercise caution with the use of COCs in patients with overweight and obesity,” choosing the safest alternatives when prescribing hormonal contraception.
For Lindley, the review also highlights the importance of talking about CV health early in a woman’s reproductive years when they tend to have significant interaction with the healthcare system when seeking contraception and during pregnancy.
“This is an opportunity for us to counsel those patients on their risk and to work with them to identify lifestyle and pharmacologic interventions that can really change the trajectory of their entire life in terms of their long-term cardiovascular health,” she added.
L.A. McKeown is a Senior Medical Journalist for TCTMD, the Section Editor of CV Team Forum, and Senior Medical…
Read Full BioSources
Rosano GMC, Rodriguez-Martinez MA , Spoletini I, Regidor PA. Obesity and contraceptive use: impact on cardiovascular risk. ESC Heart Failure. 2022;Epub ahead of print.
Disclosures
- Rosano and Lindley report no relevant conflicts of interest.





Comments