One in Five CABG Patients Develop New-Onset Atrial Fibrillation: EXCEL
The condition is not benign either, with these patients at a significantly increased risk of death and stroke, report researchers.
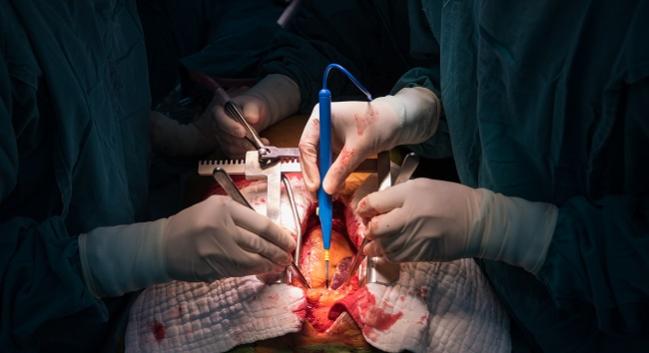
Nearly one in five patients undergoing coronary artery bypass graft surgery for left main disease develop atrial fibrillation after the procedure, according to an analysis of the EXCEL trial. New-onset atrial fibrillation is not benign either, say investigators, with these patients spending more time in the hospital and being more likely to have a major or minor bleed at 30 days.
Most importantly, new-onset atrial fibrillation was associated with a more than fourfold increased risk of stroke at 3 years and a threefold increased risk of death.
“For patients who are referred for surgery for left main disease, or any extensive degree of coronary disease, physicians need to much more attune to the occurrence and prognostic importance of atrial fibrillation,” senior investigator Gregg Stone, MD (NewYork-Presbyterian/Columbia University Medical Center, New York, NY), told TCTMD. “They need to look for it carefully and to not only treat it acutely but also consider presurgical prophylaxis to try to prevent it, with perioperative beta-blockers or amiodarone.”
Secondly, if atrial fibrillation is evident following cardiac surgery, Stone recommends considering intense device-based monitoring to assess its recurrence or treat such patients with oral anticoagulation.
Speaking with TCTMD, Subodh Verma, MD, PhD (St. Michael’s Hospital, Toronto, Canada), who wrote an editorial accompanying the analysis, said new-onset atrial fibrillation is a recognized complication of CABG surgery, but there is still a lot unknown. In the post-cardiac surgery setting, the incidence ranges from 15% to 48%, but these studies mainly focused on the risk in the hospital.
“From my perspective as a cardiac surgeon, [the EXCEL analysis] highlights a very important, understudied area of postoperative atrial fibrillation,” he said. “I see the paper more from that lens, in that atrial fibrillation after open heart surgery is grossly underestimated and its gravitas is not well appreciated. People used to believe that this was a transient phenomenon that likely wasn’t sinister, but it seems like it’s exceedingly common and it is quite sinister in that it’s associated with significantly worse outcomes.”
The study was published online ahead of print in the February 20, 2018, issue of the Journal of the American College of Cardiology.
Higher All-Cause Death, CV Death, and Stroke at 3 Years
The EXCEL study, presented and published in 2016, compared two revascularization strategies—CABG surgery and PCI—for the treatment of unprotected left main coronary artery disease. As reported by TCTMD, the trial showed that patients treated with an everolimus-eluting metallic stent (Xience; Abbott Vascular) had comparable rates of death, stroke, or MI at 3 years when compared with patients treated with CABG surgery.
In EXCEL, new-onset atrial fibrillation developed in 162 of 1,812 patients (8.9%) at a mean of 2.7 days after coronary revascularization. Just one patient treated with PCI developed the arrhythmia; the remaining cases were documented in CABG-treated patients (0.1% vs 18.0%; P < 0.0001). Older age, larger body mass index, and a lower left ventricular ejection fraction were all independent predictors of new-onset atrial fibrillation.
At the time of discharge, atrial fibrillation had resolved in 85.8% of patients. Still, hospitalizations were longer in those with the arrhythmia (14.3 vs 10.9 days; P < 0.0001), and these patients were more likely to be discharged on warfarin or a novel oral anticoagulant. Overall, 10.2% of patients with the complication were discharged on oral anticoagulation (all warfarin).
At 3 years, new-onset atrial fibrillation was an independent predictor of all-cause and cardiovascular mortality, stroke, and the composite endpoint of all-cause mortality, MI, or stroke in the overall population and in the CABG-treated arm. On multivariable analysis, it was associated with increased risks of all-cause mortality (HR 3.02; 95% CI 1.60-5.70), cardiovascular death (HR 4.86; 95% CI 2.27-10.44), and stroke (HR 4.19; 95% CI 1.74-10.11) in the CABG arm.
To TCTMD, Stone said the incidence of atrial fibrillation after cardiac surgery observed in EXCEL is within the range expected based on previous studies. The different rates observed between cardiac surgery and PCI were striking, he said, and had a significant effect on the results. “Given the deleterious effect [it] had on the CABG patients, had it not occurred, the relative prognosis of surgery versus PCI would have looked much better,” said Stone.
Regarding the variables that identified patients at higher risk for the complication, Stone said it’s premature to stratify such patients to PCI in order to potentially avoid the arrhythmia. That said, physicians should be more cognizant of monitoring and/or using preventive strategies in older patients, those with higher BMIs, and those with reduced ejection fractions.
SEARCH-AF Study Underway
Verma told TCTMD the present analysis highlights the need for ongoing clinical trials to further define the natural history and incidence of postoperative atrial fibrillation. Some reports have stated that the incidence 30 days after surgery ranges from 2% to 5%, although this is likely an underestimation.
Alongside Atul Verma, MD (Southlake Regional Health Center, Newmarket, Canada), and Andrew Ha, MD (University Health Network, Toronto, Canada), Verma is leading the SEARCH-AF study, a clinical trial assessing the incidence of atrial fibrillation/atrial flutter within 30 days of cardiac surgery. In SEARCH-AF, these events will be documented using continuous cardiac rhythm monitoring (SEEQ mobile cardiac telemetry; Medtronic).
“The impact of diagnosing atrial fibrillation in a patient population with a high CHA2DS2-VASc score is very important because prevention and treatment can have a significant impact,” said Verma.
In the editorial, Verma and coauthors Atul Verma and Deepak Bhatt, MD (Brigham and Women’s Hospital, Boston, MA), state that if postoperative atrial fibrillation is evident outside the subacute phase, it would warrant oral anticoagulant therapy, particularly if patients are at high risk for stroke.
The SEARCH-AF study investigators plan to evaluate the number of participants who are prescribed oral anticoagulation for atrial fibrillation/flutter. Oral anticoagulant use, prescribed by the treating physician at their discretion, will be measured at 45 days, 6 months, and 9 months after surgery. Rates of bleeding, hospitalization, and major adverse cardiac outcomes will also be assessed at 45 days.
Note: Stone and several co-authors of the paper are faculty and/or staff members of the Cardiovascular Research Foundation, the publisher of TCTMD.
Michael O’Riordan is the Managing Editor for TCTMD. He completed his undergraduate degrees at Queen’s University in Kingston, ON, and…
Read Full BioSources
Kosmidou I, Chen S, Kappetein AP, et al. New-onset atrial fibrillation after PCI or CABG for left main disease: the EXCEL trial. J Am Coll Cardiol. 2018;71:739-748.
Verma A, Bhatt DL, Verma S. Long-term outcomes of post-operative atrial fibrillation: guilty as charged. J Am Coll Cardiol. 2018;71:749-751.
Disclosures
- Abbott Vascular funded the EXCEL trial.
- Stone’s employer, Columbia University, receives royalties from Abbott Vascular for the sale of the MitraClip.
- Verma reports receiving research grants from Boehringer Ingelheim and Bristol-Myers Squibb-Pfizer and speaker’s honoraria from Bayer Healthcare, Boehringer Ingelheim, Bristol-Myers Squibb, Pfizer, and Servier.


Comments