Radial PCI Up, but Vascular Complication Rates Haven’t Budged
The highest-volume radial operators seem to have the lowest overall vascular complication rates, however.
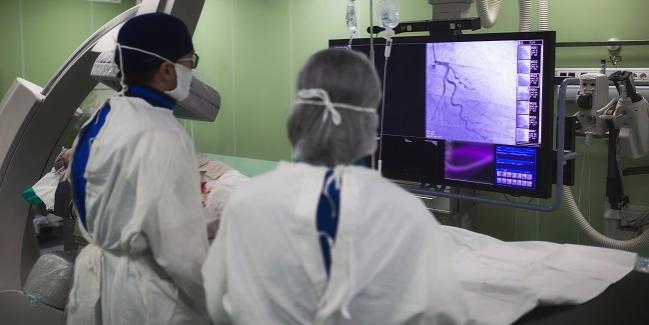
PCI via a transradial approach has increased since 2013, but the rate of vascular access-site complications (VASC) has remained steady, according to a new study. The authors attribute this phenomenon to an increased incidence of these complications following transfemoral PCI and more use of secondary vascular access.
“There has been a lot of energy expended on the radial versus femoral debate,” senior author Hitinder S. Gurm, MBBS (University of Michigan, Ann Arbor), told TCTMD in an email. “We believe that both approaches have merit, and a good operator is the one who is good at both and can pick the correct approach for a given patient. We also need to ensure that the increasing adoption of radial access does not come at the loss of femoral management skills.”
Transradial PCI has an established track record when it comes to reducing vascular-access complications, but some have raised concerns that as more people turn to a radial approach, their transfemoral skills will slide—raising the risk of problems when femoral access is necessary.
For the study, published online yesterday ahead of print in JACC: Cardiovascular Interventions, Gurm along with David Kopin, MD (University of Michigan, Ann Arbor), and colleagues looked at data from the Blue Cross Blue Shield of Michigan Cardiovascular Consortium (BMC2) registry for all 153,123 patients who underwent PCI at 48 Michigan institutions between 2013 and 2017.
Over the study period, substantial increases were observed in both transradial PCI (25.9% to 45.2%) and a need for secondary vascular access (4.9% to 8.7%). However, there was minimal change in the rate of overall vascular access-site complications (1.2% to 1.4%). The unadjusted rates of these complications increased after both transfemoral (1.6% to 2.3%; P < 0.001) and transradial PCI (0.2% to 0.4%; P = 0.019), with hematoma and pseudoaneurysm being the most common events.
In an analysis of 2017 procedures adjusted for patient characteristics and clinician experience—operators were stratified into tertiles based on the proportion of cases done with transradial access—procedures done by those with the least experience in radial access were less likely to result in transfemoral vascular access-site complications. Also, patients treated by operators with the most radial-access experience were less likely to have any vascular complications.
Vascular Access-Site Complications by Radial Experience
|
|
Adjusted OR |
95% CI |
|
Femoral VASC |
|
|
|
Tertile 3 vs 1 |
1.51 |
1.08-2.13 |
|
Tertile 2 vs 1 |
1.38 |
1.03-1.85 |
|
Any VASC |
|
|
|
Tertile 3 vs 1 |
0.62 |
0.46-0.83 |
|
Tertile 2 vs 1 |
0.94 |
0.72-1.47 |
Notably, use of secondary vascular access, which increased more dramatically among transfemoral than transradial procedures, was associated with a greater risk of complications (OR 5.82; 95% CI 5.26-6.43).
Crossovers were most often observed among transfemoral PCIs (3.09% vs 0.33%), and these were linked with a greater rate of vascular access-site complications compared to noncrossover procedures (3.32% vs 1.78%; P < 0.0001).
Does This Support Campeau’s Paradox?
Gurm said that he had expected a decline in overall vascular complications with increasing radial use and was surprised not to see this. “The increase in secondary access is much greater than I would have anticipated, and these patients have more complications,” he said. “This is noteworthy and needs more focused quality improvement.”
However, Robert W. Yeh, MD (Beth Israel Deaconess Medical Center, Boston, MA), who was not involved in the study, told TCTMD that the results were as he would have guessed. “The growth in transradial use has been seen in other populations—we know this has been happening,” he said, adding that the increase in secondary access site use, largely for chronic total occlusion and mechanical circulatory support procedures, is “counterbalancing” the reduction in vascular complications achieved through increased transradial procedures. “Most of the results are predictable and not surprising. Although, obviously [this is] a good update for the field on where the state is currently of transradial/transfemoral access,” he said.
In an accompanying editorial, Marco Valgimigli, MD, PhD, and Felice Gragnano, MD (both from Bern University Hospital, Switzerland), write that the study findings don’t support the so-called Campeau Paradox, where femoral proficiency is hypothesized to be lost with increased radial experience.
Because the comparison of complications from 2013 to 2017 in this analysis was unadjusted, “one may argue that radial use may have contributed to minimizing the overall VASC increase to only 0.2% in absolute terms,” they write. Also, “patients treated by operators in highest radial tertile had 38% less chance to experience any VASC compared with those treated by operators in the lowest tertile. Thus, the most experienced radial operators (suspected for being the most deskilled femoral operators) were solely able to concretely reduce the overall risk of VASC.”
It’s also possible that femoral access led to more complications “considering that even for operators in the lowest tertile of radial use, the rate of VASC was higher for femoral (1.8%) than radial (0.4%),” the editorialists continue. “Finally, the more experienced the operator for radial access is, the more complex and highly selected are patients requiring crossovers to femoral access. Therefore, the fact that dedicated radial operators had a higher complication rate for secondary femoral access when compared with low-volume radial operators (or routine femoral patients) may speak for selection bias, more than for lack of femoral expertise. Unfortunately, the authors did not specifically address this point, and the analysis is nonconclusive in this regard.”
Yeh agreed. “I don't think that this paper shows any demonstration of the so-called Campeau's paradox,” he said. “I would expect operators who reserve only transfemoral access for their most-sick patient populations to have a higher rate of femoral access site complications, but the more interesting finding the authors have is that those operators who do the most transradial clearly had the lowest overall vascular complication rate. That's what patient's care about. . . . So some operators clearly are doing a better job than others, and the ones that appear to be doing the best job are the ones who do transradial the most.”
There are several reasons why this might be, Yeh explained. Notably, transradial access has not increased among the STEMI population, and they might stand to benefit the most, which creates a “risk/treatment paradox,” he said. “In a situation where you only move from 20-something percent transradial to 40-something percent transradial in your population and the increase tends to be concentrated in the lowest-risk patient population, I wouldn't expect to see huge movement on vascular access-site complications,” Yeh explained. “That movement is going to come when people start becoming comfortable doing their highest-risk procedures with transradial access.”
Still, Gurm argued that the goal of this study “was not to try and address the comparative efficacy of femoral versus radial access—we know that radial has lower complications. . . . The patients who were treated by the high radial users had a higher femoral complication rate, [and] that persisted even after we adjusted for the differences in patient complexity. However, it is important to note that these operators had the lower overall complication rate.”
The Future of Training
Going forward, Gurm stressed the importance of maintaining competence in both radial and femoral access among all operators.
“We believe that training for femoral access and groin management will require greater education in the future,” he said. “This should involve tools like simulation since the proportion of patients treated via a femoral approach will continue to decline (and this decline will be greater in training programs since a larger number of them have switched to [the] radial-first approach). Our radial training has gotten better, but it should not come at the cost of reduction in femoral-access proficiency.”
Here, Yeh as well as Valgimigli and Gragnano are on the same page. “You need to be comfortable enough with transradial skills to use them ‘when it really counts’ in those highest-risk situations, but you need to be comfortable with your transfemoral skills for situations where we don't have radial alternatives, like for very large bore access or mechanical circulatory support,” said Yeh. “Training needs to involve both and I think that it does.
“I'm less concerned about operators who are in practice who have done a lot of transfemoral losing their transfemoral skills [than] I am about newly trained operators who just haven't seen enough femoral in their careers so they are a little bit less comfortable with it,” he continued. “But the good thing that's happened in femoral training is now I think almost universally at most of the major training centers, femoral access involves micropuncture and ultrasound guidance in a way that wasn't true when I was training. I think that's really improved. It's taken a lot of the guesswork out of femoral access, and it's made it safer.”
“The best interventional cardiologists are those maintaining high expertise in both radial and femoral access, making individual access-site decisions based on clinical variables and technical procedural considerations,” the editorialists conclude. “The interventional cardiology community can best serve patients by having operators who are proficient with both the arm and the leg.”
Yael L. Maxwell is Senior Medical Journalist for TCTMD and Section Editor of TCTMD's Fellows Forum. She served as the inaugural…
Read Full BioSources
Kopin D, Seth M, Sukul D, et al. Primary and secondary vascular access site complications associated with percutaneous coronary intervention: insights from BMC2. J Am Coll Cardiol Intv. 2019;Epub ahead of print.
Valgimigli M, Gragnano F. The use of radial access for cardiac catheterization: slowly, but yet it moves. J Am Coll Cardiol Intv. 2019;Epub ahead of print.
Disclosures
- The study was supported by the Blue Cross Blue Shield of Michigan and Blue Care Network as part of the Blue Cross Blue Shield of Michigan Value Partnerships program.
- Gurm reports serving as a consultant to Osprey Medical and receiving research funding from the National Institutes of Health Center for Centers for Accelerated Innovation (NCAI) and Blue Cross Blue Shield of Michigan.
- Valgimigli reports receiving grants from Abbott, Terumo, Medicure, and AstraZeneca and personal fees from Abbott, Bayer, Daiichi Sankyo, Amgen, Terumo, Alvimedica, AstraZeneca, Idorsia, Coreflow, Vifor, Bristol Myers Squib SA, and iVascular.
- Kopin, Gragnano, and Yeh report no relevant conflicts of interest.


Comments