Score May Help Guide VITT Management After COVID-19 Vaccination
It “can help draw people’s attention to how severe the disease may be and how aggressive to treat them,” Jean Connors says.

A score incorporating a handful of demographic, clinical, and laboratory findings can provide an estimated mortality risk in patients presenting with vaccine-induced immune thrombotic thrombocytopenia (VITT) after COVID-19 vaccination, potentially helping clinicians decide how aggressive to be when treating the rare complication.
Having a simple tool to risk-stratify patients, knowing effective treatments are available, might help alleviate some of the vaccine hesitancy that arose when this phenomenon was first documented, researchers say.
Researchers identified five factors associated with mortality among the earliest reported cases of VITT, also called thrombosis with thrombocytopenia syndrome (TTS), in patients who had received the adenoviral-vector vaccine from Oxford/AstraZeneca. Using age ≤ 60 years, platelet count < 25,000/µL, fibrinogen < 150 mg/dL, and presence of either intracerebral hemorrhage (ICH) or cerebral venous thrombosis (CVT), investigators then assigned 1 point to each to form the FAPIC (fibrinogen, age, platelet count, ICH, and CVT) score.
The expected rate of death increased with each 1-point rise in score:
- 0 (2.1%)
- 1 (6.66%)
- 2 (19.31%)
- 3 (44.54%)
- 4 (72.94%)
- 5 (90.05%)
The FAPIC tool had good discrimination (C-statistic 0.837), which held up in internal and external validation data sets, Jimin Hwang, MD (Johns Hopkins Bloomberg School of Public Health, Baltimore, MD), and colleagues report in a study published online this week in the European Heart Journal.
“The FAPIC score could be used in the clinical setting to recognize TTS patients at high risk of adverse outcomes and provide early intensive interventions, including intravenous immunoglobulins and nonheparin anticoagulants,” they say.
Though noting some limitations and the need for validation in larger cohorts, Jean Connors, MD (Brigham and Women’s Hospital, Boston, MA), agreed the tool could be used today. “For someone who deals with those numbers in the scoring system—like the platelets and the fibrinogen—all the time, it’s kind of intuitive that these are severe abnormalities, but they may not be to an emergency room doctor or intensive care unit doctor,” she commented to TCTMD. She added that the FAPIC score “can help draw people’s attention to how severe the disease may be and how aggressive to treat them.”
Clinical Characteristics, Treatment of VITT
With reports emerging in recipients of the Oxford/AstraZeneca vaccine shortly after countries starting ramping up their COVID-19 vaccination programs, VITT, or TTS, has been likened to autoimmune heparin-induced thrombocytopenia (HIT). The complication, which is considered rare in the context of billions of doses administered around the world, has since been identified in patients receiving another adenoviral-vector vaccine, the Janssen vaccine from Johnson & Johnson (with only a few cases associated with the mRNA vaccines).
Hwang et al pooled data from the initial published reports associated with the Oxford/AstraZeneca vaccine to explore clinical manifestations and outcomes of VITT and to determine factors associated with mortality. The analysis included six case series and 13 case reports with a total of 64 patients. Most (68.5%) were women, and their ages ranged from 21 to 71 (median 45). They presented 5 to 24 days after vaccination (median 10 days).
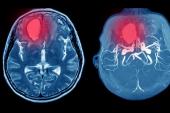
The researchers confirmed that the condition was similar to HIT. The most common symptoms were neurological, with 73.3% of patients with available data having headache; hemiparesis, visual disturbance, and hemiplegia were frequently observed as well. That’s consistent, Hwang et al say, with the presentation of typical CVT, which was present in more than half of patients (59.4%).
Systemic, GI, and bleeding symptoms were also commonly seen, and all patients had thrombocytopenia (mean platelet count 31,000/µL). The vast majority of patients (95.3%) had thrombosis, with 35.9% having at least two sites affected. In addition, one-third of patients had hemorrhage, including 18.8% with ICH.
“This spectrum of thrombotic and hemorrhagic events shows that TTS is not only limited to CVT, but can present with varying severity and locations,” the investigators note.
Treatment approaches varied, with two-thirds receiving heparin products. Nonheparin anticoagulants were used in 34.1%, and this was associated with a favorable outcome, supporting expert recommendations. Also common was use of steroids (31.7%) and IV immunoglobulin (43.9%). Surgery was required in 29.3%.
High Mortality in Early Cases
Overall mortality in this pooled analysis was high at 35.9%, which “may have been partially because these patients were among the initial reported cases of TTS, and many of them received heparin products—low-molecular-weight heparin or unfractionated heparin—in the early stages of presentation.”
The investigators assessed the utility of the FAPIC score to discriminate mortality risk, finding good performance in the initial development data set, as well as when it was internally validated (C-statistics 0.786 and 0.807) and externally validated among 16 patients who developed VITT after receipt of the Johnson & Johnson vaccine (C-statistic 0.771).
Connors said that the FAPIC score is likely to evolve as new data become available, noting that the largest published cohort of VITT, which came out last month, was not included in this study. Moreover, Hwang et al were unable to take treatment effects into account when creating the score.
Even so, the tool is useful for clinicians facing a patient with VITT, Connors said. “It can help people assess the patient in front of them and determine their likelihood of death and how concerned and aggressive they should be with treatment.”
Without the score, a patient in his or her 30s or 40s who presents with a pulmonary embolism or deep vein thrombosis and thrombocytopenia 10 days after receipt of an adenoviral-vector vaccine might be sent home on a direct oral anticoagulant, Connors said. But if the FAPIC score comes in at 3, which was associated with an expected mortality of about 45% in this study, “you might pay closer attention to that person who otherwise might seem well,” she said. “You might admit them, you might give them IV [immunoglobulin], you might be a little more aggressive than just giving a nonheparin anticoagulant.”
And for patients with a score of 5, physicians may decide to “pull out all the stops,” Connors added.
Addressing Vaccine Hesitancy
Hwang et al suggest that having a firmer grasp on the features of and outcomes with VITT could help overcome the problem of COVID-19 vaccine hesitancy.
“We expect that our report and the FAPIC score could be utilized to evaluate TTS patients according to clinical severity, further consolidate evidence regarding better or worse outcomes, and thus ameliorate the uncertainty that still prevails regarding TTS,” they say. “As evidence and experience regarding TTS are being accumulated, we expect this report to guide future management of TTS in mitigating the extremely high mortality rate in these cases, as well as inform the medical and lay community to help combat vaccine hesitancy.”
Connors said she hoped that would be the case, noting that initial reports of VITT indicated a mortality rate of around 40%. More-recent published data put the figure lower at about 18%, with some indications that VITT cases in Australia are associated with a mortality rate of just 6%, she said, citing communications with an expert in the field.
The declining mortality rate can be attributed to early recognition and effective treatment of the complication, Connors proposed. “If this scoring system can help clinicians recognize that the patient has VITT and apply the right therapies, then that is a huge step forward, and that should help decrease vaccine hesitancy because you know that if you do get this very rare disease it can be treated,” she said.
Todd Neale is the Associate News Editor for TCTMD and a Senior Medical Journalist. He got his start in journalism at …
Read Full BioSources
Hwang J, Park SH, Lee SW, et al. Predictors of mortality in thrombotic thrombocytopenia after adenoviral COVID-19 vaccination: the FAPIC score. Eur Heart J. 2021;Epub ahead of print.
Connors JM. Thromboinflammatory findings and clinical predictors of mortality in vaccine-induced immune thrombotic thrombocytopenia. Eur Heart J. 2021;Epub ahead of print.
Disclosures
- Hwang reports no relevant conflicts of interest.
- Connors reports having served on scientific advisory boards and consulted for Abbott, Alnylam, Anthos, Bristol-Myers Squibb, Five Prime Therapeutics, Pfizer, Portola, and Takeda, and receiving institutional research funding from the Patient-Centered Outcomes Research Institute, the National Heart, Lung, and Blood Institute, and CSL Behring.


Comments