Selection Bias? Debate Asks How Many TAVR Devices Centers Should Stock
Most interventionalists agree that operators should have access to at least two valves, but as a recent debate concluded, volume matters.
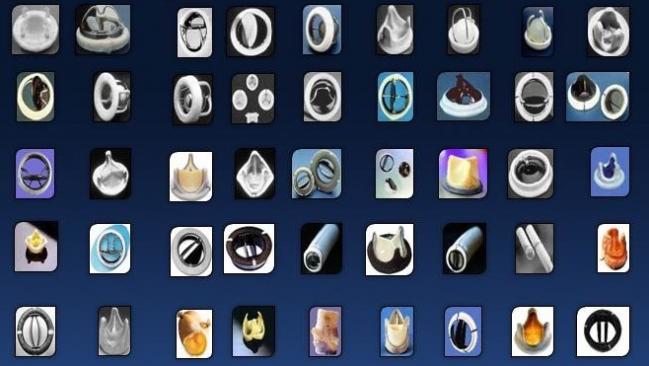
DENVER, CO—The success of TAVR has meant that operators have choices when it comes to the valves they implant, but as a debate at TCT 2017 highlighted, there are many reasons why cath labs may or may not want to limit their inventory options.
“One size doesn't fit all. It's a fact of life,” said Michael Reardon, MD (Houston Methodist Hospital, TX), who took the stance that ideally a range of devices should be available to TAVR operators at any given time. At a minimum, he argued, cath labs should stock one balloon-expanding valve, a self-expanding valve, and a mechanically-expanding valve, given that they “all deploy fundamentally differently and they all have fundamentally different characteristics. I may not need more than one of these at a time, but having these three valves of some sort covers the spectrum.”
For now, only the Sapien series of balloon-expandable valves (Edwards Lifesciences) and the CoreValve family of self-expanding valves (Medtronic) are approved for use in the United States, although a wider range of TAVR options are available in other markets.
But Haim Danenberg, MD (Hadassah Medical Center, Jerusalem, Israel), who took the counterpoint, showed side-by-side images of an Airbus and Boeing cockpit and quipped: there is “a reason why airline pilots don't fly different planes.” With “each and every valve,” he continued, there is a learning curve. “We have so many data now showing that we're paying for the learning curve in mortality, in major bleeding, and vascular complications. Wherever you start to train with the new valve, you have this learning curve.”
To make it simple for operators, he argued, “use no more than two valve systems.”
Reardon admitted that “there are just too many valves out there” after his online search resulted in more than 2,000 devices—both surgical and percutaneous, many of them still investigational or approved outside the United States—but he said he has reasons for choosing one valve over another for his patients: namely device access, patient anatomy and physiology, and delivery characteristics.
Difficulty with access, since devices are getting smaller, s becoming less of an issue, Reardon said. “At my shop right now we're 97% transfemoral, and all the rest of them are subclavian.” He used to also do a substantial number of procedures via the direct aortic approach, but this has since been abandoned. Similarly, Reardon added, how “trackable” a device is could play into whether an operator decides to use it depending on the curvature of the aorta in a specific case.
The biggest concern regarding patient anatomy would be calcification, he noted—do you put in a balloon-expandable valve and risk rupture, or go with a self-expanding valve and maybe leave some paravalvular leak? And with patient physiology, the physician needs to consider how tolerant the patient is, Reardon said. “There are some people with bad [right ventricles] that I don’t want to pace at all. I'd be afraid that they won't come back.”
As for delivery, “we all know that each of these valves behave differently and they deliver a slightly different way,” he argued.
Operator preference is the last parameter at play, Reardon said. “I may have four pericardial valves [used for surgical valve replacement], but I've had one that I like to use and I use it over and over again to get very good at it. When I move off that pericardial valve, it's for a reason and I have other choices.”
Dangerous Choice?
Danenberg said he understood the benefit of choice for TAVR operators, but argued that too much choice would be potentially dangerous for patients. After all, TAVR valves are not like coronary stents. “The valves differ in their delivery systems, and their periprocedural evaluation and deployment processes are definitely different,” he observed. “Complication management is different by all means, . . . and you need to learn and know [all of the procedural details for each valve] by heart in order to bring your results to perfection.”
Informally surveying 50 of his “experienced” colleagues with an average of 200 annual TAVR cases, Danenberg said that 48% of them are using more than two devices. About one-third said that TAVR centers should be using two or more devices, but about 60% said this should depend on case volume. When he delved more specifically into that question, all respondents said cath labs should not use more than two devices unless they do more than 100 cases annually, and 45% said that number should be 200 cases. Pulling data from the Society of Thoracic Surgeons/American College of Cardiology TVT Registry, Danenberg said the average case number per center is 78, “so most centers are not qualified to do more than two valves.”
As such, while “cardiovascular medicine gained a lot from fierce competition and multiplayer innovation, using more than two devices in all centers will not assure [a] good enough outcome,” he concluded. “Most TAVR centers should use one or two devices.”
A live poll of attendees in the session revealed that 45% thought that TAVR centers should have access to only two devices, while 14%, 36%, and 5% thought that each program should stock one, three, and four or more devices, respectively.
In a discussion after the debate, most of the experts gathered tended to agree with Danenberg. Panelist Albert Markus Kasel, MD (German Heart Center, Munich), said “you don’t need a lot on the shelf, but when you decide for more than one, then you need to have higher volume.”
Mohamed Abdel-Wahab, MD, PhD (Heart Center, Segeberger Klinkin, Bad Segeberg, Germany), agreed, noting, “It doesn’t make sense to have a lot of devices if you don’t have enough volume.”
Panelist Ganesh Manoharan, MBBCh, MD (Royal Victoria Hospital, Belfast, Northern Ireland), specified that hospitals should have access to a minimum of two devices. “And if you're going to do any more than two, you should be doing more than 100 cases,” he said.
With two valves, “you can treat 95% of the patients,” said panelist Luis Nombela-Franco, MD, PhD (Hospital Clinico Universario San Carlos, Madrid, Spain).
“Which means you need three,” countered panelist Torsten Vahl, MD (NewYork-Presbyterian/Columbia University Medical Center, New York, NY).
Photo Credit: Adapted from Reardon MJ. Point – a multi-device lesion-specific approach is preferred. Presented at: TCT 2017. November 1, 2017. Denver, CO
Yael L. Maxwell is Senior Medical Journalist for TCTMD and Section Editor of TCTMD's Fellows Forum. She served as the inaugural…
Read Full BioSources
Reardon MJ. Point – a multi-device lesion-specific approach is preferred. Presented at: TCT 2017. November 1, 2017. Denver, CO.
Danenberg H. Counterpoint – more than two TAVR devices on your shelf is unnecessary! Presented at: TCT 2017. November 1, 2017. Denver, CO.
Disclosures
- Reardon reports receiving consultant fees/honoraria from Medtronic.
- Danenberg reports receiving financial support from Medtronic.


Comments