Stark Drop in CV Imaging in Early COVID-19 Offers Food for Thought
A new study shines a light on regional and global differences in diagnostic testing, with some takeaways for the future.
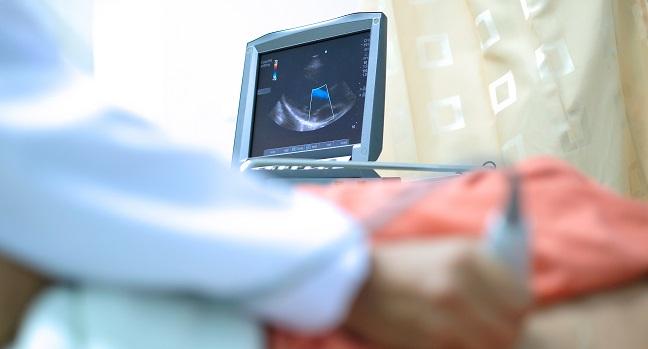
The number of diagnostic tests for cardiovascular disease in the United States fell by 68% in the first month of COVID-19 lockdowns, similar to the drop seen globally in the INCAPS-COVID registry. And while the sharp drop in cardiac admissions and procedures amid COVID-19 has been well documented, the new study shines a light on the decline in cardiovascular diagnostic tests and what this may portend for the future.
Earlier work by the same research group documented that volumes of cardiovascular imaging tests declined by 64% worldwide in the early phase of the COVID-19 pandemic—a number that’s now been exceeded by the US data reported this week. And the impact of that may be felt for many years, senior author Andrew J. Einstein, MD, PhD (Columbia University Irving Medical Center/NewYork-Presbyterian, New York, NY), told TCTMD.
“If these don't get made up, at a certain point, it's going to catch up with us in terms of cardiovascular outcomes,” Einstein said. “What we're seeing from outcome data, indeed, is that the death rate in the United States in 2020 was the highest it's ever been. That's not just from COVID, but also cardiovascular disease, cancer, and other leading causes of death without a full-blown working healthcare system. So patients suffer potentially on multiple fronts, which is something we need to be careful about and remediate insofar as possible.”
The study, led by Cole B. Hirschfeld, MD (Columbia University Irving Medical Center/NewYork-Presbyterian), was published this week in JACC: Cardiovascular Imaging.
Politics Didn’t Affect Drop-offs
In their analysis drawn from the INCAPS-COVID registry, combining data from 909 institutions in 108 countries, including 155 US centers, investigators looked at procedure volumes and related laboratory practices for all CV imaging tests performed in April 2020, using March 2019 as the comparator period. Tests included stress ECG; stress, transthoracic, and transesophageal echo; stress SPECT; stress PET; stress and nonstress CMR; coronary artery calcium scanning; coronary CTA; and invasive coronary angiography (ICA).
Hirschfeld et al report that test volumes in the US were similar to those in non-US facilities (68% vs 63%), with the exception of ICA, which saw greater declines in the US than elsewhere (69% vs 53%; P < 0.001). US declines also varied by region, with the greatest dips seen in the Northeast (76%) and the Midwest (74%), areas which also were more likely to include urban areas, which saw higher COVID-19 prevalence and more staff redeployments.
Interestingly, said Einstein, dropping test volumes did not track with politics. “One thing that frustrated me as a physician was the great politicization of COVID-19, but what we found was really no support for this, at least in terms of the implications for cardiovascular disease tests. Whether the governor of a state was Republican or Democrat was not significantly associated with cardiac procedure volume reduction. And whether it was a ‘red state’ or a ‘blue state’ was not significantly associated with procedure volume reduction in our multivariable analysis,” he said, adding that that serves as a reminder that COVID-19 had “serious consequences” for all Americans. “We're all in this boat together.”
The regional findings suggest not only that physicians in different states were not swayed by politicized interpretation of the science around COVID-19 severity, transmissibility, and the need for nonpharmaceutical interventions to curb the spread, but also that patients themselves likely had similar trepidations about hospital visits in the early months of the pandemic.
A Rise in Preventable CVD?
What that reduction in tests may mean down the road is unclear and something investigators are hoping to track through the registry. INCAPS-COVID 2 is already underway, attempting to gauge the extent to which CV imaging test volumes have recovered or helped to backfill tests missed earlier in the pandemic, and what the implications of that may be, said Einstein.
“I think it's highly likely that we'll find some bounce back, which is a good thing, but the area under the curve needs to stay the same, otherwise you're missing patients,” he said. “And even if that has bounced back to a hundred percent, you've got certain people who've missed their testing, so what are the long-term implications for those patients? One test for which we saw a huge drop-off, for example, in the United States was coronary artery calcium scoring, which is a useful risk stratification tool. So unless we made those up in the meantime, you may have patients who are not on statins and are at a higher risk of coronary disease.”
The pressing concern is that this gap in tests will lead to a higher rate of preventable cardiovascular events in the future. Moreover, the pandemic is still far from over in countries like India and Brazil, he noted, so any “bounce back” in those countries is likely a ways off.
There’s also the possibility that gaps in tests, for some patients, might not come with a price. “It's hard to tease things apart, but this is an opportunity. In the United States, probably more than most places in the world, there's a certain degree of inappropriate testing which occurs,” said Einstein, noting that different estimates suggest testing falls into the “rarely appropriate” category anywhere from 5% to 50% of the time. “So this is an opportunity to reconsider our practices and focus on what's most important in terms of cardiac testing,” he continued. “At the same time, one certainly doesn't want to throw away the baby of cardiac diagnostic testing with the bath water of inappropriate testing.”
There are still some cardiologists who send every patient for an echo and a nuclear stress test, Einstein pointed out. “And that’s certainly not necessary.” The field of imaging, he added, is moving “towards the right test, for the right patient, at the right time, using the right technique.”
Delaying calcium scoring by 6 months or a year because of COVID-19 so that a patient could stay safe at home, “was probably a good thing,” he said. “But at the same time, your patients with chest pain, who weren't getting stress tests, weren't getting a cath—that’s a lost opportunity and the human and economic costs are potentially staggering.”
What Tests Can We Get Rid of Permanently?
Commenting on the study for TCTMD, David Brown, MD (Washington University School of Medicine, St. Louis, MO), pointed out that to get a true sense of the impact on CV outcomes from any dip in testing would need a multipronged approach. “You’d have to have hospital records, but also coroner records, and EMS records to try and get an idea of the totality of cardiovascular mortality, pre- and post-COVID, and then look at the correlation between that and the testing.”
Much of the work that has been done so far, he noted, has been done with any eye to how to be better prepared for the next pandemic, or what kind of tests can be delayed. “My concern is obviously what can we get rid of permanently, without doing any harm, and cutting down on costs and these cascades of care that lead to bad outcomes.”
But if showing causality—or a lack of impact—from reduced or delayed tests and cardiovascular outcomes may be fraught, there remains the possibility that some cardiologists who’ve relied heavily on tests in the past may be slightly less inclined to do so post-pandemic if they see a minimal impact on their patients. Brown acknowledged that he himself, after transitioning out of interventional cardiology, took some time to realize how well patients were doing on medical therapy.
It’s possible that some cardiologists may emerge from the COVID-19 pandemic realizing that they can cut back on imaging referrals, said Brown, but he expressed skepticism that this would happen across the board, most notably for private practices that rely on on-site imaging as a revenue stream.
Shelley Wood was the Editor-in-Chief of TCTMD and the Editorial Director at the Cardiovascular Research Foundation (CRF) from October 2015…
Read Full BioSources
Hirschfeld CB, Shaw LJ, Williams MC, et al. Impact of COVID-19 on cardiovascular testing in the United States versus the rest of the world: the INCAPS-COVID study. J Am Coll Cardiol Img. 2021;Epub ahead of print.
Thompson RC, Lehenbauer KR. The cardiovascular imaging community’s response to the COVID-19 pandemic. J Am Coll Cardiol Img. 2021;Epub ahead of print.
Disclosures
- Einstein reports previously receiving grants from the National Institutes of Health, the International Atomic Energy Agency, Canon Medical Systems, Roche Medical Systems, WL Gore, and GE Healthcare; serving as a consultant for WL Gore; being on the speakers bureau for Ionetix; having received travel/ accommodations/meeting expenses from HeartFlow; and being a stockholder in Emergent BioSolutions Inc.
- Brown and the editorialists report no relevant conflicts of interest.



Comments