Subcutaneous ICD Has Favorable Outcomes in Older Patients
The data are “reassuring that this is a reasonable alternative even in the older patient population,” one researcher says.
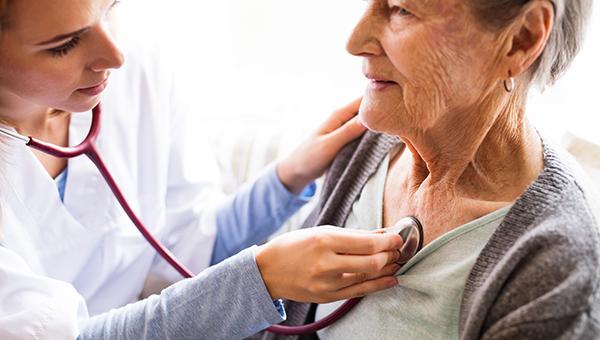
For older patients without an indication for pacing, the subcutaneous implantable cardioverter-defibrillator (S-ICD; Boston Scientific) provides results comparable to those seen with traditional single-chamber, transvenous devices through the first few years of follow-up, a registry study indicates.
There were no significant differences by ICD type in death, device reoperation, device removal for infection, or cardiovascular or all-cause readmission among fee-for-service Medicare beneficiaries included in the National Cardiovascular Data Registry ICD Registry, according to researchers led by Daniel Friedman, MD (Duke University Hospital, Durham, NC).
The results, published in the March 22, 2022, issue of the Journal of the American College of Cardiology, are reassuring, Friedman said. It was thought that older patients getting an S-ICD, compared with their younger counterparts, might be more likely to develop a need for pacing—which can’t be handled by the subcutaneous device—and thus might have a higher rate of reoperation to implant a transvenous system. But that wasn’t seen here.
“Among patients who are 65 years or older who are candidates for the subcutaneous ICD, midterm clinical outcomes are equivalent whether those patients receive a single-chamber, transvenous ICD or a subcutaneous ICD. There is no hint of a difference in outcomes,” Friedman told TCTMD. “And so, in that setting, the decision can be made based on personal preferences and based on shared decision-making between the patient, their family, and the physician.”
According to Pier Lambiase, MD, PhD (Cleveland Clinic London, England), who was not involved in the study, “having data about the [subcutaneous] ICD demonstrating you can have good outcomes in these patients, at least equivalent to transvenous ICD, is a positive step to lower the threshold to make the device more accessible for these older patients.”
Limited Evidence for Older Patients
Though the S-ICD has been established as an important alternative to transvenous devices, Friedman said, prior studies—including the randomized PRAETORIAN trial and the single-arm UNTOUCHED study—have focused on younger patients, at least in part because of the greater need for backup pacing that comes with age. In addition, younger patients potentially have a long life expectancy and have more to gain from not having implanted transvenous leads and their associated complications.
Evidence of S-ICD outcomes in older cohorts “is a real important need because there are differences in the need for backup pacing as well as differences in the likelihood of developing atrial fibrillation, which is important to diagnose and can be an important cause of inappropriate shocks,” Friedman explained.
To help fill that gap, the investigators examined data from the National Cardiovascular Data Registry ICD Registry on 16,603 patients (mean age 72.6 years; 28.4% women) who received an ICD between September 28, 2012, and December 31, 2017, had no indication for pacing, and survived to discharge. Overall, 6.2% of patients had an S-ICD implanted.
Compared with patients who received a transvenous ICD, those who received an S-ICD were younger on average, more likely to be Black and on dialysis, and less likely to have a history of atrial fibrillation/flutter.
After accounting for those differences with propensity-score matching, there were no differences in clinical outcomes between the S-ICD and transvenous ICD groups through a median follow-up of 2.3 years:
- All-cause mortality (HR 1.02; 95% CI 0.82-1.27)
- Device reoperation (subdistribution HR 0.98; 95% CI 0.65-1.48)
- Device removal for infection (subdistribution HR 0.61; 95% CI 0.14-2.74)
- Device reoperation without infection (subdistribution HR 0.98; 95% CI 0.63-1.51)
- CV readmission (subdistribution HR 1.09; 95% CI 0.91-1.30)
- Recurrent all-cause readmission (HR 1.07; 95% CI 0.99-1.16)
The results are reassuring, but there remains a need for longer-term follow-up, Friedman said, noting that the need for pacing increases over time and that battery life is shorter with the S-ICD than with transvenous devices (roughly 6 versus 10 years). Thus, S-ICD recipients will need a subsequent procedure sooner than will those who get a transvenous device. What happens around the time of the generator replacement is a key question, Friedman said.
Lambiase agreed that several years of follow-up are needed to truly assess differences between the S-ICD and other devices when it comes to conversion to pacing and outcomes like all-cause mortality, adding that issues related to transvenous leads with standard devices—like infections—won’t emerge until patients are followed for a longer period of time.
Choosing a Device
The main consideration when choosing between the S-ICD and a transvenous device, particularly in older patients, is the anticipated need for backup pacing in the future, Friedman said. Physicians can scrutinize the preimplant ECG for signals suggestive of a greater risk of eventually requiring pacing, “but our ability to predict these things is imperfect at best,” he added.
One of the factors standing in the way of the S-ICD’s early adoption was the greater risk of inappropriate shocks, the investigators note, and a limitation of the current analysis is that information on inappropriate shocks—which can affect quality of life and harder outcomes—was not available.
That “would have been very informative given the high burden of atrial arrhythmias,” Lambiase commented. He added, however, that “the lack of difference in hospital admissions at least suggests no major adverse outcomes with multiple inappropriate shocks by S-ICD.”
Lambiase noted that there could be a concern about device erosion/infection being more common in older patients, although in this study, there were no differences in reoperation and infection rates by device type. That’s reassuring, he said, considering the higher proportion of patients on dialysis in the S-ICD group and the high burden of diabetes overall.
Over the past 2 or 3 years, S-ICD implantation has been growing in the older age groups as the technology has become more accepted and operators have grown used to implanting the device, Lambiase said. Because older patients have higher rates of diabetes and renal impairment—which increase susceptibility to infections—“if you don’t need to put transvenous leads in and there’s no pacing indication, then this is a good population to offer the S-ICD to,” he said.
In an accompanying editorial, Ahmadreza Karimianpour, DO, and Michael Gold, MD, PhD (both Medical University of South Carolina, Charleston), note that prior studies have indicated that age does not influence outcomes with the S-ICD, a concept also supported by the current analysis.
“These important results support and extend previous studies suggesting that the age bias in S-ICD use in not warranted with contemporary ICD devices and programming,” they write. “So, hopefully we can treat older patients with a new trick of avoiding transvenous leads while still protecting from sudden cardiac death in the absence of pacing indications.”
Todd Neale is the Associate News Editor for TCTMD and a Senior Medical Journalist. He got his start in journalism at …
Read Full BioSources
Friedman DJ, Qin L, Parzynski C, et al. Longitudinal outcomes of subcutaneous or transvenous implantable cardioverter-defibrillators in older patients. J Am Coll Cardiol. 2022;79:1050-1059.
Karimianpour A, Gold MR. Can we treat an older patients with a new trick? J Am Coll Cardiol. 2022;79:1060-1062.
Disclosures
- The study was supported by the American College of Cardiology’s National Cardiovascular Data Registry (NCDR). The ICD Registry is an initiative of the American College of Cardiology with partnering support from the Heart Rhythm Society.
- Friedman reports no relevant conflicts of interest.
- Karimianpour reports having received extramural travel funding for educational programs from Boston Scientific.
- Gold reports having received honoraria and research grants from Boston Scientific.


Comments