Therapeutic-Dose Heparin in COVID-19: Who Benefits, Who Doesn’t
Results of the REMAP-CAP, ACTIV-4a, and ATTACC multiplatform trial should “immediately” impact global care, one author says.
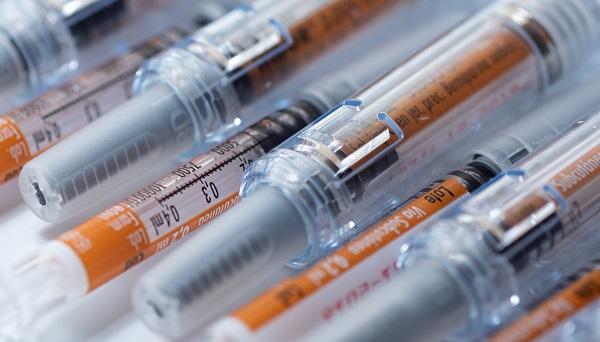
Therapeutic-dose heparin appears to benefit noncritically-ill COVID-19 patients, but it does not reduce deaths or other adverse endpoints compared with usual-care thromboprophylaxis if it’s initiated once patients are critically ill and requiring ICU-level care. Those dual findings from a large, global collaboration—first announced in preliminary form in late 2020 and early 2021, as reported by TCTMD—have now been published as separate papers in the New England Journal of Medicine.
The multiplatform trial findings represent the combined efforts of three randomized clinical trials across four continents—REMAP-CAP, ACTIV-4a, and ATTACC, which joined forces early on to align their protocols and data collection while creating a central site for endpoint adjudication. The collaboration aimed to swiftly understand the role of therapeutic-dose heparin in these two distinct patient groups as COVID-19 hospitalizations climbed.
Taken together, the findings confirm that therapeutic-dose anticoagulation using heparin is superior to standard thromboprophylaxis for improving survival with reduced need for organ support in the non-ICU patients, but is an inferior strategy in the ICU patients.
“I think this will immediately change practice around the world,” Ryan Zarychanski, MD (University of Manitoba, Winnipeg, Canada), told TCTMD, stressing that the results were seen across multiple different health settings, across all three trials, and repeated over time. “This is a pretty robust result, and we expect it to resonate widely and immediately.”
He continued: “There have been several therapies developed—and remdesivir is one of them—where health systems were reticent to adopt a therapy that was expensive, for which the treatment effects were uncertain in hospitalized patients. But for the most part heparin is a familiar drug, it’s very inexpensive, it's stocked in all hospitals around the world, and it's affordable in any health region, whether that’s in the United States or in Nepal.”
Heparin, he added, is known not only as an anticoagulant but also for its anti-inflammatory properties as well as potentially some antiviral effects; this might help explain why this agent showed benefit in non-ICU level patients, whereas others, including direct oral anticoagulants (DOACs), have not. Therapeutic-dose rivaroxaban in the ACTION trial, for example, failed to show a benefit in hospitalized patients.
“I don't consider that contradictory,” Zarychanski said. DOACs are “thrombin inhibitors, totally oral, and they don't have the same anti-inflammatory effects as heparin. And it's quite possible that this is just not an anticoagulant effect—this is a heparin effect.”
On the other hand, studies of enoxaparin and fondaparinux, which are indirect inhibitors of factor Xa that don’t inhibit thrombin, have pointed to similar benefits, Zarychanski noted. The smaller RAPID trial of therapeutic- versus prophylactic-dose heparin improved survival, although it did not significantly reduce rates of a composite primary outcome, according to preprint results. Results from the large, three-way FREEDOM COVID-19 trial randomizing patients to full-dose enoxaparin, prophylactic enoxaparin, or the DOAC apixaban will also bring clarity. The trial has enrolled roughly 2,700 out of an intended 3,600 participants and is expected to finish enrollment in the next 3 months.
Commenting on the new papers for TCTMD, Behnood Bikdeli, MD (Brigham and Women’s Hospital, Boston, MA, and Yale University School of Medicine, New Haven, CT), joint principal investigator for the INSPIRATION study, characterized the results in the critically-ill patients as definitive. “For over a year and a half we’ve being talking about an excess risk of blood clots [in COVID-19], but even if that's the case, heparins do not seem to be the answer in the ICU,” he noted. “I think by now that has become fairly definitive and clear, and kudos to the trialists for confirming this message.”
In the noncritically-ill patients, however, “here is where the situation, in my humble opinion, is more fluid and dynamic,” Bikdeli said.
Key Results
As previously reported by TCTMD, both arms of the REMAP-CAP, ACTIV-4a, and ATTACC multiplatform trial were stopped early after meeting criteria for futility in the case of critically-ill patients and for the superiority of therapeutic heparin (mostly low molecular weight) in the noncritically-ill arm.
In the latter group, 2,219 patients were included in the final analysis after the trial was stopped. In all, 80.2% of patients in the therapeutic-dose group, as compared with 76.4% the standard-prophylaxis group, reached the primary outcome of organ-support-free days, evaluated on an ordinal scale that combined in-hospital death and the number of days free from cardiovascular or respiratory organ support up to day 21 among patients who survived to hospital discharge. That amounted to a mean adjusted difference in risk of 4.0 percentage points (adjusted OR 1.27; 95% credible interval 1.03-1.58).
Zarychanski stressed to TCTMD that this gap is clinically meaningful, both for the patients battling COVID-19 and for health systems more broadly. “What that means is for every thousand patients admitted to hospital, 40 get discharged alive without the need for ICU level care. It's a benefit to patients but also a benefit to the system, because most health systems in COVID pandemics run out of ICU beds, they run out of critical-care support. From a patient perspective, this has clinical benefit with low risk, but from a health systems perspective this also reduces the burden [in the] ICU by approximately 25%.”
Superiority of the therapeutic dose was also seen for a range of other endpoints including survival to hospital discharge, survival without organ support, progression to intubation or death, and major thrombotic event or death. Major bleeding, however, was twice as common in the therapeutic-dose group (1.9% vs 0.9%).
I think this will immediately change practice around the world. Ryan Zarychanski
In an analysis broken down by D-dimer, patients with higher levels at the time of randomization had a higher probability of therapeutic dose anticoagulation being superior to usual care (97.3%) than those with lower levels (92.9%), though the probably of superiority also was seen among patients randomized to therapeutic heparin in whom D-dimer levels were unknown.
At the study outset, said Zarychanski, investigators had hypothesized that D-dimer levels might help identify best responders to therapeutic heparin, but this didn’t pan out. “Whether you add a low D-dimer or a high D-dimer, or your D-dimer was missing, you derive relatively the same treatment benefit from the protocol in moderately ill patients. The absolute treatment benefit was higher in people with high D-dimer because the event rate was higher, but the relative treatment effects—that is, the odds ratios—were very similar between the D-dimer groups. So there's no real benefit to measuring D-dimer.”
Importantly, major bleeding was nearly doubled in the therapeutic anticoagulation group.
That bleeding risk is something that will have to be discussed in conversations with patients, Bikdeli observed, and the decision to escalate heparin dose will also need to take into account other issues not fleshed out in the primary trial results, he cautioned.
For one, he continued, “the trial was not powered for, nor did it prove a reduction in, all-cause mortality. Second, as the investigators appropriately mention, the comparator was a mixed bag of what they call ‘usual care.’ The good news is, it's practical, but the challenge is that usual care could vary. So I would love to see additional analyses to see if the benefit of the treatment effect was different according to the intensity of the anticoagulation [in the comparator group].
Use of steroids also is important, he noted, as are what effect their use might have had on the results. Just over 60% of the patients in the noncritically-ill arm of the trial were treated with steroids, he noted, and analyses will have to dig into whether steroid use interacted with the full-dose heparin effects.
Critically-Ill Patients
A total of 1,098 patients in the critically-ill group had been randomized by the time the trial was stopped for futility: 534 to therapeutic-dose heparin and 564 to usual-care thromboprophylaxis. Median organ-support-free days, evaluated on an ordinal scale that included in-hospital death (assigned a value of -1) in the therapeutic-dose group was 1, compared with 4 in the patients assigned to usual care, a nonsignificant difference. There were no differences in the percentage of patients who survived to hospital discharge between the therapeutic and prophylactic groups (62.7% vs 64.5%; OR 0.84; 95% credible interval 0.64-1.11). Again, major bleeding was higher in the therapeutic-dose group than in the usual-thromboprophylaxis group: 3.8% vs 2.3%.
Asked why heparin would be beneficial in noncritically-ill patients but not those requiring organ support, Zarychanski was cautious, noting that speculation was what led investigators to assume heparin would potentially be lifesaving for patients needing ICU-level care. “We had initially thought that critically-ill patients would stand to gain the most benefit,” he said, “but that wasn't the case.”
If he had to hypothesize, he continued, “perhaps it is that the severity of illness is too great to be overcome by the modest, moderate, and beneficial effects of heparin—patients are too sick to benefit from a drug that has modest anti-inflammatory effects but established antithrombotic effects. Maybe there's too much microthrombosis already; maybe there's too much macrothrombosis already. Or maybe the inflammation cascade is already set in motion, and that is in existence in those who are severely ill and can't be readily modified by heparin at that point.”
In an accompanying editorial, Hugo ten Cate, PhD (Maastricht University Medical Center, the Netherlands), had a similar hypothesis: that the thrombotic and inflammatory damage that has already occurred among critically-ill patients cannot be influenced by higher-dose heparin. There’s also the possibility, however, that the makeup of the populations played a role. Whereas the “vast majority” of critically-ill patients were recruited at centers involved in REMAP-CAP, in the United Kingdom, the bulk of the moderate-disease patients were recruited in ATTACC and ACTIV-4a in the US and Brazil. There may also be “caveats related to the noncurrent nature of the control group,” he writes, “in which experimental groups entered and exited the trial at different times,” not to mention differences in the type of standard thromboprophylaxis used at different sites—a point also raised by Bikdeli.
The theory that drug timing and sickness severity are critical is one that has been raised in the past, and it may be the most compelling. Other agents, Zarychanski pointed out, have also proven to have different and unexpected benefits—or lack of benefit—depending on the timing of initiation. Steroids, for example, seem to work best in patients requiring supplemental oxygen, but not in less severe illness. Tocilizumab (Actemra/RoActemra; Roche) appears to work best in critically-ill patients, whereas both remdesivir (Veklury; Gilead) and convalescent plasma seem to have an edge in patients who are not yet severely ill.
Indelible Impact?
In addition to stressing what he believes could be an immediate effect on global patient care in COVID-19, Zarychanski sees other ways in which this multiplatform trial will leave an “indelible mark” on science. One, he said, is the notion of using heparin earlier in the course of sepsis—a trial studying heparin in sepsis ironically was what Zarychanski was in the midst of doing when COVID-19 halted enrollment, leaving him well positioned to apply the same protocol to patients battling SARS-CoV-2. The other impact, he predicted, will be on swift, collaborative research “using multiplatform trials as a model of global collaboration, to tackle important questions, not only in the pandemic and interpandemic period. . . . I think that this kind of trial will set a precedent for future trials.”
Zarychanski is also hopeful that his heparin RCT in sepsis, sidelined during the pandemic, will be up and running again full speed in the near future.
There are at least 75 clinical trials registered on ClinicalTrials.gov addressing antithrombotic strategies in COVID-19, with the majority focused on heparin or low-molecular-weight heparin, says ten Cate. But many open questions remain including whether other antithrombotic agents “or even profibrinolytic strategies” may be beneficial in critically-ill patients, in whom therapeutic heparin doses have come up short. And while the multiplatform trial published today shows “signals of benefit” for heparin in noncritically-ill patients, physicians will still wrestle with the “lack of insight into mechanisms” and the difficulty of juggling bleeding risks with benefits, ten Cate adds.
Bikdeli noted that if he had a patient hospitalized with COVID-19, full-dose heparin is certainly a strategy he would consider discussing based on the results of these trial results, because “it’s an interesting and impressive signal.” But he will also be looking closely at studies still ongoing and hopes a subsequent meta-analysis of heparin trials “will help us get some definitive answers,” an analysis he says the World Health Organization has already said it supports.
Shelley Wood was the Editor-in-Chief of TCTMD and the Editorial Director at the Cardiovascular Research Foundation (CRF) from October 2015…
Read Full BioSources
The REMAP-CAP, ACTIV-4a, and ATTACC investigators. Therapeutic anticoagulation with heparin in critically ill patients with COVID-19. N Engl J Med. 2021;Epub ahead of print.
The ATTACC, ACTIV-4a, and REMAP-CAP investigators. Therapeutic anticoagulation with heparin in noncritically ill patients with COVID-19. N Engl J Med. 2021;Epub ahead of print.
ten Cate H. Surviving COVID-19 with heparin? N Engl J Med. 2021;Epub ahead of print.
Disclosures
- Zarychanski reports no relevant disclosures.
- Bikdeli reports no relevant disclosures.
- Ten Cate reports consulting for Alveron and Stago; holding shares in Coagulation Profile; receiving advisory board fees from Portola/Alexia, and serving on the advisory board for CARIM; receiving research contracts with CARIM/PPS Health Holland and Bayer, as well as research support from Pfizer.



Comments