‘These Are Good Organs’: Drug Overdose Deaths Boost Transplants, With Few Downsides
It’s an unexpected upside to the opioid epidemic: transplants after overdose deaths fare similarly to non-high-risk hearts.
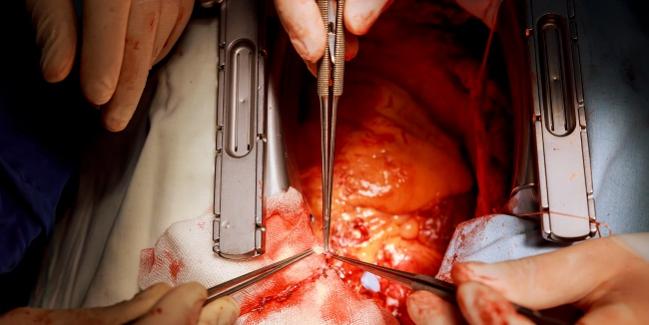
The tragedy of the opioid epidemic has brought with it an increasing number of donor hearts available for transplantation in the United States, and these organs appear to perform just as well as others for recipients, new data show.
Across the country, the proportion of transplants involving overdose-death donors rose from 1.1% in 2000 to 6.0% in 2012, after which the increase accelerated, bringing that figure to 14.2% in 2017. In 2018, the proportion topped 25% in many states, including Delaware, where half of heart transplants involved organs obtained from people who had died of overdose.
Though these organs were more likely to come from people infected with hepatitis C, patients who received the hearts had posttransplantation stroke and survival rates similar to those who received organs from other types of donors.
“These are good organs and they should be used for transplantation and anyone who receives an offer [for a heart] from one of these types of donors, they need to think hard . . . before rejecting it because it’s a ‘high-risk’ donor,” senior author Nader Moazami, MD (NYU Langone Health, New York, NY), told TCTMD.
The study, with lead author Katherine Phillips, BS (NYU Langone Health), was published online June 6, 2019, ahead of print in the Annals of Thoracic Surgery.
Moazami said it has been known for several years within the transplant community that more donor organs have been made available by the opioid epidemic, and indeed other studies have also tried to quantify the impact on transplantations. Up until 3 or 4 years ago, he said, data from the United Network for Organ Sharing (UNOS) showed that 2,100 to 2,200 heart transplants were being done each year. Since then, however, there have been another 300 to 400 a year, coinciding with the spike in deaths due to opioid use. “There’s amazing altruism and generosity on the part of either the donors or the families for donating these organs,” he said.
Moazami said he and his colleagues wanted to delve deeper into how the surge of overdose deaths has impacted the transplant community and learn more about the characteristics of hearts obtained from these types of donors, both those that were used and those that were discarded. They examined data from the Scientific Registry of Transplant Recipients on 15,904 cardiac transplantations performed in adults between January 1, 2010, and June 1, 2017. Overall, 10.8% involved overdose-death donors.
Compared with other donors, those who died of drug overdose were more frequently younger than 40 and white, with higher rates of cocaine use, hepatitis C positivity, cardiac arrest, receipt of CPR, and an LVEF below 50%.
Recipients of hearts from overdose-death donors had higher rates of support from extracorporeal membrane oxygenation or an intra-aortic balloon pump before transplantation, but after the operation, had a rate of stroke similar to those who received organs from other types of donors (2.3% vs 2.7%; P = 0.373). There were no differences between groups in terms of posttransplantation hospital length of stay (median 15 days in both groups; P =0.950) or overall survival (P = 0.066). Recipients of overdose-death donor hearts had less need for hemodialysis after surgery (9.6% vs 11.9%; P = 0.008).
Citing the comparable outcomes, Moazami said “there’s really a potential pool that can be expanded for many patients who are waiting on the transplant list and are at risk of dying.” He added that he has no specific concerns with using hearts from people who have died of drug overdose as long as they are of good quality, similar to the consideration for any donor organ.
All of these types of hearts will be automatically labeled as high-risk, he noted. “The only implication for that is that I need to have a thorough conversation with the recipient that this heart is coming from a donor that has ‘XYZ’ characteristics and therefore is high-risk,” Moazami said. “So we get a separate consent from the recipient because they’re the ones who actually have to make the decision. But from a physician perspective, I usually believe that . . . we should be using them all the time.” In his experience, nearly all patients have agreed to accept such an organ.
Commenting for TCTMD, heart-lung transplant surgeon Robert S.D. Higgins, MD (Johns Hopkins Hospital, Baltimore, MD), said the opioid epidemic has had a tangible impact on the available of donor organs, not just for cardiac transplantation but for lung, liver, and kidney transplantation as well.
“One of the things that I think has changed has been the level of comfort [that has developed so] that people would be willing to accept an organ that historically was not optimal to save their life,” said Higgins, who is the current president of the Society of Thoracic Surgeons and a former president of UNOS.
Higgins observed that, in his experience hearts from overdose-death donors have performed very well, noting, “They don’t tend to have any structural problems. It appears that they may, in fact, have a higher incidence of hepatitis C, and so we have to be mindful about that. We still need to have an informed-consent process that says that patients would be willing to accept organs from these donors because they are unique.”
This new study, Higgins said, “raises the specter that maybe this is a donor pool that should be accepted without reservation going forward because the overall survival and outcomes are equivalent, certainly not worse. . . . It requires further study and careful assessment going forward, so that we can maybe fine-tune the criteria that we use to say a heart is no good because it has a potential risk to [instead] say maybe we can include it in the donor pool and save lives.”
Todd Neale is the Associate News Editor for TCTMD and a Senior Medical Journalist. He got his start in journalism at …
Read Full BioSources
Phillips KG, Ranganath NK, Malas J, et al. Impact of the opioid epidemic on heart transplantation: donor characteristics and organ discard. Ann Thorac Surg. 2019;Epub ahead of print.
Disclosures
- Phillips and Moazami report no relevant conflicts of interest.


Comments