True Myocarditis Uncommon in COVID-19, Review Concludes
A roundup of published autopsy data and a comparison of tissue samples provide some reassurance for clinicians.
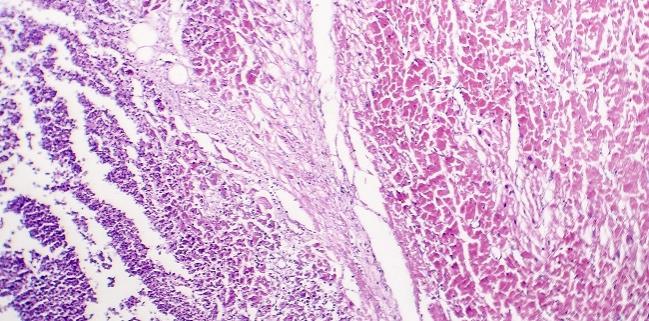
Among patients with COVID-19, the incidence of myocarditis is less than 5%, according to a review paper that looked at evidence from tissue taken either at autopsy or endomyocardial biopsy.
Coronavirus-related myocarditis has been a topic of concern over the last year, beginning with small postmortem reports from Wuhan, China, of fulminant myocarditis in some patients, followed by publication of a controversial cardiac magnetic resonance (CMR) study suggesting that more than three-quarters of middle-age adults—some with mild or no symptoms—had ongoing cardiac involvement weeks or even months after recovering from COVID-19. There also was some evidence even among young adults, with a small analysis of 26 college competitive athletes who’d tested positive for the virus showing that four had CMR imaging evidence of myocarditis and eight had signs of prior myocardial injury.

The new review focused on the pathology data, noted senior author Aloke V. Finn, MD (CVPath Institute, Gaithersburg, MD), because they are important to understanding the true incidence of myocarditis in this population. Many of the early reports were based on clinical data, not tissue samples, which are needed to make the diagnosis. Alongside the literature review, Finn and colleagues, led by Rika Kawakami, MD (CVPath Institute), also examined 15 hearts they obtained from Italy that came from patients who died of COVID-19.
Finn said the bottom line for clinicians is that the bulk of the existing evidence they reviewed is reassuring.
“What we can conclude is that in the histological examination, we just don't find [myocarditis] very commonly,” he added. “That’s supported by our own data of the hearts we examined. They didn’t have any evidence of myocarditis.”
Focus on Autopsies
In the months following the creep of the COVID-19 pandemic across Europe, small autopsy studies began to emerge in publications and on preprint servers. Two important ones came from Germany. The first focused mainly on the pulmonary effects of the virus. The second found that 61.5% of autopsies conducted on patients who died in April 2020 had SARS-CoV-2 RNA in myocardium on reverse transcriptase-polymerase chain reaction (PCR) testing, hinting at direct viral infection of the heart. However, none of those cases met criteria for myocarditis.
More recently, a small autopsy study that included 21 patients from Italy, the United States, and the Netherlands reported high rates of macrophage infiltration in cardiac tissue. In terms of multifocal lymphocytic myocarditis, however, only three of these 21 cases were identified on rigorous histopathologic examination.
Those reports and 16 others were the focus of the review. Among the collective published literature consisting of 201 autopsied hearts or endomyocardial biopsy tissue, there was “some evidence of myocarditis of unclear extent and nature” in 4.5%, the researchers conclude. They caution that in most cases, “analysis for the virus in the heart was not performed and evidence for direct infection of cardiac myocytes has not been shown.” An important caveat, however, is the possibility of false-negative results, which could be caused by sampling errors of tissue or by degradation of viral RNA during the process of fixation prior to analysis.
In the separate analysis of the 15 hearts that was performed by Kawakami et al, they found that while none met the myocarditis criteria, three samples showed “evidence of either microvascular or epicardial thrombosis in the setting of acute myocardial infarction, and these cases all had neutrophilic infiltration.” Additionally, inflammatory cell infiltration in the epicardium was noted in 10 of 16 cases (63%), and consisted primarily of lymphocytes, while myocardial mononuclear inflammatory cell infiltration was present in five of 16 (31%), they write. All samples had RNA extracted from myocardial tissue, which was measured for quality and concentration, and quantitative reverse transcriptase PCR was performed using specifically designed primers for SARS-CoV-2.
“In only two cases was the virus detected in the heart by PCR and both were in the atria (one left atrium and one right atrium) and not in the ventricles, and neither was accompanied by inflammation, although in most of the 16 cases the virus was detected in the lung,” the researchers note.
Kawakami and colleagues also compared inflammatory cells found in the myocardium of COVID-19 patients with those of samples from their own registry, taken from patients who did not die of COVID-19 (controls). There was no difference in the total number of T cells or macrophages between the groups. The researchers also compared the COVID-19 inflammatory cells with samples from mild myocarditis of non-SARS-COV-2 origin from their own biobank. The COVID-19 samples showed more macrophages than T cells and no evidence of necrotic myocytes, while the myocarditis sample had more T cells than macrophages and significant necrotic myocytes.
Confronting a Valid Concern
The review also discusses whether endomyocardial biopsy is appropriate for suspected myocarditis in COVID-19 patients. Given the potential risks of the procedure, including cardiac perforation, pericardial tamponade, and bleeding, as well as the small percentage of confirmed myocarditis in the published literature, the investigators suggest that biopsy be reserved “for worst case scenarios, such as patients with new-onset fulminant heart failure with hemodynamic compromise in the setting of documented COVID-19 infection, and the absence of coronary artery disease.”
To TCTMD, Finn said the evidence suggests that the incidence of myocarditis with the current virus is actually less than was seen among the limited autopsies done during the first SARS-CoV outbreaks in the early 2000s.
“Maybe the disease manifest differently in young persons, as we know the systemic inflammatory response in kids has been seen. That remains an open question,” Finn added.
L.A. McKeown is a Senior Medical Journalist for TCTMD, the Section Editor of CV Team Forum, and Senior Medical…
Read Full BioSources
Kawakami R, Sakamoto A, Kawai K, et al. Pathological evidence for SARS-CoV-2 as a cause of myocarditis. J Am Coll Cardiol. 2021;77:314-325.
Disclosures
- The study was supported by the CVPath Institute.
- Finn has received honoraria from Abbott Vascular, Biosensors, Boston Scientific, Celonova, Cook Medical, CSI, Lutonix Bard, Sinomed, and Terumo; and has served as a consultant to Amgen, Abbott Vascular, Boston Scientific, Celonova, Cook Medical, Lutonix Bard, and Sinomed.




Comments