In Vaccine Era, Deaths Drop Sharply in STEMI Patients With COVID-19
STEMI outcomes have largely normalized for vaccinated patients, but the unvaccinated face risks compounded by COVID-19 symptoms.
WASHINGTON, DC—The profile of STEMI patients with COVID-19 evolved over the first 2 years of the pandemic, data from the North American COVID-19 Myocardial Infarction (NACMI) registry show. Between 2020 and 2021, in-hospital deaths decreased by a relative 25%, in large part due to the availability of COVID vaccines.
Prior reports from the NACMI have shown both good news and bad: STEMI care didn’t suffer, even early in the pandemic, but mortality rates were soberingly high.
Santiago Garcia, MD (Minneapolis Heart Institute, MN, and The Christ Hospital, Cincinnati, OH), presented the latest findings today at the American College of Cardiology 2022 Scientific Session, with the results simultaneously published in the Journal of the American College of Cardiology.
“Despite increased number of COVID-19 cases worldwide, significant progress has been made in both disease prevention and management during the course of the pandemic, which has contributed to a marked reduction in mortality in selected countries,” Garcia and colleagues write.
Garcia told TCTMD that despite going into the study knowing that the pandemic itself was changing, as well as STEMI outcomes, it was a surprise to see such a big improvement in survival. They timed the cut points of their analysis to capture the effects of COVID-19 vaccines becoming commercially available in early 2021. When it comes to mortality that year, Garcia said, “it looks like there are two groups of patients: those that are vaccinated and those that are unvaccinated.”
Thanks, Vaccines
For this paper, the researchers analyzed data on 586 patients with STEMI who’d tested positive for COVID-19 during or within 4 weeks before their index STEMI hospitalization. Among them, 227 were treated in 2020 and 359 in 2021.
Compared with 2020 patients, those presenting in 2021 were more likely to be Caucasian (58% vs 39%; P < 0.001) and to present with typical ischemic symptoms (59% vs 51%; P = 0.04). They were less likely to present with dyspnea (42% vs 56%; P = 0.002), have pulmonary manifestations (33% vs 47%; P = 0.001), and show infiltrates on chest X-ray (33% vs 47%; P = 0.001). The 2021 patients also showed a trend toward less shock before PCI (13% vs 18%; P = 0.07) compared with the 2020 group.
Invasive angiography was used more often in 2021 than 2020 (86% vs 77%; P = 0.004). More than 70% of patients underwent PCI, with no difference between years. Among those undergoing primary PCI, median door-to-balloon time was similar at 78 minutes in 2020 and 70 minutes in 2021, and a similar proportion of patients had times < 90 minutes in each year.
Hospital stays were shorter in 2021 than 2020 (median 5 vs 7 days; P = 0.01), as were ICU stays (median 2 vs 4 days; P < 0.001).
In-hospital mortality dropped from 33% in 2020 to 23% in 2021 (P = 0.008), which equated to 25% lower on multivariate analysis. For patients with infiltrates, mortality was increased by a relative 70%, and the risk of dying was nearly three times higher for patients with cardiogenic shock. Death risk also was increased, by 80%, for patients aged at least 66 years. There was a trend toward less stroke, as well, but no difference in reinfarction over time.
When NACMI began, COVID-19 vaccines were a hope, but not a reality. Gradually, participating centers have begun tracking vaccination status. This information was available for 193 (54%) of those treated in 2021. Just 22 of these patients, 11%, were vaccinated (median time from COVID shot to STEMI of 20 days). They were less likely than unvaccinated patients to have respiratory symptoms or infiltrates. None of them died in the hospital. That same year, the in-hospital death rate was 22% for unvaccinated patients (P = 0.009).
For the nearly 800 COVID-negative patients in the NACMI registry, mortality was similar in both years at approximately 10% to 11%.
“Taken together, our observations suggest that the clinical profile, management, and outcomes of STEMI patients with COVID-19 infection is evolving towards that of STEMI patients prior to the pandemic, although mortality remains high for unvaccinated patients,” the researchers conclude.
Garcia told TCTMD that as the data on vaccine status roll in from participating centers, even in states where 75% of people have had their COVID-19 shots, the vaccinated remain in the minority of patients hospitalized. This is “because the people coming to the hospital [are largely] the unvaccinated,” he explained, “so there’s a strong bias every time you look at hospitalized [patients].”
Vaccine uptake stagnated after vaccination became such a political issue, Garcia said, but “I hope we can convince more patients with these data to get vaccinated.” Importantly, he noted, their study “provides a mechanistic link” for why STEMI patients vaccinated against SARS-CoV-2 infection are more likely to survive.
Garcia said the reasons for the decreasing mortality are “multifactorial.” Some relate to the patient demographics. The racial/ethnic minorities hit hardest by COVID-19 in 2020 may have had less access to healthcare, for instance. He also cited the reduction in cardiogenic shock.
“Pulmonary involvement is the big one,” he stressed, pointing out that these factors—such as being intubated or on mechanical ventilation—were important predictors of death in NACMI’s previously developed risk score. “So I think eliminating that from the equation with vaccines has made a huge difference,” said Garcia.
By 2021, STEMI care has mostly returned to normal, at least for the vaccinated, he observed. “For unvaccinated patients, there are still some stuck in 2020.”
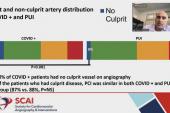
Garcia said the NACMI investigators have also done a gender-based analysis that they expect to present at SCAI 2022, and will continue gathering data into 2022, which will reveal shifts related to the Omicron variant. They also are developing an angiographic core lab, “because one in five patients undergoing angiography have no culprit vessel,” suggesting their condition relates to microthrombi, he said. They’re also working on an ECG core lab.
Caitlin E. Cox is Executive Editor of TCTMD and Associate Director, Editorial Content at the Cardiovascular Research Foundation. She produces the…
Read Full BioSources
Garcia S, Dehghani P, Stanberry L, et al. Trends in clinical characteristics, management strategies and outcomes of STEMI patients with COVID-19. J Am Coll Cardiol. 2022;Epub ahead of print.
Disclosures
- Garcia reports institutional research grants from Edwards Lifesciences, BSCI, Medtronic, and Abbott Vascular; serving as a consultant to the ACC, Medtronic, and BSCI; and being a proctor for Edwards Lifesciences.



Comments