BP Reductions Last 5 Years After Bariatric Surgery: GATEWAY
Just under 50% of those treated surgically were taking no antihypertensives, all while maintaining good BP control.
Bariatric surgery provides effective and durable treatment for high blood pressure in patients with severe obesity, long-term follow-up of the GATEWAY study shows.
Five years after Roux-en-Y gastric bypass, more than 80% of patients were able to cut down on the number of antihypertensive medications and still maintain blood pressures of less than 140/90 mm Hg, report investigators. In contrast, less than one in seven of the patients randomized to medical therapy alone were able to cut their use of BP-lowering drugs.
The chance of complete remission of hypertension—using no antihypertensive medications while maintaining healthy blood pressure—was roughly 20 times greater if patients were treated with surgery.
“Hypertension is related to obesity in many, many patients,” lead researcher Carlos A. Schiavon, MD, PhD (Hospital do Coracão, São Paulo, Brazil), told TCTMD. “One important thing is that obesity drives many patients to have resistant hypertension, which is a more dangerous disease.” Bariatric surgery, he said, is a very good treatment option for these patients, particularly those with severe obesity. He added that in general there is some degree of therapeutic inertia when it comes to hypertension, but focusing only on blood pressure or other risk factors is not enough when caring for patients with obesity.
“We must treat obesity when we are dealing with patients with cardiovascular disease or metabolic disease who have obesity as the base of the problem,” said Schiavon.
“When we think about the impact of bariatric surgery, in particular, not only do we think about the sizable weight loss, but the first comorbidity we typically look at are improvements in markers in type 2 diabetes,” said Sarwer. “While those results are impressive, the results related to hypertension are equally as impressive, as we see in this study. The results replicate findings from other, larger investigations from around the world as well.”
That’s an important consideration, he added, because the percentage of people with diabetes around the world, particularly in westernized countries, is still relatively low, but the percentage of those with hypertension, or who are on an antihypertensive medication, is high. Sarwer, who is involved in research investigating clinical inertia when dealing with hypertension, said the early results with bariatric surgery—weight loss and improvements in cardiometabolic risk factors, including hypertension—have been shown to be quite good and these latest results confirm its long-term efficacy.
“What may get lost in the shuffle is that as people continue to age, as they maybe become a little less active with age, and as they move further away from the date of surgery, it could be that their blood pressure actually gets a little less attention and could, in fact, start to creep up again,” he said. “To see the rates of remission and improvement stay as robust as they are in this study is really encouraging.”
To see the rates of remission and improvement stay as robust as they are in this study is really encouraging. David Sarwer
Philip Schauer, MD (Pennington Biomedical Research Center/Louisiana State University, Baton Rouge), said GATEWAY is the first randomized trial to focus exclusively on hypertension-related outcomes as a primary endpoint. The 5-year results, he added, are extremely important because they show the durability of bariatric surgery beyond that first year or two when there is significant weight loss.
“The effect is well sustained in terms of improving blood pressure control,” he said. “I think one of the key findings in this study was that surgery was very effective for those with resistant hypertension. It basically resolved the problem whereas with medical therapy, there was still a significant number of people who were on three drugs or more that were still not at their target diastolic and systolic blood pressure.”
Schauer, who led the STAMPEDE trial of bariatric surgery in obese patients with uncontrolled type 2 diabetes, saw a similarly durable benefit in that study. He noted that the 5-year results showed surgery was significantly better than medical therapy alone for decreasing hyperglycemia.
Targeting Obesity to Maintain Healthy BP
The obesity epidemic is a widely documented phenomenon, and there is ample evidence that excess weight and visceral fat are major causes of hypertension. Diet and exercise remain the cornerstone of obesity treatment, but the long-term management of obesity-related hypertension is challenging, as Schiavon pointed out. The American Heart Association recommends diet and exercise as first-line treatments, but also acknowledge that some patients will require medications or surgery in conjunction with continued lifestyle changes.
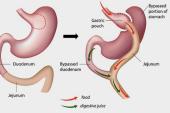
Originally published in 2017, the GATEWAY study included 100 obese subjects (mean body mass index [BMI] 36.9 kg/m2) with hypertension who were taking at least two antihypertensive medications. They were randomized to laparoscopic Roux-en-Y gastric bypass or medical therapy to determine the effect of surgery on obesity-related hypertension.
As reported by TCTMD, the 1-year primary outcome—defined as a 30% reduction in the use of antihypertensive medication (ie, a decrease in one or more drugs in those taking two or three medications, or at least two drugs in those taking four medications) while maintaining blood pressure targets of less than 140/90 mm Hg—was superior in those randomized to bariatric surgery compared with those on medical therapy alone. The benefits of surgery were maintained at 3 years.
At 5 years, 74% of those randomized to surgery and 64% of those on medical therapy were available for follow-up. Of the 69 patients (mean age 44.5 years; 76.8% female) available for analysis, baseline characteristics were mostly balanced, although there were some differences in the presence of comorbid conditions, such as dyslipidemia, diabetes, and family history of CAD. The median number of antihypertensive medications at baseline was three in both groups.
In total, 80.7% of patients in the bariatric group reduced their antihypertensive medication use by 30%, compared with 13.7% of patients randomized to medical therapy (P < 0.001). The mean number of antihypertensive medications taken was 0.8 in the surgery group versus 2.97 in the medical therapy group (P < 0.001). Despite taking fewer medications, there was no significant difference in 24-hour ambulatory systolic and diastolic blood pressures and no difference in daytime and nighttime blood pressure. The 5-year between-group difference in systolic blood pressure was -7.48 mm Hg favoring surgery (P = 0.045).
We must treat obesity when we are dealing with patients with cardiovascular disease or metabolic disease who have obesity as the base of the problem. Carlos Schiavon
Additionally, results showed that 46.9% of those randomized to gastric surgery were taking no antihypertensive medications at 5 years, compared with just 2.4% in the medical therapy group. On the other end of the spectrum, 10% and 28% of those in the surgical and medical-therapy groups still had uncontrolled hypertension.
In a post hoc analysis focused on the lower target in the US hypertension guidelines, 54.7% and 9.0% of those in the surgery and medical-therapy arms, respectively, achieved blood pressures of less than 130/80 mm Hg (P < 0.001). In all, 40% of those treated with surgery got to this target without medications, compared with 2.2% in the medical-therapy group.
Additionally, mean BMI declined from 37.35 to 28.01 kg/m2 and body weight from 101.95 to 76.35 kg in the surgical arm from baseline to 5 years, with no significant change in the medical therapy arm.
Stacking Up Against Medications
To TCTMD, Schiavon said the COVID-19 pandemic affected their ability to track all the patients through 5 years, but that despite the loss to follow-up the results remain robust. “To have almost 47% remission after 5 years, and patients are taking less medications, I think is a very good result,” he said.
In an editorial accompanying the study, Michael E. Hall, MD (University of Mississippi Medical Center, Jackson), and colleagues emphasize that long-term control of body weight is important for maintaining healthy blood pressures. Despite this, patient nonadherence and physician inertia remain major factors to poor blood pressure control, noting that resistant hypertension is also a major driver of other cardiometabolic disorders.
“People with obesity often require challenging and costly treatments for diabetes, dyslipidemia, and other comorbidities in addition to hypertension,” they write. “Bariatric surgery is effective at reducing all of these obesity-associated disorders while decreasing blood pressure and major adverse cardiovascular events.”
They point out that obesity is thought to raise blood pressure via multiple neurohormonal and renal mechanisms, but it’s not known if bariatric surgery reduces blood pressure by reversing these mechanisms or through decreased caloric intake and reduced adiposity. Schiavon noted that tirzepatide (Mounjaro/Zepbound; Eli Lilly), a glucagon-like peptide 1 (GLP-1) receptor agonist, was also shown to reduce 24-hour ambulatory blood pressure in the SURMOUNT-1 study, published just this week in Hypertension.
Schauer, a metabolic surgeon, said that sleeve gastrectomy has become the more dominant surgical procedure in some parts of the world, including the US. However, based on some of the latest national numbers, the utilization of gastric bypass is again beginning to increase. In STAMPEDE, surgeons used both sleeve gastrectomy and gastric bypass, with gastric bypass resulting in greater weight loss. To date, there has not been a study focused exclusively on hypertension outcomes with the sleeve gastrectomy procedure, he said.
Reducing hypertension and obesity . . . is very likely to have a very beneficial effect on long-term cardiovascular morbidity and mortality. Philip Schauer
To TCTMD, Sarwer noted that while the GATEWAY trial was small and there was loss to follow-up, it’s very difficult to execute a clinical trial where patients are randomized to a surgical intervention.
Obesity treatment is undergoing a revolution with the introduction of medications to drastically induce weight loss, with one trial showing that the GLP-1 receptor agonist semaglutide (Wegovy; Novo Nordisk) reduces the risk of major adverse cardiovascular events in patients who are overweight or have obesity. With their popularity exploding, Sarwer noted, the drugs can be hard to access and remain expensive for some patients.
“There’s also some discussion in the United States that some private insurance companies are taking another look at the onerous preoperative requirements to bariatric surgery,” said Sarwer. “They’re beginning to think about pulling some of those back to make it easier for patients to have surgery. In some ways, it's going to be very interesting in the next 3 to 5 years to see how this change in the landscape, with the enthusiasm around these new medications, impacts both pharmacotherapy and also bariatric surgery.”
Schiavon said the new drugs are excellent for weight loss, but that they remain a challenge to get and pay for in many countries with public health systems, like Brazil, Canada, and elsewhere. “And the big challenge is to maintain this [weight loss],” said Schiavon. “For those with more severe obesity, bariatric is very good.”
Schauer noted that complications with surgery are very low, and the procedure is as safe as having your gall bladder out. “Reducing hypertension and obesity, two of the major risk factors, is very likely to have a very beneficial effect on long-term cardiovascular morbidity and mortality,” he said.
Michael O’Riordan is the Managing Editor for TCTMD. He completed his undergraduate degrees at Queen’s University in Kingston, ON, and…
Read Full BioSources
Schiavon CA, Cavalcanti AB, Oliveira JD, et al. Randomized trial of effect of bariatric surgery on blood pressure after 5 years. J Am Coll Cardiol. 2024;83:637-648.
Hall ME, Mace HP, Hall JE. Bariatric surgery for obesity hypertension: a gateway for durable blood pressure control. J Am Coll Cardiol. 2024;83:649-651.
Disclosures
- Schiavon reports a research grant from Ethicon and lecture fees from Ethicon and Medtronic.
- Hall reports no relevant conflicts of interest.
- Sarwer reports grant funding from the National Institutes of Health. He reports consulting for Novo Nordisk and Twenty30 Health.



Comments