CABG Bests PCI for 5-Year Survival in Biggest Analysis Yet, With Options for Left Main Disease
The results reinforce the need for surgeons and cardiologists to collaborate for a disease where heart team decisions have become “ad hoc,” experts say.
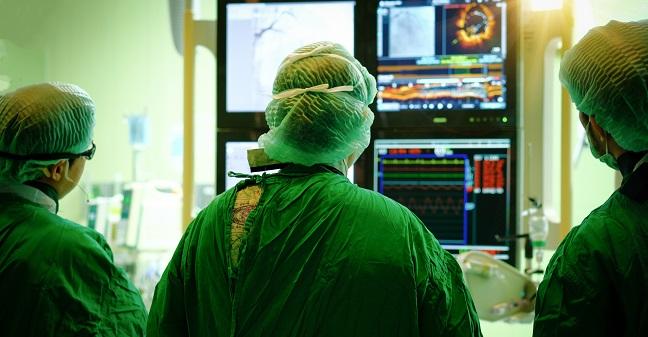
A large pooled analysis of randomized data is providing some much-needed long-term mortality numbers in the long-running CABG versus PCI debate. The data show that while CABG holds a long-term survival benefit over PCI in patients with both multivessel disease and diabetes, both revascularization strategies appear appropriate for patients with left main disease.
“There have been a lot of randomized trials comparing bypass surgery and percutaneous coronary intervention, and most of them have included between 500 and up to 2,000 patients, but that is still a little bit too small to actually detect big differences between the two revascularization strategies in terms of mortality,” lead study author Stuart J. Head, MD (Erasmus University Medical Center, Rotterdam, the Netherlands), told TCTMD.
For this analysis, published online February 22, 2018, ahead of print in the Lancet, the researchers compiled patient-level data from 11,518 individuals enrolled in 11 randomized trials comparing CABG and PCI between 1995 and 2015. The mean SYNTAX score was 26.0.
Overall, 976 patients died over a mean follow-up of 3.8 years. Five-year all-cause mortality was higher in those treated with PCI compared with CABG (11.2% vs 9.2%; HR 1.20; 95% CI 1.06-1.37). A time-dependent model showed no difference in risk between the two revascularization strategies before 1 year, but CABG was favored beyond the 1-year mark.
Notably, among the 3,051 patients who received bare-metal stents, there was no difference in 5-year all-cause mortality between PCI and CABG (8.7% vs 8.2%; HR 1.05; 95% CI 0.82-1.34). Type of stent used, however (bare metal versus DES), did not interfere with the overall findings (P for interaction = 0.53).
The mortality difference between PCI and CABG was also seen regardless of whether patients received first- versus newer-generation DES.
For patients with diabetes, PCI was associated with a higher risk of all-cause mortality at 5 years compared with CABG (15.7% vs 10.7%; HR 1.44; 95% CI 1.20-1.74). This relationship was also seen among patients with multivessel disease where the 5-year all-cause mortality was 11.5% for PCI and 8.9% for CABG (HR 1.28; 95% CI 1.09-1.49); it was even stronger for patients with both diabetes and multivessel disease (15.5% vs 10.0%; HR 1.48; 95% CI 1.19-1.84). However, there was no mortality difference between PCI and CABG for nondiabetic patients with multivessel disease.
Surprisingly, for patients with left main disease—a common reason why patients are sent for CABG—there was no difference in mortality at 5 years between PCI and CABG (10.7% vs 10.5%; HR 1.05; 95% CI 0.87-1.33).
Clear Answers With Pooled Data
While Head said the overall results weren’t unexpected since previous research had hinted that survival rates are better overall with CABG over PCI, having definitive evidence now is satisfying. However, among the subgroups, he said he was surprised to see no difference in mortality for the cohort of patients with left main disease, especially given that there were “some patients with higher SYNTAX scores that were included in that population as well. That's something that didn't come out of the SYNTAX trial.”
This reinforces the importance of large analyses like this one to the body of evidence, Head noted. In a study of 1,000 patients, “to actually find some significant differences in [subgroups] can be tricky because you don't have enough patients and you never know whether it's an effect of chance or what is actually occurring,” he said. On the other hand, “if you have big data like this, then it obviously becomes more powerful to detect those differences.”
Study co-author Gregg W. Stone, MD (Columbia University Medical Center, New York), agreed. “A large patient population is required to detect differences in a low frequency safety endpoint such as mortality with high confidence,” he told TCTMD in an email. “Having the individual patient data is critical to afford analysis in important subgroups, such as those with and without diabetes, and according to SYNTAX score.”
While it “was a lot of work for everyone involved” to include the original patient-level data from each of the 11 trials, Head said it was worthwhile. Data sharing enables researchers to “answer questions that we've never been able to answer,” he added.
This study “demonstrates clearly that long-term survival is improved with surgery compared to PCI in patients with multivessel disease and diabetes,” Stone summarized. “PCI may be considered an acceptable or even preferred alternative to CABG in patients with multivessel disease without diabetes, and in most patients with left main disease regardless of diabetes. However, CABG would be preferred in providing a long-term survival benefit in most patients with multivessel disease and diabetes.”
By Head’s estimation, there is a global “tendency to have patients undergo CABG if there is more complex disease,” and these findings support that practice. “What [this study] really confirms is that as soon as you have more coronary artery disease, then CABG is better—so multivessel disease and especially then in those with diabetes.”
The subgroup findings will likely influence the new European revascularization guidelines expected later this year, he added.
Remaining Challenges
Commenting on the study for TCTMD, Sandeep Nathan, MD, MSc (University of Chicago, IL), said the pooled data is “very important” for several reasons. First, obviously, is size. “Without burning through an exorbitant amount of funding, it would be almost impossible to do the appropriately sized single randomized controlled trial evaluating survival” following CABG versus PCI, he said.
Also, “it gives us a more complete understanding of the interaction terms that are involved even when a heart team is assessing patients for candidacy for one revascularization strategy versus the other,” Nathan added. “The theme that runs through this paper is that multivessel disease and diabetes are big drivers of adverse events, in this case mortality.”
The challenge with this analysis, however, is that it is unknown whether the “right” lesions were revascularized, he said. “In labs such as ours where we use a lot of functional testing—FFR, iFR, CFR—as well as intravascular imaging, you're consistently surprised, and the one thing that is consistent is that we're not that good at predicting functional severity simply looking at the angiogram within that gray zone.”
The theme that runs through this paper is that multivessel disease and diabetes are big drivers of adverse events, in this case mortality. Sandeep Nathan
Also, Nathan questioned the amount of residual unrevascularized disease left among the patients in this study and how that may affect mortality outcomes. “We know from the original SYNTAX publication and some of the secondary publications that a PCI-based strategy is more likely to leave unrevascularized territories on the table,” he explained. “And we know that whether you break it up by tertiles of residual SYNTAX score or residual SYNTAX score ≥ 8, adverse events are driven up. So if the likelihood of complete revascularization is greater with bypass surgery, you wonder whether it's an apples-to-apples comparison when we're talking about multivessel disease or whether the totality of disease was even correctly identified at the outset and targeted for revascularization.”
Additionally, given that diabetes appears to interact substantially with outcomes, “this makes you wonder whether there is residual disease within that vessel, not the lesion per se, but lots of disease that either is obstructive at the time of revascularization or is likely to become obstructive in the near future,” Nathan added. “In diabetic patients where characteristically disease is diffuse, perhaps treating the vessel as opposed to just treating the lesion that is obstructed at the time of angiography bears dividends in the 1-to-5-year haul, which is when these curves start to splay out.”
Patient Preference and Collaboration
Given that the mean age of the patients in this study was about 65 years, 5 years of follow-up is “still relatively short,” Head said. “We really need to have [even] longer follow up to find whether these differences are actually still occurring at 10 years . . . between the two revascularization strategies.”
Ten-year follow-up results from the SYNTAX trial are planned to be presented at TCT 2018 in September, he said.
What is also unknown is the degree to which patient preference plays into decision-making patterns. While the risk of mortality between PCI and CABG is significant, the difference may seem small to a patient, and “of course mortality is not the only outcome—you also need to look at stroke, myocardial infarction, and repeat revascularization,” Head said. “What comes out of this is that it's also very important to sit with the heart team and discuss what we think is best, but also discuss this with the patient. . . . There are obviously some times when it's a big debate between cardiologists and surgeons, and I'm a surgeon, but in the end, it's what's best for the patient. If you can do PCI with similar results of CABG, then it's definitely something to consider over CABG.”
Asked whether the heart team concept is used enough for coronary interventions, Nathan said, “it's often a bit of an ad hoc exercise and not uniformly applied.” Teamwork has “become the norm in structural and valvular interventions and has really attained a level of formality that's well established in most institutions,” he added, but “we could always use more collaborative decision making in clinical medicine.”
There are obviously some times when it's a big debate between cardiologists and surgeons, and I'm a surgeon, but in the end, it's what's best for the patient. Stuart J. Head
For his part, Stone said he would like to see future studies designed “to determine why CABG provides a survival benefit in patients with multivessel disease and diabetes compared with PCI. For example, is this related to incomplete revascularization or inadequate adherence to guideline-directed medical therapy? Or is it inherent to bypassing greater vulnerable segments of the coronary tree in the diabetic patients?” Additionally, he said, studies should address whether other factors like stable CAD versus ACS; use of second- versus first-generation DES; and patient age, sex, and frailty “may affect the relative outcomes of the two procedures.”
Looking forward, Head said that “PCI is improving every day—the techniques, the stents, etcetera. So I'm curious to see whether, in the future, the results will be different from what we have now, and undoubtedly the results with PCI are going to improve. I guess also as a message for the surgeons, we have to keep improving our technique to be able to continue providing good results that are either better or equal to PCI. It's going to be an interesting next 10 years.”
Note: Study co-author Gregg W. Stone, MD, is a faculty member of the Cardiovascular Research Foundation, the publisher of TCTMD.
Yael L. Maxwell is Senior Medical Journalist for TCTMD and Section Editor of TCTMD's Fellows Forum. She served as the inaugural…
Read Full BioSources
Head SJ, Milojevic M, Daemen J, et al. Mortality after coronary artery bypass grafting versus percutaneous coronary intervention with stenting for coronary artery disease: a pooled analysis of individual patient data. Lancet. 2018;Epub ahead of print.
Disclosures
- Head, Stone, and Nathan report no relevant conflicts of interest.


Comments