COVID Vaccine Thrombosis, Thrombocytopenia Risks Clarified in International Study
The study comparing adenoviral and mRNA vaccines confirms the complications are “extremely rare,” Hyung Chun says.
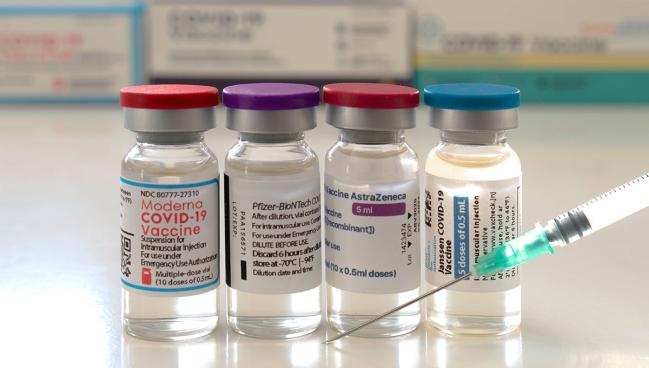
In this series, the vaccines primarily diverged around the risk of thrombocytopenia alone, which was significantly higher after a first dose of the adenovirus-based Oxford/AstraZeneca shot than after a first dose of the mRNA-based Pfizer/BioNTech vaccine, consistent with prior studies. The absolute risk difference was 8.21 cases per 100,000 recipients.
But when it came to the risk of TTS, a combination of clotting and low blood platelets, it was rare and did not differ significantly in any of the vaccine comparisons.
“However, this finding should be put in context with previous research, because some of our estimates were close to significance, suggesting a potential increased risk of venous thromboembolism with thrombocytopenia syndrome after vaccination with [the adenovirus-based Janssen vaccine from Johnson & Johnson],” lead author Xintong Li, MHS (University of Oxford, England), and colleagues write in a study published online this week in the BMJ.
Overall, they say, “although rare, the observed risks after adenovirus-based vaccines should be considered when planning further immunization campaigns and future vaccine development.”
Commenting for TCTMD, Hyung Chun, MD (Yale University, New Haven, CT), said the results confirm, with a larger sample size, what has been seen in prior studies—that thrombosis and thrombocytopenia are “extremely rare” after COVID-19 vaccination.
In the early waves of the pandemic, risks of these complications were much higher with COVID-19 itself than what was subsequently seen after vaccination, he noted. He added that even though more-recent variants of SARS-CoV-2—like Omicron and its offshoots—are associated with lower risks of thrombocytopenia and thrombosis than earlier ones, “the risk of severe illness with COVID-19 certainly does seem to be higher than what you would expect with the vaccines themselves.”
Overall, Chun said his message around COVID-19 vaccination hasn’t changed: “The vaccinations do offer safe protection from severe illness from COVID-19. There is a very small risk of potential adverse events, but this study doesn’t tell me that the risk is higher than what had been known before and it does show that the vaccines currently in use in the US . . . do continue to demonstrate robust safety.”
Reports of patients developing acute thrombosis accompanied by thrombocytopenia after receipt of the Oxford/AstraZeneca vaccine started coming out in the months after the shots were introduced. Similar reports followed the rollout of the Johnson & Johnson vaccine, highlighting a risk primarily with the adenovirus-based products, but there’s some evidence that the complication can develop after receipt of mRNA-based shots from Moderna and Pfizer/BioNTech as well.
“While the pathogenesis is not yet fully understood, an immune response leading to the development of pathological platelet-activating antibodies has been suggested and named as vaccine-induced immune thrombotic thrombocytopenia [VITT],” Li et al write. “Although these events are very rare, absolute numbers of affected patients could become substantial owing to the large numbers of vaccine doses administered worldwide.”
I think there is sufficient evidence that there is this small risk of potential adverse events. So if the vaccine manufacturers can potentially improve upon this, certainly that is something that should be actively pursued. Hyung Chun
More than two and a half years into the pandemic, a relevant question is whether the risk of TTS, or VITT, differs among the available vaccines.
The investigators addressed that issue by examining routinely collected health data from five European countries (France, Germany, the Netherlands, Spain, and the United Kingdom) and the United States. Overall, there was information available on 4.6 million people who received a first dose of Oxford/AstraZeneca vaccine (with a second dose in 1.6 million) between December 2020 and the middle of 2021; 1.1 million who received the single-dose Johnson & Johnson vaccine; 10.6 million who received a first dose of Pfizer/BioNTech vaccine (with a second dose in 7.7 million); and 4.3 million who received a first dose of Moderna vaccine (with a second dose in 2.9 million).
After applying propensity-score adjustment and other statistical methods to improve the robustness of the results, the investigators focused on the most-rigorous comparisons of vaccine risks within the first 28 days after administration.
When it came to the risk of thrombocytopenia alone, a first dose of Oxford-AstraZeneca vaccine was associated with more events compared with a first dose of Pfizer/BioNTech vaccine, with a pooled calibrated incidence rate ratio (IRR) of 1.33 (95% CI 1.18-1.50). Risk didn’t differ when comparing recipients of second doses of those vaccines or when comparing the Johnson & Johnson shot with a first dose of Pfizer/BioNTech vaccine.
Among the comparisons robust enough for meta-analysis, the only other significant difference observed was in the risk of intestinal infarction, which was lower with the Johnson & Johnson vaccine than with a first dose of Pfizer/BioNTech vaccine (calibrated IRR 0.37; 95% CI 0.15-0.89).
Risks of various venous and arterial thrombotic events, as well as TTS, did not differ significantly in those comparisons, although there were nonsignificant trends toward less arterial thromboembolism when comparing first doses of Oxford/AstraZeneca vaccine with the Pfizer/BioNTech shot (calibrated IRR 0.87; 95% CI 0.75-1.01) and toward more cases of TTS stemming from deep vein thrombosis (calibrated IRR 1.83; 95% CI 0.62-5.38) and venous thromboembolism (IRR 2.26; 95% CI 0.93-5.52) when comparing the Johnson & Johnson shot with the Pfizer/BioNTech vaccine.
The hints of differences observed in the main analyses and across subgroups require additional research, the investigators say.
The study is subject to several potential limitations, including possible misclassification of vaccine use and outcomes, unmeasured confounding, variation in the timing of when vaccines became available and to whom they were first made available, and limited power for the analysis of TTS risk, Li et al point out.
But there are important strengths as well, they say. “While other epidemiological methods have been used in vaccine safety studies, a cohort study with active comparators enabled us to directly estimate the relative risk of developing thromboembolic events or [TTS] after different COVID-19 vaccines, which is not feasible in self-controlled designs or in observed to expected analyses,” they write. “Our study therefore answers a more-reliable question at this stage of the pandemic (ie, ‘which vaccine is safer’ rather than ‘are vaccines safer than no vaccination’).”
Chun agreed with the investigators that these findings should be taken into consideration when making future decisions about immunization campaigns or next-generation vaccine development.
The vaccines are already quite safe, he added, but said, “I think there is sufficient evidence that there is this small risk of potential adverse events. So if the vaccine manufacturers can potentially improve upon this, certainly that is something that should be actively pursued as we continue to deal with the pandemic in its various stages.”
Todd Neale is the Associate News Editor for TCTMD and a Senior Medical Journalist. He got his start in journalism at …
Read Full BioSources
Li X, Burn E, Duarte-Salles T, Yin C, et al. Comparative risk of thrombosis with thrombocytopenia syndrome or thromboembolic events associated with different COVID-19 vaccines: international network cohort study from five European countries and the US. BMJ. 2022;379:e071594.
Disclosures
- The study was funded by the European Medicines Agency.
- Li reports support from the Clarendon Fund and Brasenose College scholarship (University of Oxford) to support her DPhil study.
- Chun reports working with a healthcare investment firm that is not associated with any of the vaccine manufacturers.



Comments