October 2021 News Roundup
This month features dialysis patients in need of TAVI, aspirin in COVID-19, virtual reality in cardiac care, and more.

Every month, Section Editor L.A. McKeown curates a roundup of recent news tidbits from journals and medical meetings around the globe.
Disagreements over whether and how to revascularize are common between members of heart teams, particularly in cases of patients with complex CAD. A study in the European Heart Journal: Quality of Care & Clinical Outcomes explores factors that influence decision-making and provides recommendations to improve organization and agreement among team members.
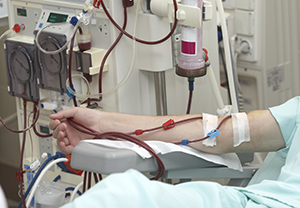 Patients on dialysis who require aortic valve replacement present a significant treatment challenge. A case report published in Structural Heart describes a successful TAVI outcome in a patient with severe symptomatic aortic stenosis and severe nephropathy.
Patients on dialysis who require aortic valve replacement present a significant treatment challenge. A case report published in Structural Heart describes a successful TAVI outcome in a patient with severe symptomatic aortic stenosis and severe nephropathy.
Outpatient management of both pulmonary embolism and deep vein thrombosis has been increasing in recent years and is associated with lower rates of healthcare utilization and major bleeding compared with inpatient management, a study published in the Journal of the American Heart Association concludes. The researchers attribute the shift to outpatient care to availability of direct oral anticoagulants (DOACs) and improved clinical ability to identification low‐risk patients.
The Journal of Cardiac Failure presents an interesting dual perspective on the realities of HF: that of a young patient learning about his illness and treatment, as well as that of the physician who was part of his care team.
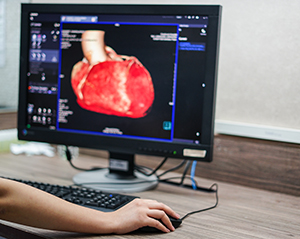 A small study of patients recovering from COVID-19 who underwent MRI or CT coronary angiography found no evidence of left ventricular dysfunction or excess persistent myocardial injury compared with comorbidity-matched volunteers. “These patients have a high prevalence of cardiovascular comorbidity that may account for much of the reported myocardial abnormalities on cardiac magnetic resonance,” the researchers write in Heart. “However, some patients recovering from COVID-19 did have evidence of mild persistent right ventricular dysfunction that likely reflects recovery from a severe life-threatening respiratory viral illness.”
A small study of patients recovering from COVID-19 who underwent MRI or CT coronary angiography found no evidence of left ventricular dysfunction or excess persistent myocardial injury compared with comorbidity-matched volunteers. “These patients have a high prevalence of cardiovascular comorbidity that may account for much of the reported myocardial abnormalities on cardiac magnetic resonance,” the researchers write in Heart. “However, some patients recovering from COVID-19 did have evidence of mild persistent right ventricular dysfunction that likely reflects recovery from a severe life-threatening respiratory viral illness.”
A meta-analysis of 17 studies finds that while TAVI is feasible in selected patients with bicuspid anatomy, these individuals are at greater risk of moderate to severe paravalvular leak, annular rupture, and cerebral ischemic events compared with tricuspid patients, investigators report in JACC: Cardiovascular Interventions.
Patients who were on aspirin therapy prior to a hospital admission for COVID-19 were less likely to die or require mechanical ventilation than those who were not, according to the ASA-CARE study of 984 Italian patients. While considered hypothesis-generating and unlikely to change standard of care, it confirms data from a much smaller multicenter study that found aspirin intake to be independently associated with decreased risks of mechanical ventilation, ICU admission, and in-hospital mortality, investigators report in the International Journal of Cardiology.
 As virtual and augmented reality evolve into useful options in the cardiovascular field it will be important to ensure that these innovations are created in patients’ best interest and that they offer comparable or better care than what is available in real-world settings, according to a state-of-the-art paper published in JACC: Cardiovascular Imaging.
As virtual and augmented reality evolve into useful options in the cardiovascular field it will be important to ensure that these innovations are created in patients’ best interest and that they offer comparable or better care than what is available in real-world settings, according to a state-of-the-art paper published in JACC: Cardiovascular Imaging.
Body weight may influence QRS duration, a large ECG analysis suggests. Individuals with a body mass index (BMI) of 30 or higher had mean QRS durations of 88 ms compared with 82 ms and 86 ms for those with a BMI of 18.50-24.9 and 25-29.9, respectively. Reporting in IJC Heart & Vasculature, the Australian researchers say their findings should prompt more study into whether it is possible to reverse some conduction abnormalities through weight loss.
L.A. McKeown is a Senior Medical Journalist for TCTMD, the Section Editor of CV Team Forum, and Senior Medical…
Read Full Bio




Comments