PALACS: Posterior Left Pericardiotomy Cuts Postop AF After Cardiac Surgery
The single-center, proof-of-concept study sets the stage for a larger trial to quantify the potential benefit, Mario Gaudino says.

Performing a posterior left pericardiotomy during cardiac surgery appears to markedly reduce the risk of postoperative atrial fibrillation (AF), a stubbornly common and potentially serious complication, the single-center PALACS trial shows.
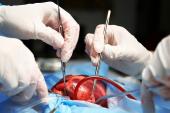
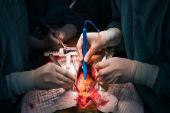
The procedure is relatively simple, involving a 4- to 5-cm incision in the posterior pericardium to allow drainage of fluid and clots from the pericardium to the left pleural cavity during the postoperative period, Mario Gaudino, MD, PhD (Weill Cornell Medicine, New York, NY), explained during his presentation at the virtual American Heart Association (AHA) 2021 Scientific Sessions.
In the trial, patients who received the incision during an operation on the coronary arteries, aortic valve, and/or ascending aorta had a significantly lower rate of postoperative AF compared with those who didn’t (17% vs 32%; RR 0.55; 95% CI 0.39-0.78), with no increase in perioperative complications, Gaudino reported.
“We believe that at this stage of knowledge, a large, pragmatic, confirmatory, multicenter trial that includes the entire spectrum of cardiac surgery operations is needed to quantify the potential clinical benefit of the intervention,” he said.
Commenting for TCTMD on the findings, which were published simultaneously online in the Lancet, Joseph Cleveland, MD (University of Colorado Medicine, Aurora), noted that aside from being a problem by increasing healthcare resource use, postoperative AF after cardiac surgery also has been associated with greater risks of stroke and mortality over the long term.
On that background, the PALACS results are intriguing, said Cleveland, chair of the American College of Cardiology’s Cardiac Surgery Team Council. He agreed that performing a posterior left pericardiotomy is relatively straightforward and is something most contemporary cardiac surgeons can do easily, adding that he doesn’t have any specific safety concerns with the technique.
The findings will have to be confirmed in a multicenter trial, Cleveland said, but PALACS “certainly is a very provocative and hypothesis-generating study that I think lends a simple intervention to reduce a complication after cardiac surgery that is prevalent and is serious.”
PALACS
Indeed, AF is the most common complication after cardiac surgery, reported in 20% to 40% of patients depending on the type of operation and the method of arrhythmia monitoring, Gaudino said. Postoperative pericardial effusion is frequently observed after surgery as well, and experimental studies indicate that even a small amount of effusion may trigger AF, possibly due to mechanical compression of the atria or local inflammation and oxidative stress, he added.
Prior smaller studies have explored posterior left pericardiotomy as a way to drain the pericardium and reduce postoperative AF, though the results have not been consistent. Thus, Gaudino said, the technique has not been widely adopted by surgeons.
PALACS is a single-center, single-blind trial that included adult patients with no history of arrhythmias undergoing elective operations on the coronary arteries, aortic valve, and/or ascending aorta; those undergoing mitral or tricuspid operations were excluded to reduce the heterogeneity of the population.
Investigators randomized 420 patients (mean age 61 years; 24% women) to receive a posterior left pericardiotomy as part of the operation or not. Mean CHA2DS2-VASc score was 2, with 37% of patients having a score of 3 or higher. Operations involved the aortic valve in 53% of cases, CABG in 45%, and the ascending aorta in 44%.
The reduction in postoperative AF—assessed using continuous cardiac rhythm monitoring during the postoperative in-hospital stay—observed in the pericardiotomy group was consistent across subgroups defined by age, sex, LVEF, CHA2DS2-VASc score, and type of surgery.
Among the secondary outcomes, pericardiotomy was associated with less need for postoperative antiarrhythmic medications (17% vs 31%; RR 0.55; 95% CI 0.38-0.79) and for systemic anticoagulation (6% vs 14%; RR 0.44; 95% CI 0.24-0.82). There were no differences between groups in the median length of the postoperative hospital stay (5 days in both groups) or of the total in-hospital stay (6 days in both groups).
Gaudino said there was no signal of risk related to the added incision, with no differences in operative mortality (1% in both arms); postoperative all-cause mortality, stroke, or MI (3% with pericardiotomy vs 2% without); or postoperative left pleural effusion (30% vs 32%). As expected, pericardiotomy was associated with a lower rate of postoperative pericardial effusion (12% vs 21%; RR 0.58; 95% CI 0.37-0.91).
More Research Needed
The trial was limited by the single-center design, the exclusion of mitral and tricuspid surgery, and the fact that it was not powered to detect differences in clinical events, Gaudino pointed out, saying that the findings need to be confirmed in additional studies.
Subodh Verma, MD, PhD (St. Michael’s Hospital, University of Toronto, Canada), discussing the results after Gaudino’s presentation, highlighted the key strengths of the trial—it provides the first surgical (as opposed to pharmacological) approach to reducing postoperative AF after cardiac surgery; it was adequately powered for the clinical outcome; the strategy tested was safe, with consistent results across subgroups; and it demonstrated a marked reduction in pericardial effusion.
But he also raised some questions related to the capture of only in-hospital postoperative AF, the liberal definition of AF (episodes lasting more than 30 seconds), the type of population enrolled, and the lack of subgroup analyses according to left atrial size and chest tube losses. There remains a question, Verma said, about whether a benefit similar to that seen in PALACS could be achieved with extended chest tube drainage after surgery.
Nonetheless, Verma said, “this is a well-conducted surgical trial that provides convincing proof of concept that a simple, inexpensive, generalizable, surgical adjunctive procedure of pericardial drainage can safely reduce postoperative atrial fibrillation after cardiac surgery.”
Asked about the mechanism of the effect, Gaudino said the most likely is related to relief of inflammation stemming from the drainage of clots and fluid from the pericardium, but he added that mechanistic analyses are ongoing.
While awaiting further data from this and any future studies, Cleveland suggested that at least some cardiac surgeons—himself included—will consider adding this technique in the types of patients included in PALACS. “This is a safe, relatively simple technical maneuver that holds promise to reduce the risk of postoperative atrial fibrillation after cardiac surgery in the population studied,” he said.
Todd Neale is the Associate News Editor for TCTMD and a Senior Medical Journalist. He got his start in journalism at …
Read Full BioSources
Gaudino M, Sanna T, Ballman KV, et al. Posterior left pericardiotomy for the prevention of atrial fibrillation after cardiac surgery: an adaptive, single-centre, single-blind, randomised, controlled trial. Lancet. 2021;Epub ahead of print.
Disclosures
- Gaudino and Verma report no relevant conflicts of interest.



Comments