Screening Programs for Abdominal Aortic Aneurysm Need a Rethink, Swedish Study Contends
As smoking rates have declined, so too has the mortality risk from AAA rupture. Are new randomized controlled trials of AAA screening needed?
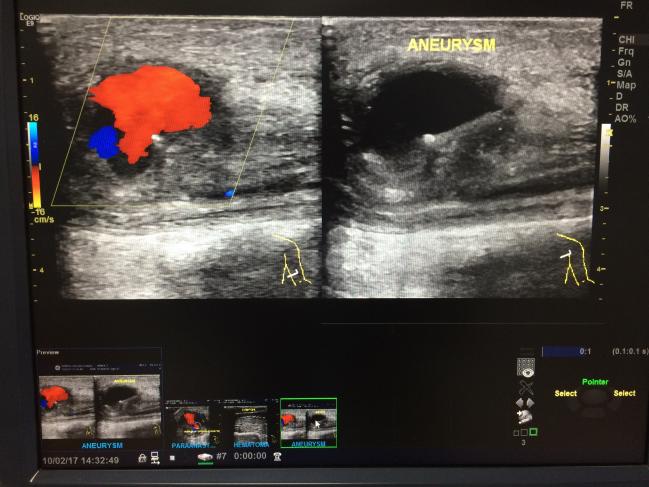
Population-based abdominal aortic aneurysm (AAA) screening programs may need a second look, based on dwindling returns and established harms, say the authors of a new registry-based cohort study. Their analysis of AAA mortality rates in Sweden over recent decades, as well as a comparison of men in regions with and without access to screening, call into question the value of population-wide screening programs for a condition that, today, so rarely ends in death.
“[Sweden’s] program was implemented based on evidence from randomized controlled trials that were performed in the 80s and 90s, and they showed a reduction in mortality from screening,” lead author Minna Johansson, MD (University of Gothenburg, Sweden), told TCTMD. “Since then there have been some studies showing that the incidence of AAA decreased by over 70%,” likely due to the decline in smoking. “When the incidence of the condition that we screen for decreases, then the benefit of screening also decreases, and theoretically, the balance between benefits and harms also becomes worse.”
Sweden, the United States, and the United Kingdom are among the countries that formally recommend AAA screening for men older than 65, although with different upper age limits and considerations. According to Kim Eagle, MD (University of Michigan, Ann Arbor), who commented on the study for TCTMD, these recommendations are based on 30 years of rigorous and thoughtful study. To use a retrospective review of claims data to challenge current screening programs, according to Eagle, is “difficult to swallow.”
“This won’t change my practice one bit, and to me it’s a bit alarming,” Eagle said.
Ultrasound Cheap, Everything That Follows Is Not
For their study, published in the June 16, 2018, issue of the Lancet, Johansson and colleagues analyzed AAA mortality between 1987 and 2015, and noted that in the latter half of this window rates decreased from 36 to 10 deaths per 100,000 men who were between the ages of 65 and 74.
The investigators also compared mortality rates between counties in Sweden where men had been invited to undergo screening with those where screening had not yet been offered. In this analysis, the reduction in AAA mortality after 6 years of screening was not statistically significant (adjusted OR 0.76; 95% CI 0.38–1.51) between jurisdictions. In other words, write the authors, for every 10,000 men screened, two men could be expected to avoid death.
Screening was, however, associated with a significant likelihood of AAA diagnosis and elective surgery such that for every 10,000 men offered screening, 49 were likely “overdiagnosed” and 19 would have had avoidable surgery.
“In my opinion, it's very doubtful that the benefits of AAA screening today compensate for the harms,” Johansson said.
The study did not consider the economic impact of screening—something Johansson said was by intent, since investigators wanted to focus specifically on the ethical question of the medical risk-benefit balance. To TCTMD, however, Johansson stressed that the economic questions should also be asked.
“Many people say, ‘Well, it's so cheap, you should just do the ultrasound,’ but that is of course not the problem. The ultrasound is cheap, it's everything that follows [that’s expensive].”
Moreover, the “huge” increase in elective surgeries is not offset by a reduction in emergency surgeries, she noted. There’s also the disproportionate allocation of human and healthcare resources, potentially depleting the ability of hospitals to offer other, more lifesaving procedures. “You could spend the money and the human resources in ways that would benefit public health much more.”
Smoking Rates, AAA Deaths Decline
Speaking with TCTMD, Eagle took issue with the study’s conclusions, especially the contention that screening had led to “excess” and harmful surgeries. Johansson et al’s analysis, he observed, did not provide detailed information on the type and size of aneurysms identified and how they were managed.
“There have been very good studies of people with known aneurysms showing that if you elect to intervene on aneurysms greater than 5.5 cm in men and a little smaller in women, that there is a relative reduction in mortality due to rupture as compared with the group you don’t operate on,” Eagle said. “That kind of information goes back a ways, so the authors of this [paper] would say, ‘If you get people to stop smoking, you manage their cholesterol and you manage their blood pressure, maybe they don’t rupture like they used to.’ But proving that can’t be established by claims data; that would require a randomized controlled trial.”
An accompanying editorial by Stefan Acosta, MD (Lund University, Malmö, Sweden), supports Johansson et al’s contention that a drop in smoking rates deserves much of the credit for falling AAA mortality rates. Acosta notes that smoking has been implicated in 75% of AAA cases and is eight times more common among people with AAA than among healthy controls. A 44% decline in smoking in Sweden since 1970 “should be viewed as the main cause of the decreasing incidence and mortality of AAA,” he writes. “Primary prevention programs to reduce the prevalence of tobacco smoking is a top priority, whereas screening for AAA is not,” he concludes.
Eagle, for his part, conceded that many of the pivotal studies in this field are outdated. “Maybe the time is right to do a carefully controlled, prospective, randomized study where you actually do this the right way, but it has to be done with forward-thinking in mind. Maybe the risk is so low in the population today that we should now only screen smokers with a big belly [in whom aneurysms cannot be manually palpated]. That might be true, but we haven’t studied it and we shouldn’t throw away everything we’ve come to believe about finding and treating AAAs based on a claims database study like this one.”
To TCTMD, Johansson stressed that any countries currently contemplating AAA screening recommendations should ensure that groups tasked with determining public policy include a broad range of perspectives.
“It should be a transparent council made up of people with no intellectual or financial conflicts of interests, from many different specialties,” she said.
A harder question is what to do in jurisdictions where screening is already in place, said Johansson, noting that she herself had “a harsh experience” when she publicly questioned screening programs. “It's very controversial, and once you implement a screening program, it's very hard to take it away,” she said. “People like it. It's very popular both among the public and among politicians, and also amongst doctors and healthcare personnel.”
It’s both “deeply human” and “a part of our culture” to want to know about disease risk and to act upon that information, she added. “In my experience, it's difficult to keep this [strictly] as a scientific debate.”
Shelley Wood was the Editor-in-Chief of TCTMD and the Editorial Director at the Cardiovascular Research Foundation (CRF) from October 2015…
Read Full BioSources
Johansson M, Zahl PH, Siersma V, et al. Benefits and harms of screening men for abdominal aortic aneurysm in Sweden: a registry-based cohort study. Lancet. 2018;391:2441-2447.
Acosta S. Screening men for AAA under magnification loupe in Sweden. Lancet. 2018;391:2394-2395.
Disclosures
- Johansson and Acosta report no relevant conflicts of interest.


Comments