Better Outcomes, Including Mortality, With IVUS-Guided PCI: Medicare Analysis
Uptake of IVUS remains low in the US, but experts say more positive trials with intracoronary imaging could nudge use higher.
“There was some debate about IVUS many years ago, but then randomized controlled trials came out, as well as other observational studies, to show that it is effective in optimizing post-PCI results, including stent deployment and the detection of complications,” lead researcher Amgad Mentias, MD (Cleveland Clinic, OH), told TCTMD. “That’s one of the reasons why we did our study. We wanted to see—across the nation in a Medicare population—how frequently hospitals are performing PCI guided by IVUS and to also see if the findings found in the randomized trials were generalizable to a wider population.”
In a propensity-matched analysis that included a broad population of patients, including those undergoing complex and less-complex PCI procedures as well as those with ACS and stable CAD, the risk of mortality at 30 days was significantly lower in patients treated with PCI guided by IVUS compared with those undergoing angiography-guided PCI (3.7% vs 4.3%; P < 0.01). At 1 year, 11.5% of patients undergoing PCI with IVUS had died compared with 12.3% of those in the non-IVUS group (P < 0.01).
The analysis was published August 18, 2020, in JACC: Cardiovascular Interventions.
Some might think it’ll just delay their procedures with little benefit to the patient. Amgad Mentias
Thomas Johnson, MBBS (University of Bristol, England), who coauthored an expert consensus statement from the European Association of Percutaneous Coronary Interventions on the use of intracoronary imaging, said that while the reduction in mortality, MI, and repeat revascularization seen with IVUS lines up with previously published data, he was especially struck by how infrequently IVUS was used. Overall, just 5.6% of 1,877,177 PCIs between 2009 and 2017 were performed with IVUS guidance, although there was a large variability in its use, with uptake increasing from 3.0% in 2009 to 6.9% in 2017.
“The really interesting aspect is: why [IVUS] isn’t picked up more and how do you persuade people?” said Johnson. “Clearly, the weakness is that there aren’t really compelling randomized controlled trials that provide the type of outcomes that this Medicare data does. Seeing a clear significant advantage in terms of mortality, revascularization, and MI is what will persuade physicians, but to date the only trial that has achieved that, in my mind, is ULTIMATE.”
Other large-scale intravascular imaging trials are underway, though. The largest, ILUMIEN IV, will compare clinical outcomes in high-risk patients (and those with high-risk lesions) who receive optical coherence tomography (OCT)-guided PCI against those undergoing standard PCI guided by angiography. The OCTOBER trial is also studying the use of OCT in the setting of complex bifurcation lesions, while the Korean RENOVATE trial will assess the clinical benefit of OCT and IVUS in complex procedures.
Broad Spectrum of Medicare Patients
In addition to mortality, the researchers looked other short-term outcomes as well as longer follow-up. At 1 year, the need for repeat revascularization was 6.1% and 6.7% in patients undergoing PCI with and without IVUS (P < 0.01), respectively, while the risk of MI also was lower in patients undergoing IVUS-guided PCI (4.9% vs 5.2%; P < 0.01).
In long-term follow-up (median 3.7 years), there were 82.8 deaths per 1,000 person-years in the IVUS-guided PCI group compared with 88.7 deaths in the non-IVUS group. At a median of 3 years, the MI event rate per 1,000 person-years of follow-up with and without IVUS was 33.5 and 35.8, respectively, while repeat revascularization rates were 35.8 and 39.9 per 1,000 person-years of follow-up. Despite the small absolute reductions in outcomes, all differences were statistically significant (P < 0.001).
IVUS was more likely to be used in patients with comorbidities, including heart failure, prior coronary artery disease, prior stroke, chronic kidney disease, chronic lung disease, and pulmonary hypertension. Complex cases were also more likely to see IVUS used, and these patients had more stents placed and more vessels treated, as well as a higher prevalence of bifurcation and chronic total occlusion (CTO) lesions.
Mentias said IVUS-guided PCI tends to be more frequently used in complex cases where physicians are worried about postintervention complications. Their data, however, showed IVUS was associated with a significantly lower risk of long-term mortality, MI, and repeat revascularization when the analysis was performed separately in patients undergoing complex PCI and those undergoing less complex procedures. The benefit of IVUS was also observed in patients with ACS or stable CAD as well as in those who received BMS or DES.
“Across the study subgroups, IVUS was consistently associated with a benefit and reduced mortality in the long term,” said Mentias.
While he doesn’t predict IVUS will be universally adopted for all cases, Mentias said it should be used more frequently in the US, particularly in complex PCIs. “And you know, right now complex cases make up at least 50% of PCI volume at different institutions,” said Mentias. “Complex interventions are much more common than they were before. So, I think in complex interventions IVUS should be routinely used to make sure that the poststenting result is optimized and the patient doesn’t end up with a suboptimal result before leaving the cath lab.”
Johnson agreed that IVUS or OCT is not justified in all patients undergoing PCI given the cost and time required. “However, the complexity of work is increasing all the time,” he said. “I think for all complex cohorts, the penetration should be much, much higher. CTO operators have embraced that well. Certainly for us, complex CTO is done pretty much 100% of the time with image guidance.”
At present, use of IVUS for the assessment of non-left main CAD is a Class IIb recommendation from the American College of Cardiology/American Heart Association and a IIa recommendation from the European Society of Cardiology. In an editorial, Lorenz Räber, MD, PhD and Yasushi Ueki, MD (both from Bern University Hospital, Switzerland), point out that ULTIMATE—a 1,448-patient trial that showed IVUS-guided PCI with contemporary DES translated into a significant reduction in target vessel failure at 1 year—was considered an all-comers study, but the majority of patients enrolled were considered complex.
For this reason, a broader recommendation on the use of IVUS, including noncomplex lesions, remains debatable. Nonetheless, like Mentias and Johnson, they believe the “niche-like” adoption rate seen in the US and elsewhere should be improved. In Japan and Korea, the uptake of IVUS is extremely high, they note.
Why Isn’t IVUS Used More Often?
Although the study was not designed to assess why IVUS uptake remains low, Mentias said there are several potential reasons, including cost relative to reimbursement. However, he noted that a recent economic analysis suggested that adding IVUS to PCI was a cost-effective strategy when used in higher-risk patients. Beyond its price tag, a lack of expertise or experience with IVUS might explain its relatively infrequent use. Physicians might not be comfortable obtaining the images or interpreting the results, he said.
“It could also be that people don’t believe the randomized, controlled findings wouldn’t stand up in the real world,” said Mentias. “Some might think it’ll just delay their procedures with little benefit to the patient.”
Johnson believes cost and time are excuses. Instead, he said, the low penetration rate is likely the result of interventionalists not being comfortable interpreting the technology and/or making decisions based on the image. Such decisions, which include choosing the appropriate stent size and length, as well as the assessment of tissue morphology, can be quite nuanced with IVUS and can “put people off because it’s quite a hard thing to learn—it takes a lot of time and energy,” said Johnson. At the moment, OCT is a little more user-friendly, with automated software that aids in image interpretation.
I think for all complex cohorts, the penetration should be much, much higher. Thomas Johnson
One drawback of the current study is that the Medicare data provide little insight into why or how IVUS was used during PCI, said Johnson.
“Anecdotally, if you look at how imaging is taken, it’s reactionary,” he said. “You’re taking it at a point where you’ve either had a complication or something doesn’t look right on the angiogram. So those cases are weighted against imaging, because you’re taking complex or complicated cases and still demonstrating a benefit in outcomes. You’d really hope that in a clean, randomized, prospective study you’d see an even greater gain with imaging. That’s the hope with ILUMIEN IV.”
Ideally, IVUS or OCT should be used to guide the entire procedure, as opposed to casting a backward look to determine that a stent was optimally placed, added Johnson. “If possible, the imaging probe should be used from the very beginning to the end of the procedure, so that you understand the disease that you’re treating before you deploy the stent and then you ensure once you selected the appropriate stent you’ve optimized its placement.”
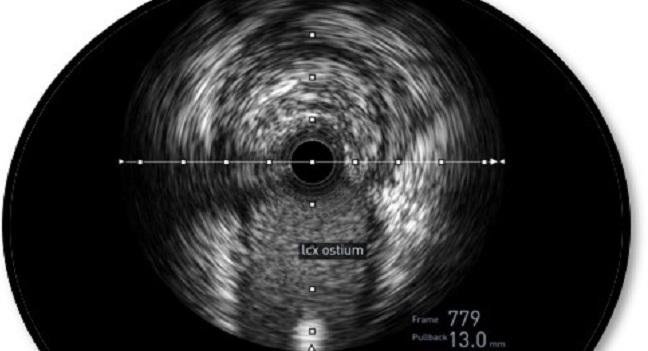
Photo Credit: Adapted from Bhattacharya DD. IVUS: Its Present Roles and Advantages. Presented at TCT 2019. September 28, 2019. San Francisco, CA.
Michael O’Riordan is the Managing Editor for TCTMD. He completed his undergraduate degrees at Queen’s University in Kingston, ON, and…
Read Full BioSources
Mentias A, Sarrazin MV, Saad M, et al. Long-term outcomes of coronary stenting with and without use of intravascular ultrasound. J Am Coll Cardiol Intv. 2020;13:1880-1890.
Räber L, Ueki Y. Outcomes of intravascular ultrasound-guided percutaneous coronary intervention in the United States. J Am Coll Cardiol Intv. 2020;13:1891-1893.
Disclosures
- Mentias reports grant support from National Institutes of Health paid to the Abboud Cardiovascular Research Center.
- Räber reports institutional research grant support from Abbott Vascular, Biotronik, Boston Scientific, Heart- Flow, Sanofi, and Regeneron; he reports speaking/consulting fees from Abbott Vascular, Amgen, AstraZeneca, Canon, CSL Behring, Occlutech, Sanofi, and Vifor.
- Ueki reports travel grants from Infraredx.
- Johnson reports personal fees from Boston Scientific, Terumo, Abbott Vascular, Daiichi Sankyo, and AstraZeneca.


Comments