COVID-19: TCTMD’s Dispatch for May Week 4
We’re curating a list of COVID-19 research and other useful content, and updating it regularly.

Since March 2020, TCTMD reporter Todd Neale has been writing up breaking news and peer-reviewed research related to COVID-19 every weekday. In July 2021, we transitioned to Mondays, Wednesdays, and Fridays. If you have something to share, tell us. All of our COVID-19 coverage can be found on our COVID-19 Hub.
May 26, 2022
 Though some parts of the world continue to deal with rising COVID-19 numbers, including the Americas and the Western Pacific region, cases have again started to decline from a global perspective after a week of stabilization, according to the latest update from the World Health Organization (WHO). New cases fell 3% from the prior week, with an 11% reduction in new deaths. CIDRAP News has more.
Though some parts of the world continue to deal with rising COVID-19 numbers, including the Americas and the Western Pacific region, cases have again started to decline from a global perspective after a week of stabilization, according to the latest update from the World Health Organization (WHO). New cases fell 3% from the prior week, with an 11% reduction in new deaths. CIDRAP News has more.
Earlier this week, the US Centers for Disease Control and Prevention (CDC) issued an alert regarding the potential for “COVID-19 rebound” after treatment with Pfizer’s oral antiviral therapy Paxlovid. The agency maintains its recommendation to use the therapy for patients with mild-to-moderate COVID-19 who are at risk for progression to severe disease, but newly advises patients with a rebound to re-isolate for at least 5 days and wear a mask for 10 days after the start of rebound symptoms. A STAT story discusses the efforts going into uncovering the reasons for the rebound phenomenon.
Taiwan, which managed to limit the number of locally transmitted COVID-19 cases to less than 15,000 for all of 2021, is now seeing about 80,000 cases each day as it eases restrictions with an eye on living with the virus, a Reuters article notes. “Unlike some countries where new case spikes overwhelmed medical systems and disrupted everyday life, Taiwan hospital beds earmarked for COVID patients are at 56% occupancy. Shops, restaurants, and gyms remain open, and gatherings continue, with mandatory mask-wearing.”
Full vaccination is associated with less secondary transmission of COVID-19 and a shorter duration of viable viral shedding compared with partial or no vaccination, according to a study in JAMA Network Open. That provides “important evidence that despite the possibility of breakthrough infections, COVID-19 vaccinations remain critically useful for controlling the spread of SARS-CoV-2,” the authors say. A commentary delves into the implications.
 Sweden is recommending a fifth COVID-19 shot for people older than 65 and others deemed to be at risk for serious illness, including pregnant women, those who are immunocompromised, and patients with heart and lung disease, the Associated Press reports. The policy takes effect September 1.
Sweden is recommending a fifth COVID-19 shot for people older than 65 and others deemed to be at risk for serious illness, including pregnant women, those who are immunocompromised, and patients with heart and lung disease, the Associated Press reports. The policy takes effect September 1.
Some studies have suggested that COVID-19 vaccination not only protects against severe outcomes from acute SARS-CoV-2 infection, but also limits long COVID symptoms months later. A new study in Nature Medicine, however, indicates that protection against long COVID is not absolute—vaccinated people with breakthrough infections still had an elevated risk of postacute sequelae, though it was lower than that seen in unvaccinated individuals. “Altogether, the findings suggest that vaccination before infection confers only partial protection in the postacute phase of the disease; hence, reliance on it as a sole mitigation strategy may not optimally reduce long-term health consequences of SARS-CoV-2 infection,” the researchers write. The findings are disappointing, the lead author told the Washington Post.
A study from CDC researchers, published in Morbidity and Mortality Weekly Report, provides some insights into the occurrence of post-COVID conditions up to a year after the initial infection, showing that about one in five people ages 18 to 64 and one in four people 65 and older had at least one condition that could be linked to COVID-19. The greatest risks were seen for acute pulmonary embolism and respiratory signs or symptoms. Here’s more from the New York Times.
Another study, this one in the Annals of Clinical and Translational Neurology, indicates that a subset of patients who were not hospitalized for COVID-19 can have neurologic symptoms, fatigue, and compromised quality of life that lasts more than a year after the initial infection. At a median follow-up of 14.8 months, a range of symptoms that included “brain fog,” numbness/tingling, headache, dizziness, blurred vision, tinnitus, and fatigue remained prevalent. Vaccination did not have an impact on cognitive function or fatigue.
Though a fourth dose of the Pfizer/BioNTech vaccine gives added protection against SARS-CoV-2 infection and severe COVID-19 compared with three doses in people 60 and older, its effects fade faster than those seen with a third dose, researchers report in the BMJ. Effectiveness against infection peaked 3 weeks after administration of the fourth dose (at 65.1%), falling to just 22.0% by 10 weeks.
 Long-term exposure to air pollution, particularly ground-level ozone, is associated with greater risks of hospitalization, ICU admission, and death among patients with COVID-19, according to a study in CMAJ. “However,” the authors say, “uncertainty still remains in the mechanisms of how long-term air pollution might affect COVID-19 severity, which calls for future research.”
Long-term exposure to air pollution, particularly ground-level ozone, is associated with greater risks of hospitalization, ICU admission, and death among patients with COVID-19, according to a study in CMAJ. “However,” the authors say, “uncertainty still remains in the mechanisms of how long-term air pollution might affect COVID-19 severity, which calls for future research.”
May 23, 2022
According to the latest numbers from the US Centers for Disease Control and Prevention (CDC), released late last week, most Americans live in areas with low levels of COVID-19, although many parts of the country have moved into medium and high levels. The 7-day average of new cases increased by 18.8% compared with the prior period, with hospitalizations up 24.2%. The average of new deaths declined slightly, by 1.2%.
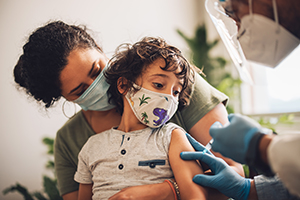 Pfizer and BioNTech said Monday that a third, 3-µg dose of their COVID-19 vaccine elicited “a strong immune response, with a favorable safety profile” in children ages 6 months to under 5 years in a phase II/III trial. Vaccine efficacy, a secondary endpoint, was 80.3% at a time when the Omicron variant was dominant. “These top-line safety, immunogenicity, and efficacy data are encouraging, and we look forward to soon completing our submissions to regulators globally with the hope of making this vaccine available to younger children as quickly as possible, subject to regulatory authorization,” said Albert Bourla, Pfizer’s chairman and CEO. US Food and Drug Administration (FDA) advisors will meet June 14 and 15 to discuss the use of this vaccine and the one from Moderna in young children (Reuters).
Pfizer and BioNTech said Monday that a third, 3-µg dose of their COVID-19 vaccine elicited “a strong immune response, with a favorable safety profile” in children ages 6 months to under 5 years in a phase II/III trial. Vaccine efficacy, a secondary endpoint, was 80.3% at a time when the Omicron variant was dominant. “These top-line safety, immunogenicity, and efficacy data are encouraging, and we look forward to soon completing our submissions to regulators globally with the hope of making this vaccine available to younger children as quickly as possible, subject to regulatory authorization,” said Albert Bourla, Pfizer’s chairman and CEO. US Food and Drug Administration (FDA) advisors will meet June 14 and 15 to discuss the use of this vaccine and the one from Moderna in young children (Reuters).
Excess mortality related to COVID-19 in Massachusetts was actually higher when Omicron was the dominant variant than when Delta was widely circulating, despite reports that Omicron presents less risk, researchers report in JAMA. “The present findings indicate that a highly contagious (although relatively milder) SARS-CoV-2 variant can quickly confer substantial excess mortality, even in a highly vaccinated and increasingly immune population,” they say.
Over the course of the pandemic, COVID-19-related mortality has continued to fall among older individuals, with particularly large declines in death rates in those 80 and older, according to a study in JAMA Network Open. In contrast, mortality increased over time among younger adults. “Possible factors underpinning these changing patterns are higher vaccination prevalence and less exposure to infection among older individuals,” the authors suggest. “This advantage may have increased over time as younger individuals returned to work and other activities and the Delta variant emerged.”
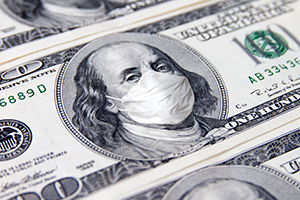 The COVID-19 pandemic did not drive up medical debt among Americans, an analysis of credit reports in JAMA Health Forum suggests. “We found no evidence of a net association between the COVID-19 pandemic and medical debt, overall or across areas with different incomes and pandemic severity. These results are consistent with any increase in medical debt being offset by decreases in elective medical procedures and new healthcare-related governmental policies,” the authors write.
The COVID-19 pandemic did not drive up medical debt among Americans, an analysis of credit reports in JAMA Health Forum suggests. “We found no evidence of a net association between the COVID-19 pandemic and medical debt, overall or across areas with different incomes and pandemic severity. These results are consistent with any increase in medical debt being offset by decreases in elective medical procedures and new healthcare-related governmental policies,” the authors write.
Over the weekend, the New York Times released a story delving into what’s known about long COVID, or postacute sequelae of COVID-19 (PASC), including discussions around diagnosis, risk factors, the impact of vaccination, and medical care. Studies estimate that 10% to 30% of people report medical issues months after the initial infection. “Such lingering medical issues are so varied that one study by a patient-led research group evaluated 203 symptoms that may fluctuate or even appear out of the blue after people seem to have recovered,” the article notes.
People with low body weight have less waning of COVID-19 vaccine immunity 6 months after receipt of two doses of the Pfizer/BioNTech shot, according to a study in JAMA Network Open. The researchers conclude: “A booster shot . . . may be given later than 6 months after the second dose in young and middle-aged healthy persons with low body weight.” CIDRAP News has more.
A study out of Israel, published in JAMA, indicates that the severity of multisystem inflammatory syndrome in children (MIS-C) associated with SARS-CoV-2 infection was reduced when Omicron was circulating. “Possible explanations include the Omicron variant itself, previous infection with SARS-CoV-2, vaccination against SARS-CoV-2, and improvement in treatment over time,” its authors note.
 A study published last week in Psychological Medicine shows that depression, worry about COVID-19, and loneliness prior to SARS-CoV-2 infection are associated with a greater risk of hospitalization for COVID-19. “Assessment of psychological distress may identify patients at greater risk of hospitalization,” the researchers say. “Future work should examine whether addressing distress improves physical health outcomes.”
A study published last week in Psychological Medicine shows that depression, worry about COVID-19, and loneliness prior to SARS-CoV-2 infection are associated with a greater risk of hospitalization for COVID-19. “Assessment of psychological distress may identify patients at greater risk of hospitalization,” the researchers say. “Future work should examine whether addressing distress improves physical health outcomes.”
Todd Neale is the Associate News Editor for TCTMD and a Senior Medical Journalist. He got his start in journalism at …
Read Full Bio




Comments